The authors thank the North Carolina Department of Labor for permission to re-use materials developed during the writing of an NCDOL industry guide on hearing conservation.
The primary objective of occupational hearing conservation programmes (HCPs) is to prevent on-the-job noise-induced hearing loss due to hazardous workplace noise exposures (Royster and Royster 1989 and 1990). However, the person—who shall later be characterized as the “key individual”—who is responsible for making the HCP effective should use common sense to modify these practices to fit the local situation in order to achieve the desired goal: protection of workers from harmful occupational noise exposures. A secondary objective of these programmes should be to so educate and motivate individuals that they also elect to protect themselves from harmful non-occupational noise exposures and translate their knowledge about hearing conservation to their families and friends.
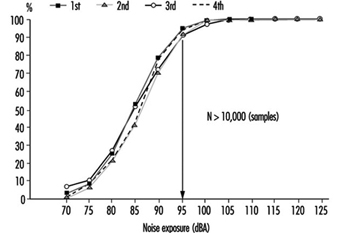
Figure 1 shows the distributions of over 10,000 noise exposure samples from four sources in two countries, including a variety of industrial, mining and military work environments. The samples are 8-hour time-weighted-average values based on exchange rates of 3, 4 and 5 dB. These data indicate that about 90% of daily equivalent noise exposures are 95 dBA or below, and only 10% exceed 95 dBA.
Figure 1. Estimated noise exposure hazard for different populations
The importance of the data in figure 1, assuming that they apply to most countries and populations, is simply that a vast majority of noise-exposed employees need to achieve only 10 dBA of protection from noise to eliminate the hazard. When hearing protection devices (HPDs) are worn to achieve this protection, those responsible for worker health must take the time to fit each individual with a device that is comfortable, practical for the environment, takes into account the individual’s auditory needs (ability to hear warning signals, speech, etc.), and provides an acoustic seal when worn day in and day out in real-world environments.
This article presents a condensed set of good hearing conservation practices, as summarized in the checklist presented in figure 2.
Figure 2. Checklist of good HCP practices
Benefits of Hearing Conservation
Prevention of occupational hearing loss benefits the employee by preserving hearing abilities which are critical to good quality of life: interpersonal communication, enjoyment of music, detection of warning sounds, and many more. The HCP provides a health screening benefit, since non-occupational hearing losses and potentially treatable ear diseases are often detected through annual audiograms. Lowering noise exposure also reduces potential stress and fatigue related to noise.
The employer benefits directly by implementing an effective HCP which maintains employees’ good hearing, since workers will remain more productive and more versatile if their communication abilities are not impaired. Effective HCPs can reduce accident rates and promote work efficiency.
Phases of an HCP
Refer to the checklist in the figure 2 for details of each phase. Different personnel may be responsible for different phases, and these personnel comprise the HCP team.
Sound exposure surveys
Sound level meters or personal noise dosimeters are used to measure workplace sound levels and estimate workers’ noise exposures to determine if an HCP is needed; if so, the data so gathered will help establish appropriate HCP policies to protect employees (Royster, Berger and Royster 1986). Survey results identify which employees (by department or job) will be included in the HCP, which areas should be posted for required hearing protector use, and which hearing protection devices are adequate. Adequate samples of representative production conditions are needed to classify exposures into ranges (below 85 dBA, 85-89, 90-94, 95-99 dBA, etc.). The measurement of A-weighted sound levels during the general noise survey often identifies dominant noise sources in areas of the plant where follow-up engineering noise control studies may significantly reduce employee exposures.
Engineering and administrative noise controls
Noise controls may reduce employees’ noise exposures to a safe level, eliminating the need for a hearing conservation programme. Engineering controls (see “Engineering noise control” [NOI03AE] in this chapter) involve modifications of the noise source (such as fitting mufflers to air exhaust nozzles), the noise path (such as placing sound-blocking enclosures around equipment) or the receiver (such as constructing an enclosure around the employee’s workstation). Worker input is often needed in designing such modifications to ensure that they are practical and will not interfere with his or her tasks. Obviously, hazardous employee noise exposures should be reduced or eliminated by means of engineering noise controls whenever practical and feasible.
Administrative noise controls include replacement of old equipment with quieter new models, adherence to equipment maintenance programmes related to noise control, and changes in employee work schedules to reduce noise doses by limiting exposure time when practical and technically advisable. Planning and designing to achieve non-hazardous noise levels when new production facilities are brought on-line is an administrative control which can also eliminate the need for an HCP.
Education and motivation
HCP team members and employees will not actively participate in hearing conservation unless they understand its purpose, how they will benefit directly from the programme, and that compliance with the company’s safety and health requirements is a condition of employment. Without meaningful education to motivate individual actions, the HCP will fail (Royster and Royster 1986). Topics to be covered should include the following: the purpose and benefits of the HCP, sound survey methods and results, using and maintaining engineering noise control treatments to reduce exposures, hazardous off-the-job noise exposures, how noise damages hearing, consequences of hearing loss in daily life, selection and fitting of hearing protection devices and importance of consistent wear, how audiometric testing identifies hearing changes to indicate the need for greater protection and the employer’s HCP policies. Ideally, these topics can be explained to small groups of employees in safety meetings, given ample time for questions. In effective HCPs the educational phase is a continuous process—not just an annual presentation—as HCP personnel take daily opportunities to remind others about conserving their hearing.
Hearing protection
The employer provides hearing protection devices (earplugs, earmuffs, and semi-insert devices) for employees to wear as long as hazardous noise levels exist in the workplace. Because feasible engineering noise controls have not been developed for many types of industrial equipment, hearing protectors are the best current option for preventing noise-induced hearing loss in these situations. As indicated earlier, most noise-exposed workers need to achieve only 10 dB of attenuation to be adequately protected from noise. With the large selection of hearing protectors available today, adequate protection can be readily achieved (Royster 1985; Royster and Royster 1986) if devices are individually fitted to each employee to achieve an acoustic seal with acceptable comfort, and if the worker is taught how to wear the device correctly to maintain an acoustic seal, but consistently whenever a noise hazard exists.
Audiometric evaluations
Each exposed individual should receive a baseline hearing check followed by annual rechecks to monitor hearing status and detect any hearing change. An audiometer is used in a sound-attenuating booth to test the employee’s hearing thresholds at 0.5, 1, 2, 3, 4, 6 and 8 kHz. If the HCP is effective, employees’ audiometric results will not show significant changes associated with on-the-job noise-induced hearing damage. If suspicious hearing changes are found, the audiometric technician and the audiologist or physician who reviews the record can counsel the employee to wear HPDs more carefully, assess whether better-fitting HPDs are needed and motivate the individual to be more careful in protecting his or her hearing both on and off the job. Sometimes non-occupational causes of hearing change may be identified, such as gunfire or hobby noise exposure, or medical ear problems. Audiometric monitoring is useful only if quality control of testing procedures is maintained and if the results are used to trigger follow-up for individuals with significant hearing changes (Royster 1985).
Record Keeping
Requirements for the type of records to be kept and the duration for maintaining them vary among countries. In countries where litigation concerns and worker’s compensation are important issues, records should be maintained longer than required by occupational regulations since they are often useful for legal purposes. The goal of record keeping is to document how employees have been protected from noise (Royster and Royster 1989 and 1990). Especially important records include the sound survey procedures and findings, audiometric calibration and results, follow-up actions in response to employees’ hearing changes and documentation of hearing protector fitting and training. Records should include the names of the personnel who carried out the HCP tasks as well as the results.
Programme Evaluation
Characteristics of effective programmes
Successful HCPs share the following characteristics and promote a “safety culture” with respect to all safety programmes (safety eyeglasses, “hard hats”, safe lifting behaviour, etc.).
The “key individual”
The most important strategy for making the five phases of the HCP function together effectively is to unite them under the supervision of one individual of central importance (Royster and Royster 1989 and 1990). In smaller companies where one person may actually carry out all facets of the HCP, lack of coordination is not usually a problem. However, as the size of the organization increases, different types of staff become involved in the HCP: safety personnel, medical personnel, engineers, industrial hygienists, tool crib supervisors, production supervisors and others. With personnel from varying disciplines carrying out different aspects of the programme, it becomes very difficult to coordinate their efforts unless one “key individual” is able to oversee the entire HCP. The choice of who this person should be is critical to the success of the programme. One of the primary qualifications for the key individual is genuine interest in the company’s HCP.
The key individual is always approachable and is sincerely interested in comments or complaints that can help to improve the HCP. This individual does not take a remote attitude or stay in an office, running the HCP on paper by mandate, but spends time on the production floors or wherever workers are active in order to interact with them and observe how problems can be prevented or solved.
Active communications and roles
The primary HCP team members should meet together regularly to discuss the progress of the programme and ensure that all duties are being carried out. Once people with different tasks understand how their own roles contribute to the overall outcome of the programme, they will cooperate better to prevent hearing loss. The key individual can achieve this active communication and cooperation if management provides him or her with the authority to make HCP decisions and the resource allocations to act on decisions once they are made. The success of the HCP depends on everyone from the top boss to the most recently hired trainee; everyone has an important role. Management’s role is largely to support the HCP and enforce its policies as one facet of the company’s overall health and safety programme. For middle managers and supervisors the role is more direct: they help carry out the five phases. The role of employees is to participate actively in the programme and be aggressive in making suggestions to improve HCP operation. However, for employee participation to succeed, management and the HCP team must be receptive to comments and actually respond to employee input.
Hearing protectors—effective and enforced
The importance of hearing protection policies to HCP success is underscored by two desired characteristics of effective HCPs: strict enforcement of hearing protector utilization (there must be actual enforcement, not just a paper policy) and the availability of protectors which are potentially effective for use by the wearers in the work environment. Potentially effective devices are practical and comfortable enough for employees to wear consistently, and they provide adequate sound attenuation without impairing communication through overprotection.
Limited external influences on the HCP
If local HCP decisions are limited by policies mandated by corporate headquarters, the key individual may need top management’s assistance in obtaining exceptions to the corporate or external rules in order to meet local needs. The key individual also must keep strict control over any services provided by outside consultants, contractors or government officials (such as sound surveys or audiograms). When contractors are used, it is more difficult to integrate their services cohesively into the overall HCP, but it is critical to do so. If in-plant personnel do not follow through by using the information provided by the contractors, then the contracted elements of the programme lose effectiveness. Experience clearly indicates that it is very difficult to establish and maintain an effective HCP which depends predominantly on external contractors.
In contrast to the previous characteristics, the following is a listing of some common causes of HCP ineffectiveness.
- inadequate communication and coordination among HCP personnel
- insufficient or erroneous information used to make decisions
- inadequate training for hearing protector fitters and issuers
- inadequate or inappropriate selection of protectors in stock
- over-reliance on number ratings in choosing devices
- failure to fit and train each HPD wearer individually
- over-reliance on external sources (government or contractors) to provide HCP services
- failure to use audiometric monitoring results to educate and motivate employees
- failure to use audiometric data to evaluate HCP effectiveness.
Objective evaluation of the audiometric data
The audiometric data for the noise-exposed population provide evidence of whether the HCP is preventing occupational hearing loss. Over time, the rate of hearing change for noise-exposed employees should be no greater than that of matched controls without noisy jobs. To give an early indication of HCP effectiveness, procedures for audiometric database analysis have been developed using year-to-year variability in threshold values (Royster and Royster 1986; ANSI 1991).