Children categories

1. Blood (3)

1. Blood
Chapter Editor: Bernard D. Goldstein
Table of Contents
Tables
Haematopoietic and Lymphatic System
Bernard D. Goldstein
Leukaemia, Malignant Lymphomas and Multiple Myeloma
Timo Partanen, Paolo Boffetta, Elisabete Weiderpass
Agents or Work Conditions Affecting the Blood
Bernard D. Goldstein
Tables
Click a link below to view the table in the article context.

2. Cancer (4)

2. Cancer
Chapter Editor: Paolo Boffetta
Table of Contents
Tables
Introduction
Neil Pearce, Paolo Boffetta and Manolis Kogevinas
Occupational Carcinogens
Paolo Boffetta, Rodolfo Saracci, Manolis Kogevinas, Julian Wilbourn and Harri Vainio
Environmental Cancer
Bruce K. Armstrong and Paolo Boffetta
Prevention
Per Gustavsson
Tables
Click a link below to view table in article context.
- Occupational cancer: Key facts
- Estimated proportions of cancer (PAR) attributable to occupations
- Evaluation of evidence of carcinogenicity in the IARC Monographs
- IARC Monograph programme classification groups
- Group 1-Chemicals carcinogenic to humans
- Group 2A—Chemicals probably carcinogenic to humans
- Group 2B—Chemicals possibly carcinogenic to humans
- Pesticides evaluated in IARC Monographs, Volumes 1-63 (1972-1995)
- Drugs evaluated in IARC Monographs, Volumes 1-63 (1972-1995)
- Environmental agents/exposures known or suspected of human cancer
- Industries, occupations, exposures presenting a carcinogenic risk
- Industries, occs., exps. with cancer excess not definitive carcinogens
- Registered population variations of incidence of some common cancers

3. Cardiovascular System (7)

3. Cardiovascular System
Chapter Editors: Lothar Heinemann and Gerd Heuchert
Table of Contents
Tables and Figures
Introduction
Lothar Heinemann and Gerd Heuchert
Cardiovascular Morbidity and Mortality in the Workforce
Gottfried Enderlein and Lothar Heinemann
The Risk Factor Concept in Cardiovascular Disease
Lothar Heinemann, Gottfried Enderlein and Heide Stark
Rehabilitation and Prevention Programmes
Lothar Heinemann and Gottfried Enderlein
Physical, Chemical and Biological Hazards
Physical Factors
Heide Stark and Gerd Heuchert
Chemical Hazardous Materials
Ulrike Tittelbach and Wolfram Dietmar Schneider
Biological Hazards
Regina Jäckel, Ulrike Tittelbach and Wolfram Dietmar Schneider
Tables
Click a link below to view table in article context
- Mortality from cardiovascular diseases
- Mortality rates, special cardiovascular diagnosis groups
- Rate of disease and reduced work ability
- Work associated with cardiovascular hazards
- Occupation-related infection and disease
Figures
Point to a thumbnail to see figure caption, click to see the figure in the article context.

4. Digestive System (6)

4. Digestive System
Chapter Editor: Heikki Savolainen
Table of Contents
Figures
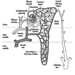
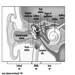
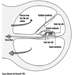
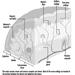
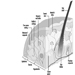
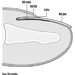
Digestive system
G. Frada
Mouth and teeth
F. Gobbato
Liver
George Kazantzis
Peptic ulcer
K. S. Cho
Liver cancer
Timo Partanen, Timo Kauppinen, Paolo Boffetta and Elisabete Weiderpass
Pancreatic cancer
Timo Partanen, Timo Kauppinen, Paolo Boffetta and Elisabete Weiderpass
Figures
Point to a thumbnail to see figure caption, click to see figure in article context.

5. Mental Health (8)

5. Mental Health
Chapter Editors: Joseph J. Hurrell, Lawrence R. Murphy, Steven L. Sauter and Lennart Levi
Table of Contents
Tables and Figures
Work and Mental Health
Irene L.D. Houtman and Michiel A.J. Kompier
Work-related Psychosis
Craig Stenberg, Judith Holder and Krishna Tallur
Mood and Affect
Depression
Jay Lasser and Jeffrey P. Kahn
Work-related Anxiety
Randal D. Beaton
Post-traumatic Stress Disorder and its Relationship to Occupational Health and Injury Prevention
Mark Braverman
Stress and Burnout and their Implication in the Work Environment
Herbert J. Freudenberger
Cognitive Disorders
Catherine A. Heaney
Karoshi: Death from Overwork
Takashi Haratani
Tables
Click a link below to view table in article context.
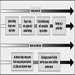
1. Schematic overview of management strategies & examples
Figures
Point to a thumbnail to see figure caption, click to see figure in article context.

6. Musculoskeletal System (14)

6. Musculoskeletal System
Chapter Editors: Hilkka Riihimäki and Eira Viikari-Juntura
Table of Contents
Tables and Figures
Overview
Hilkka Riihimäki
Muscles
Gisela Sjøgaard
Tendons
Thomas J. Armstrong
Bones and Joints
David Hamerman
Intervertebral Discs
Sally Roberts and Jill P.G. Urban
Low-back Region
Hilkka Riihimäki
Thoracic Spine Region
Jarl-Erik Michelsson
Neck
Åsa Kilbom
Shoulder
Mats Hagberg
Elbow
Eira Viikari-Juntura
Forearm, Wrist and Hand
Eira Viikari-Juntura
Hip and Knee
Eva Vingård
Leg, Ankle and Foot
Jarl-Erik Michelsson
Other Diseases
Marjatta Leirisalo-Repo
Tables
Click a link below to view table in article context.
- Structure-function of joint components
- Prevalence of back disorders, in Finns over 30 years
- Reducing the risks for low-back pain at work
- Classification-low-back disorders (Quebec Task Force)
- Permissible motions for head in prolonged driving
- Incidence of epicondylitis in various populations
- Incidence of tenosynovitis/peritendinitis
- Primary osteoarthrosis of the hip in Malmö, Sweden
- Guidelines for the treatment of rheumatoid arthritis
- Infections known to trigger reactive arthritis
Figures
Point to a thumbnail to see figure caption, click to see figure in article context.

7. Nervous System (9)

7. Nervous System
Chapter Editor: Donna Mergler
Table of Contents
Tables and Figures
Nervous System: Overview
Donna Mergler and José A. Valciukas
Anatomy and Physiology
José A. Valciukas
Chemical Neurotoxic Agents
Peter Arlien-Søborg and Leif Simonsen
Manifestations of Acute and Early Chronic Poisoning
Donna Mergler
Preventing Neurotoxicity at Work
Barry Johnson
Clinical Syndromes Associated with Neurotoxicity
Robert G. Feldman
Measuring Neurotoxic Deficits
Donna Mergler
Diagnosis
Anna Maria Seppäläinen
Occupational Neuroepidemiology
Olav Axelson
Tables
Click a link below to view table in article context.
- Names & main functions of each pair of cranial nerves
- Grouping neurotoxic effects as to neurotoxicity
- Gases associated with neurotoxic effects
- Neurotoxic metals & their inorganic compounds
- Neurotoxic monomers
- Organic solvents associated with neurotoxicity
- Classes of common neurotoxic pesticides
- Other chemicals associated with neurotoxicity
- Chronic symptoms checklist
- Neuro-functional effects of exposures to some neurotoxins
- Chemical exposures & associated neurotoxic syndromes
- Some “core” batteries for assessing early neurotoxic effects
- Decision tree for neurotoxic disease
- Consistent neuro-functional effects of worksite exposures to some leading neurotoxic substances
Figures
Point to a thumbnail to see figure caption, click to see figure in article context.

8. Renal-Urinary System (2)

8. Renal-Urinary System
Chapter Editor: George P. Hemstreet
Table of Contents
Tables and Figures
Renal-Urinary Systems
George P. Hemstreet
Renal-Urinary Cancers
Timo Partanen, Harri Vainio, Paolo Boffetta and Elisabete Weiderpass
Tables
Click a link below to view table in article context.
- Drug-metabolism enzymes in kidney
- The most common causes of haematuria, by age & sex
- Criteria for biomarker selection
- Potential biomarkers linked to cell injury
- Acute renal insufficiency & occupation
- Segments of the nephron affected by selected toxicants
- Applications of urinary cytology
Figures
Point to a thumbnail to see figure caption, click to see figure in article context.

9. Reproductive System (9)

9. Reproductive System
Chapter Editor: Grace Kawas Lemasters
Table of Contents
Tables and Figures
Reproductive System: Introduction
Lowell E. Sever
Introduction to Male and Female Reproductive Function
Donald R. Mattison
Male Reproductive System and Toxicology
Steven Schrader and Grace Kawas Lemasters
Structure of the Female Reproductive System and Target Organ Vulnerability
Donald R. Mattison
Maternal Occupational Exposures and Adverse Pregnancy Outcomes
Grace Kawas Lemasters
Preterm Delivery and Work
Nicole Mamelle
Occupational and Environmental Exposures to the Newborn
Mary S. Wolff and Patrisha M. Woolard
Maternity Protection in Legislation
Marie-Claire Séguret
Pregnancy and US Work Recommendations
Leon J. Warshaw
Tables
Click a link below to view table in article context.
1. Exposures with multiple adverse endpoints
2. Epidemiological studies of paternal effects on pregnancy outcome
3. Potential female reproductive toxicants
4. Definition of foetal loss & infant death
5. Factors for small for gestational age and foetal loss
6. Identified sources of occupational fatigue
7. Relative risks & fatigue indices for preterm delivery
8. Prematurity risk by number of occupational fatigue indices
9. Relative risks and changes in working conditions
10. Newborn exposure sources and levels
Figures
Point to a thumbnail to see figure caption, click to see figure in article context.

10. Respiratory System (18)

10. Respiratory System
Chapters Editors: Alois David and Gregory R. Wagner
Table of Contents
Tables and Figures
Structure and Function
Morton Lippmann
Lung Function Examination
Ulf Ulfvarson and Monica Dahlqvist
Diseases Caused by Respiratory Irritants and Toxic Chemicals
David L.S. Ryon and William N. Rom
Occupational Asthma
George Friedman-Jimenez and Edward L. Petsonk
Diseases Caused by Organic Dusts
Ragnar Rylander and Richard S. F. Schilling
Beryllium Disease
Homayoun Kazemi
Pneumoconioses: Definition
Alois David
ILO International Classification of Radiographs of Pneumoconioses
Michel Lesage
Aetiopathogenesis of Pneumoconioses
Patrick Sébastien and Raymond Bégin
Silicosis
John E. Parker and Gregory R. Wagner
Coal Workers’ Lung Diseases
Michael D. Attfield, Edward L. Petsonk and Gregory R. Wagner
Asbestos-Related Diseases
Margaret R. Becklake
Hard Metal Disease
Gerolamo Chiappino
Respiratory System: The Variety of Pneumoconioses
Steven R. Short and Edward L. Petsonk
Chronic Obstructive Pulmonary Disease
Kazimierz Marek and Jan E. Zejda
Health Effects of Man-Made Fibres
James E. Lockey and Clara S. Ross
Respiratory Cancer
Paolo Boffetta and Elisabete Weiderpass
Occupationally Acquired Infections of the Lung
Anthony A. Marfin, Ann F. Hubbs, Karl J. Musgrave, and John E. Parker
Tables
Click a link below to view table in article context.
1. Respiratory tract regions & particle deposition models
2. Inhalable, thoracic & respirable dust criteria
3. Summary of respiratory irritants
4. Mechanisms of lung injury by inhaled substances
5. Compounds capable of lung toxicity
6. Medical case definition of occupational asthma
7. Steps in diagnostic evaluation of asthma in the workplace
8. Sensitizing agents that can cause occupational asthma
9. Examples of sources of hazards of exposure to organic dust
10. Agents in organic dusts with potential biological activity
11. Diseases induced by organic dusts & their ICD codes
12. Diagnostic criteria for byssinosis
13. Properties of beryllium & its compounds
14. Description of standard radiographs
15. ILO 1980 Classification: Radiographs of Pneumoconioses
16. Asbestos-related diseases & conditions
17. Main commercial sources, products & uses of asbestos
18. Prevalence of COPD
19. Risk factors implicated in COPD
20. Loss of ventilatory function
21. Diagnostic classification, chronic bronchitis & emphysema
22. Lung function testing in COPD
23. Synthetic fibres
24. Established human respiratory carcinogens (IARC)
25. Probable human respiratory carcinogens (IARC)
26. Occupationally acquired respiratory infectious diseases
Figures
Point to a thumbnail to see figure caption, click to see figure in article context.

11. Sensory Systems (8)

11. Sensory Systems
Chapter Editor: Heikki Savolainen
Table of Contents
Tables and Figures
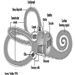
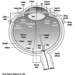
The Ear
Marcel-André Boillat
Chemically-Induced Hearing Disorders
Peter Jacobsen
Physically-Induced Hearing Disorders
Peter L. Pelmear
Equilibrium
Lucy Yardley
Vision and Work
Paule Rey and Jean-Jacques Meyer
Taste
April E. Mott and Norman Mann
Smell
April E. Mott
Cutaneous Receptors
Robert Dykes and Daniel McBain
Tables
Click a link below to view table in article context.
1. Typical calculation of functional loss from an audiogram
2. Visual requirements for different activities
3. Recommended illuminance values for the lighting design
4. Visual requirements for a driving licence in France
5. Agents/processes reported to alter the taste system
6. Agents/processes associated with olfactory abnormalities
Figures
Point to a thumbnail to see figure caption, click to see figure in article context.

12. Skin Diseases (7)

12. Skin Diseases
Chapter Editor: Louis-Philippe Durocher
Table of Contents
Tables and Figures
Overview: Occupational Skin Diseases
Donald J. Birmingham
Non-Melanocytic Skin Cancer
Elisabete Weiderpass, Timo Partanen, Paolo Boffetta
Malignant Melanoma
Timo Partanen, Paolo Boffetta, Elisabete Weiderpass
Occupational Contact Dermatitis
Denis Sasseville
Prevention of Occupational Dermatoses
Louis-Phillipe Durocher
Occupational Nail Dystrophy
C.D. Calnan
Stigmata
H. Mierzecki
Tables
Click a link below to view table in article context.
1. Occupations at risk
2. Types of contact dermatitis
3. Common irritants
4. Common skin allergens
5. Predisposing factors for occupational dermatitis
6. Examples of skin irritants & sensitizers with occupations
7. Occupational dermatoses in Quebec in 1989
8. Risk factors & their effects on the skin
9. Collective measures (group approach) to prevention
Figures
Point to a thumbnail to see figure caption, click to see figure in article context.

13. Systemic Conditions (3)

13. Systemic Conditions
Chapter Editor: Howard M. Kipen
Table of Contents
Figures
Systemic Conditions: An Introduction
Howard M. Kipen
Sick Building Syndrome
Michael J. Hodgson
Multiple Chemical Sensitivities
Mark R. Cullen
Figures
Point to a thumbnail to see figure caption, click to see figure in article context.
Physical Factors
Noise
Hearing loss due to workplace noise has been recognized as an occupational disease for many years. Cardiovascular diseases are at the centre of the discussion on possible chronic extra-aural effects of noise. Epidemiological studies have been done within the workplace noise field (with high-level noise indicators) as well as in the surrounding noise field (with low-level noise indicators). The best studies to date were done on the relationship between exposure to noise and high blood pressure. In numerous new survey studies, noise researchers have assessed the available research results and summarized the current state of knowledge (Kristensen 1994; Schwarze and Thompson 1993; van Dijk 1990).
Studies show that the noise risk factor for diseases of the cardiovascular system is less significant than behavioural risk factors like smoking, poor nutrition or physical inactivity (Aro and Hasan 1987; Jegaden et al. 1986; Kornhuber and Lisson 1981).
The results of epidemiological studies do not permit any final answer on the adverse cardiovascular health effects of chronic workplace or environmental noise exposure. The experimental knowledge on hormonal stress effects and changes in peripheral vasoconstriction, on the one hand, and the observation, on the other, that a high workplace noise level >85 dBA) promotes the development of hypertension, allow us to include noise as an non-specific stress stimulus in a multi-factored risk model for cardiovascular diseases, warranting high biological plausibility.
The opinion is advanced in modern stress research that although increases in blood pressure during work are connected to noise exposure, the blood pressure level per se depends on a complex set of personality and environmental factors (Theorell et al. 1987). Personality and environmental factors play an intimate role in determining the total stress load at the workplace.
For this reason it appears all the more urgent to study the effect of multiple burdens at the workplace and to clarify the cross effects, mostly unknown up to now, between combined influencing exogenous factors and diverse endogenous risk characteristics.
Experimental studies
It is today generally accepted that noise exposure is a psychophysical stressor. Numerous experimental studies on animals and human subjects permit extending the hypothesis on the pathomechanism of noise to the development of cardiovascular diseases. There is a relatively uniform picture with respect to acute peripheral reactions to noise stimuli. Noise stimuli clearly cause peripheral vasoconstriction, measurable as a decrease in finger pulse amplitude and skin temperature and an increase in systolic and diastolic blood pressure. Almost all studies confirm an increase in heart rate (Carter 1988; Fisher and Tucker 1991; Michalak, Ising and Rebentisch 1990; Millar and Steels 1990; Schwarze and Thompson 1993; Thompson 1993). The degree of these reactions is modified by such factors as the type of noise occurrence, age, sex, state of health, nervous state and personal characteristics (Harrison and Kelly 1989; Parrot et al. 1992; Petiot et al. 1988).
A wealth of research deals with the effects of noise on metabolism and hormone levels. Exposure to loud noise almost always results fairly quickly in changes such as in blood cortisone, cyclical adenosinmonophosphate (CAMP), cholesterol and certain lipoprotein fractions, glucose, protein fractions, hormones (e.g., ACTH, prolactin), adrenalin and noradrenalin. Increased catecholamine levels can be found in the urine. All of this clearly shows that noise stimuli below the noise-deafness level can lead to hyperactivity of the hypophyseal adrenal cortex system (Ising and Kruppa 1993; Rebentisch, Lange-Asschenfeld and Ising 1994).
Chronic exposure to loud noise has been shown to result in a reduction of magnesium content in serum, erythrocytes and in other tissues, such as the myocardium (Altura et al. 1992), but study results are contradictory (Altura 1993; Schwarze and Thompson 1993).
The effect of workplace noise on blood pressure is equivocal. A series of epidemiological studies, which were mostly designed as cross-sectional studies, indicate that employees with long-term exposure to loud noise show higher systolic and/or diastolic blood pressure values than those who work under less noisy conditions. Counterpoised, however, are studies that found very little or no statistical association between long-term noise exposure and in- creased blood pressure or hypertension (Schwarze and Thompson 1993; Thompson 1993; van Dijk 1990). Studies that enlist hearing loss as a surrogate for noise show varied results. In any case, hearing loss is not a suitable biological indicator for noise ex- posure (Kristensen 1989; van Dijk 1990). The indications are mounting that noise and the risk factors—increased blood pres- sure, increased serum cholesterol level (Pillsburg 1986), and smoking (Baron et al. 1987)—have a synergistic effect on the de- velopment of noise-induced hearing loss. Differentiating between hearing loss from noise and hearing loss from other factors is difficult. In the studies (Talbott et al. 1990; van Dijk, Veerbeck and de Vries 1987), no connection was found between noise exposure and high blood pressure, whereas hearing loss and high blood pressure have a positive correlation after correction for the usual risk factors, especially age and body weight. The relative risks for high blood pressure range between 1 and 3.1 in com- parisons of exposure to loud and less loud noise. Studies with qualitatively superior methodology report a lower relationship. Differences among the blood pressure group means are relatively narrow, with values between 0 and 10 mm Hg.
A large epidemiological study of women textile workers in China (Zhao, Liu and Zhang 1991) plays a key role in noise effect research. Zhao ascertained a dose-effect relationship between noise levels and blood pressure among women industrial workers who were subject to various noise exposures over many years. Using an additive logistical model the factors “indicated cooking salt use”, “family history of high blood pressure” and “noise level” (0.05) significantly correlated with the probability of high blood pressure. The authors judged that no confounding was present due to overweight. The noise level factor nevertheless constituted half the risk of hypertension of the first two named factors. An increase in the noise level from 70 to 100 dBA raised the risk for high blood pressure by a factor of 2.5. The quantification of the risk of hypertension by using higher noise exposure levels was possible in this study only because the offered hearing protection was not worn. This study looked at non-smoking women aged 35 ±8 years, so according to v. Eiff’s results (1993), the noise-related risk of hypertension among men could be significantly higher.
Hearing protection is prescribed in western industrialized countries for noise levels over 85-90 dBA. Many studies carried out in these countries demonstrated no clear risk at such noise levels, so it can be concluded from Gierke and Harris (1990) that limiting the noise level to the set limits prevents most extra-aural effects.
Heavy Physical Work
The effects of “lack of movement” as a risk factor for cardiovascular disease and of physical activity as promoting health were elucidated in such classic publications as those by Morris, Paffenbarger and their co-workers in the 1950s and 1960s, and in numerous epidemiological studies (Berlin and Colditz 1990; Powell et al. 1987). In previous studies, no direct cause-and-effect relationship could be shown between lack of movement and the rate of cardiovascular disease or mortality. Epidemiological studies, however, point to the positive, protective effects of physical activity on reducing various chronic diseases, including coronary heart disease, high blood pressure, non insulin dependent diabetes mellitus, osteoporosis and colon cancer, as well as anxiety and depression. The connection between physical inactivity and the risk of coronary heart disease has been observed in numerous countries and population groups. The relative risk for coronary heart disease among inactive people compared to active people varies between 1.5 and 3.0; with the studies using qualitatively higher methodology showing higher relationship. This increased risk is comparable to that found for hypercholesterolemia, hypertension and smoking (Berlin and Colditz 1990; Centers for Disease Control and Prevention 1993; Kristensen 1994; Powell et al. 1987).
Regular, leisure-time physical activity appears to reduce the risk of coronary heart disease through various physiological and metabolic mechanisms. Experimental studies have shown that with regular motion training, the known risk factors and other health-related factors are positively influenced. It results, for example, in an increase in the HDL-cholesterol level, and a decrease in the serum-triglyceride level and blood pressure (Bouchard, Shepard and Stephens 1994; Pate et al. 1995).
A series of epidemiological studies, spurred on by the studies of Morris et al. on coronary risk among London bus drivers and conductors (Morris, Heady and Raffle 1956; Morris et al. 1966), and the study of Paffenbarger et al. (1970) among American harbour workers, looked at the relationship between the difficulty level of physical work and the incidence of cardiovascular diseases. Based on earlier studies from the 1950s and 1960s the prevailing idea was that physical activity at work could have a certain protective effect on the heart. The highest relative risk for cardiovascular diseases was found in people with physically inactive jobs (e.g., sitting jobs) as compared to people who do heavy physical work. But newer studies have found no difference in the frequency of coronary disease between active and inactive occupational groups or have even found a higher prevalence and incidence of cardiovascular risk factors and cardiovascular diseases among heavy labourers (Ilmarinen 1989; Kannel et al. 1986; Kristensen 1994; Suurnäkki et al. 1987). Several reasons can be given for the contradiction between the health-promoting effect of free-time physical activities on cardiovascular morbidity and the lack of this effect with heavy physical labour:
- Primary and secondary selection processes (healthy worker effect) can lead to serious distortions in occupational medical epidemiological studies.
- The relationship found between physical work and the onset of cardiovascular diseases can be influenced by a number of confounding variables (like social status, education, behavioural risk factors).
- Assessing the physical load, often solely on the basis of job descriptions, must be seen as an inadequate method.
Social and technological development since the 1970s has meant that only a few jobs with “dynamic physical activity” remain. Physical activity in the modern workplace often means heavy lifting or carrying and a high proportion of static muscle work. So it is not surprising that physical activity in occupations of this type lacks an essential criterion for coronary-protective effect: a sufficient intensity, duration and frequency to optimize the physical load on big muscle groups. The physical work is, in general, intensive, but has less of a workout effect on the cardiovascular system. The combination of heavy, physically demanding work and high free-time physical activity could establish the most favourable situation with respect to the cardiovascular risk-factor profile and the onset of CHD (Saltin 1992).
The results of studies to date are also not consistent on the question of whether heavy physical work is related to the onset of arterial hypertension.
Physically demanding work is related to changes in blood pressure. In dynamic work that utilizes big muscle masses, blood supply and demand are in balance. In dynamic work that requires the smaller and middle muscle masses, the heart may put out more blood than is needed for the total physical work and the result can be considerably increased systolic and diastolic blood pressure (Frauendorf et al. 1986).
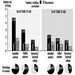
Even with combined physical-mental strain or physical strain under the effects of noise, a substantial increase in blood pressure and heart rate are seen in a certain percentage (approximately 30%) of people (Frauendorf, Kobryn and Gelbrich 1992; Frauendorf et al. 1995).
No studies are presently available on the chronic effects of this increased circulatory activity in local muscle work, with or without noise or mental strain.
In two recently published independent studies, by American and German researchers (Mittleman et al. 1993; Willich et al. 1993), the question was pursued as to whether heavy physical work can be a trigger for an acute myocardial infarction. In the studies, of 1,228 and 1,194 people with acute myocardial infarction respectively, the physical strain one hour before the infarction was compared with the situation 25 hours before. The following relative risks were calculated for the onset of a myocardial infarction within one hour of heavy physical strain in comparison with light activity or rest: 5.9 (CI 95%: 4.6-7.7) in the American and 2.1 (CI 95%: 1.6-3.1) in the German study. The risk was highest for people not in shape. An important limiting observation is, however, that the heavy physical strain occurred one hour before the infarction in only 4.4 and 7.1% of the infarction patients respectively.
These studies involve questions of the significance of physical strain or a stress-induced increased output of catecholamines on the coronary blood supply, on triggering coronary spasms, or an immediately harmful effect of catecholamines on the beta adrenergic receptors of the heart muscle membrane as a cause of the infarction manifestation or acute cardiac death. It can be assumed that such results will not ensue with a healthy coronary vessel system and intact myocardium (Fritze and Müller 1995).
The observations make clear that statements on possible causal relationships between heavy physical labour and effects on cardiovascular morbidity are not easy to substantiate. The problem with this type of investigation clearly lies in the difficulty in measuring and assessing “hard work” and in excluding preselections (healthy worker effect). Prospective cohort studies are needed on the chronic effects of selected forms of physical work and also on the effects of combined physical-mental or noise stress on selected functional areas of the cardiovascular system.
It is paradoxical that the result of reducing heavy dynamic muscle work—until now greeted as a significant improvement in the level of strain in the modern workplace—possibly results in a new, significant health problem in modern industrial society. From the occupational medicine perspective, one might conclude that static physical strain on the muscle-skeleton system with lack of movement, presents a much greater health risk than previously assumed, according to the results of studies to date.
Where monotonous improper strains cannot be avoided, counterbalancing with free-time sports activities of comparable duration should be encouraged (e.g., swimming, bicycling, walking and tennis).
Heat and Cold
Exposure to extreme heat or cold is thought to influence cardiovascular morbidity (Kristensen 1989; Kristensen 1994). The acute effects of high outside temperatures or cold on the circulatory system are well documented. An increase in mortality as a result of cardiovascular diseases, mostly heart attacks and strokes, was observed at low temperatures (under +10°C) in the winter in countries at northern latitudes (Curwen 1991; Douglas, Allan and Rawles 1991; Kristensen 1994; Kunst, Looman and Mackenbach 1993). Pan, Li and Tsai (1995) found an impressive U-shaped relationship between outside temperature and mortality rates for coronary heart disease and strokes in Taiwan, a subtropical country, with a similarly falling gradient between +10°C and +29°C and a sharp increase thereafter at over +32°C. The temperature at which the lowest cardiovascular mortality was observed is higher in Taiwan than in countries with colder climates. Kunst, Looman and Mackenbach found in the Netherlands a V-shaped relationship between total mortality and outside temperature, with the lowest mortality at 17°C. Most cold-related deaths occurred in people with cardiovascular diseases, and most heat-related deaths were associated with respiratory tract illnesses. Studies from the United States (Rogot and Padgett 1976) and other countries (Wyndham and Fellingham 1978) show a similar U-shaped relationship, with the lowest heart attack and stroke mortality at outside temperatures around 25 to 27°C.
It is not yet clear how these results should be interpreted. Some authors have concluded that a causal relationship possibly exists between temperature stress and the pathogenesis of cardiovascular diseases (Curwen and Devis 1988; Curwen 1991; Douglas, Allan and Rawles 1991; Khaw 1995; Kunst, Looman and Mackenbach 1993; Rogot and Padgett 1976; Wyndham and Fellingham 1978). This hypothesis was supported by Khaw in the following observations:
- Temperature proved to be the strongest, acute (day to day) predictor for cardiovascular mortality under the parameters which were handled differently, such as seasonal environmental changes and factors like air pollution, sunlight exposure, incidence of flu and nutrition. This speaks against the assumption that temperature acts only as a substitute variable for other detrimental environmental conditions.
- The consistency of the connection in various countries and population groups, over time and in different age groups, is furthermore convincing.
- Data from clinical and laboratory research suggests various biologically plausible pathomechanisms, including effects of changing temperature on haemostasis, blood viscosity, lipid levels, the sympathetic nervous system and vasoconstriction (Clark and Edholm 1985; Gordon, Hyde and Trost 1988; Keatinge et al. 1986; Lloyd 1991; Neild et al. 1994; Stout and Grawford 1991; Woodhouse, Khaw and Plummer 1993b; Woodhouse et al. 1994).
Exposure to cold increases blood pressure, blood viscosity and heart rate (Kunst, Looman and Mackenbach 1993; Tanaka, Konno and Hashimoto 1989; Kawahara et al. 1989). Studies by Stout and Grawford (1991) and Woodhouse and co-workers (1993; 1994) show that fibrinogens, blood clotting factor VIIc and lipids were higher among older people in the winter.
An increase in blood viscosity and serum cholesterol was found with exposure to high temperatures (Clark and Edholm 1985; Gordon, Hyde and Trost 1988; Keatinge et al. 1986). According to Woodhouse, Khaw and Plummer (1993a), there is a strong inverse correlation between blood pressure and temperature.
Still unclear is the decisive question of whether long-term exposure to cold or heat results in lasting increased risk of cardiovascular disease, or whether exposure to heat or cold increases the risk for an acute manifestation of cardiovascular diseases (e.g., a heart attack, a stroke) in connection with the actual exposure (the “triggering effect”). Kristensen (1989) concludes that the hypothesis of an acute risk increase for complications from cardiovascular disease in people with underlying organic disease is confirmed, whereas the hypothesis of a chronic effect of heat or cold can neither be confirmed nor rejected.
There is little, if any, epidemiological evidence to support the hypothesis that the risk of cardiovascular disease is higher in populations with an occupational, long-term exposure to high temperature (Dukes-Dobos 1981). Two recent cross-section studies focused on metalworkers in Brazil (Kloetzel et al. 1973) and a glass factory in Canada (Wojtczak-Jaroszowa and Jarosz 1986). Both studies found a significantly increased prevalence of hypertension among those subject to high temperatures, which increased with the duration of the hot work. Presumed influences of age or nutrition could be excluded. Lebedeva, Alimova and Efendiev (1991) studied mortality among workers in a metallurgical company and found high mortality risk among people exposed to heat over the legal limits. The figures were statistically significant for blood diseases, high blood pressure, ischemic heart disease and respiratory tract diseases. Karnaukh et al. (1990) report an increased incidence of ischemic heart disease, high blood pressure and haemorrhoids among workers in hot casting jobs. The design of this study is not known. Wild et al. (1995) assessed the mortality rates between 1977 and 1987 in a cohort study of French potash miners. The mortality from ischemic heart disease was higher for underground miners than for above-ground workers (relative risk = 1.6). Among people who were separated from the company for health reasons, the ischemic heart disease mortality was five times higher in the exposed group as compared to the above-ground workers. A cohort mortality study in the United States showed a 10% lower cardiovascular mortality for heat-exposed workers as compared to the non-exposed control group. In any case, among those workers who were in heat-exposed jobs less than six months, the cardiovascular mortality was relatively high (Redmond, Gustin and Kamon 1975; Redmond et al. 1979). Comparable results were cited by Moulin et al. (1993) in a cohort study of French steel workers. These results were attributed to a possible healthy worker effect among the heat-exposed workers.
There are no known epidemiological studies of workers exposed to cold (e.g., cooler, slaughterhouse or fishery workers). It should be mentioned that cold stress is not only a function of temperature. The effects described in the literature appear to be influenced by a combination of factors like muscle activity, dress, dampness, drafts and possibly poor living conditions. Workplaces with exposure to cold should pay special attention to appropriate dress and avoiding drafts (Kristensen 1994).
Vibration
Hand-arm vibration stress
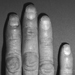
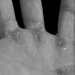
It is long known and well documented that vibrations transmitted to the hands by vibrating tools can cause peripheral vascular disorders in addition to damage to the muscle and skeletal system, and peripheral nerve-function disorders in the hand-arm area (Dupuis et al. 1993; Pelmear, Taylor and Wasserman 1992). The “white finger disease”, first described by Raynaud, appears with higher prevalency rates among exposed populations, and is recognized as an occupational disease in many countries.
Raynaud’s phenomenon is marked by an attack with vasospastic reduced fusion of all or some fingers, with the exception of the thumbs, accompanied by sensibility disorders in the affected fingers, feelings of cold, pallor and paraesthesia. After the exposure ends, circulation resumes, accompanied by a painful hyperaemia.
It is assumed that endogenous factors (e.g., in the sense of a primary Raynaud’s phenomenon) as well as exogenous exposures can be held responsible for the occurrence of a vibration-related vasospastic syndrome (VVS). The risk is clearly greater with vibrations from machines with higher frequencies (20 to over 800 Hz) than with machines that produce low-frequency vibrations. The amount of static strain (gripping and pressing strength) appears to be a contributing factor. The relative significance of cold, noise and other physical and psychological stressors, and heavy nicotine consumption is still unclear in the development of the Raynaud’s phenomenon.
The Raynaud’s phenomenon is pathogenetically based on a vasomotor disorder. Despite a large number of studies on functional, non-invasive (thermography, plethysmography, capillaroscopy, cold test) and invasive examinations (biopsy, arteriography), the pathophysiology of the vibration-related Raynaud’s phenomenon is not yet clear. Whether the vibration directly causes damage to the vascular musculature (a “local fault”), or whether it is a vasoconstriction as a result of sympathetic hyperactivity, or whether both these factors are necessary, is at present still unclear (Gemne 1994; Gemne 1992).
The work-related hypothenar hammer syndrome (HHS) should be distinguished in the differential diagnosis from vibration-caused Raynaud’s phenomenon. Pathogenetically this is a chronic-traumatic damage to the artery ulnaris (intima lesion with subsequent thrombosization) in the area of the superficial course above the unciform bone (os hamatum). HHS is caused by long-term mechanical effects in the form of external pressure or blows, or by sudden strain in the form of mechanical partial body vibrations (often combined with persistent pressure and the effects of impacts). For this reason, HHS can occur as a complication or in connection with a VVS (Kaji et al. 1993; Marshall and Bilderling 1984).
In addition to the early and, for exposure against hand-arm vibration, specific peripheral vascular effects, of particular scientific interest are the so-called non-specific chronic changes of autonomous regulations of the organ systems—for example, of the cardiovascular system, perhaps provoked by vibration (Gemne and Taylor 1983). The few experimental and epidemiological studies of possible chronic effects of hand-arm vibration give no clear results confirming the hypothesis of possible vibration-related endocrine and cardiovascular function disorders of the metabolic processes, cardiac functions or blood pressure (Färkkilä, Pyykkö and Heinonen 1990; Virokannas 1990) other than that the activity of the adrenergic system is increased from exposure to vibration (Bovenzi 1990; Olsen 1990). This applies to vibration alone or in combination with other strain factors like noise or cold.
Whole-body vibration stress
If whole-body mechanical vibrations have an effect on the cardio- vascular system, then a series of parameters such as heart rate, blood pressure, cardiac output, electrocardiogram, plethysmo- gram and certain metabolic parameters must show corresponding reactions. Conclusions on this are made difficult for the method- ological reason that these circulation quantifications do not react specifically to vibrations, but can also be influenced by other simultaneous factors. Increases in heart rate are apparent only under very heavy vibration loads; the influence on blood pressure values shows no systematic results and electrocardiographic (ECG) changes are not significantly differentiable.
Peripheral circulatory disorders resulting from vasoconstriction have been less researched and appear weaker and of shorter duration than those from hand-arm vibrations, which are marked by an effect on the grasping strength of the fingers (Dupuis and Zerlett 1986).
In most studies the acute effects of whole-body vibrations on the cardiovascular system of vehicle drivers were found to be relatively weak and temporary (Dupius and Christ 1966; Griffin 1990).
Wikström, Kjellberg and Landström (1994), in a comprehensive overview, cited eight epidemiological studies from 1976 to 1984 that examined the connection between whole-body vibrations and cardiovascular diseases and disorders. Only two of these studies found a higher prevalence of such illnesses in the group exposed to vibrations, but none where this was interpreted as the effect of whole-body vibrations.
The view is widely accepted that changes of physiological functions through whole-body vibrations have only a very limited effect on the cardiovascular system. Causes as well as mechanisms of the reaction of the cardiovascular system to whole-body vibrations are not yet sufficiently known. At present there is no basis to assume that whole-body vibrations per se contribute to the risk of diseases of the cardiovascular system. But attention should be paid to the fact that this factor very often is combined with exposure to noise, inactivity (sitting work) and shift work.
Ionizing Radiation, Electromagnetic Fields, Radioand Microwaves, Ultra- and Infrasound
Many case studies and a few epidemiological studies have drawn attention to the possibility that ionizing radiation, introduced to treat cancer or other diseases, may promote the development of arteriosclerosis and thereby increase the risk for coronary heart disease and also other cardiovascular diseases (Kristensen 1989; Kristensen 1994). Studies on the incidence of cardiovascular diseases in occupational groups exposed to ionizing radiation are not available.
Kristensen (1989) reports on three epidemiological studies from the early 1980s on the connection between cardiovascular diseases and exposure to electromagnetic fields. The results are contradic- tory. In the 1980s and 1990s the possible effects of electrical and magnetic fields on human health have attracted increasing atten- tion from people in occupational and environmental medicine. Partially contradictory epidemiological studies that looked for cor- relations between occupational and/or environmental exposure to weak, low-frequency electrical and magnetic fields, on the one hand, and the onset of health disorders on the other, aroused considerable attention. In the foreground of the numerous experi- mental and few epidemiological studies stand possible long-term effects such as carcinogenicity, teratogenicity, effects on the im- mune or hormone systems, on reproduction (with special atten- tion to miscarriages and defects), as well as to “hypersensitivity to electricity” and neuro-psychological behavioural reactions. Poss- ible cardiovascular risk is not being discussed at present (Gamber- ale 1990; Knave 1994).
Certain immediate effects of low-frequency magnetic fields on the organism that have been scientifically documented through in vitro and in vivo examinations of low to high field strengths should be mentioned in this connection (UNEP/WHO/IRPA 1984; UNEP/WHO/IRPA 1987). In the magnetic field, such as in the blood stream or during heart contraction, charged carriers lead to induction of electrical fields and currents. Thus the electrical voltage that is created in a strong static magnetic field over the aorta near the heart during coronary activity can amount to 30 mV at a flow thickness of 2 Tesla (T), and induction values over 0.1 T were detected in the ECG. But effects on the blood pressure, for example, were not found. Magnetic fields that change with time (intermittent magnetic fields) induce electrical eddy fields in biological objects that can for example arouse nerve and muscle cells in the body. No certain effect appears with electrical fields or induced currents under 1 mA/m2. Visual (induced with magnetophosphene) and nervous effects are reported at 10 to 100 mA/m2. Extrasystolic and heart chamber fibrillations appear at over 1 A/m2. According to currently available data, no direct health threat is to be expected for short-term whole-body exposure up to 2 T (UNEP/WHO/IRPA 1987). However, the danger threshold for indirect effects (e.g., from the magnetic field force action on ferromagnetic materials) lies lower than that for direct effects. Precautionary measures are thus required for persons with ferromagnetic implants (unipolar pacemakers, magnetizable aneurysm clips, haemoclips, artificial heart valve parts, other electrical implants, and also metal fragments). The danger threshold for ferromagnetic implants begins at 50 to 100 mT. The risk is that injuries or bleeding can result from migration or pivotal motions, and that functional capacities (e.g., of heart valves, pacemakers and so on) can be affected. In facilities in research and industry with strong magnetic fields, some authors advise medical surveillance examinations for people with cardiovascular diseases, including high blood pressure, in jobs where the magnetic field exceeds 2 T (Bernhardt 1986; Bernhardt 1988). Whole-body exposure of 5 T can lead to magnetoelectrodynamic and hydrodynamic effects on the circulatory system, and it should be assumed that short-term whole-body exposure of 5 T causes health hazards, especially for people with cardiovascular diseases, including high blood pressure (Bernhardt 1988; UNEP/WHO/ IRPA 1987).
Studies that examine the various effects of radio and microwaves have found no detrimental effects to health. The possibility of cardiovascular effects from ultrasound (frequency range between 16 kHz and 1 GHz) and infrasound (frequency range >>20 kHz) are discussed in the literature, but the empirical evidence is very slight (Kristensen 1994).
Depression
Depression is an enormously important topic in the area of workplace mental health, not only in terms of the impact depression can have on the workplace, but also the role the workplace can play as an aetiological agent of the disorder.
In a 1990 study, Greenberg et al. (1993a) estimated that the economic burden of depression in the United States that year was approximately US$ 43.7 billion. Of that total, 28% was attributable to direct costs of medical care, but 55% was derived from a combination of absenteeism and decreased productivity while at work. In another paper, the same authors (1993b) note:
“two distinguishing features of depression are that it is highly treatable and not widely recognized. The NIMH has noted that between 80% and 90% of individuals suffering from a major depressive disorder can be treated successfully, but that only one in three with the illness ever seeks treatment.… Unlike some other diseases, a very large share of the total costs of depression falls on employers. This suggests that employers as a group may have a particular incentive to invest in programs that could reduce the costs associated with this illness.”
Manifestations
Everyone feels sad or “depressed” from time to time, but a major depressive episode, according to the Diagnostic and Statistical Manual of Mental Disorders, 4th edition (DSM IV) (American Psychiatric Association 1994), requires that several criteria be met. A full description of these criteria is beyond the scope of this article, but portions of criterion A, which describes the symptoms, can give one a sense of what a true major depression looks like:
A. Five (or more) of the following symptoms have been present during the same 2-week period and represent a change from previous functioning; at least one of the symptoms is number 1 or 2.
- depressed mood most of the day, nearly every day
- markedly diminished interest or pleasure in all, or almost all, activities most of the day, nearly every day
- significant weight loss when not dieting or weight gain, or decrease or increase in appetite nearly every day
- insomnia or hypersomnia nearly every day
- psychomotor agitation or retardation nearly every day
- fatigue or loss of energy nearly every day
- feelings of worthlessness or excessive or inappropriate guilt nearly every day
- diminished ability to think or concentrate, or indecisiveness nearly every day
- recurrent thoughts of death, recurrent suicidal ideation, with or without a plan, or a suicide attempt.
Besides giving one an idea of the discomfort suffered by a person with depression, a review of these criteria also shows the many ways depression can impact negatively on the workplace. It is also important to note the wide variation of symptoms. One depressed person may present barely able to move to get out of bed, while others may be so anxious they can hardly sit still and describe themselves as crawling out of their skin or losing their mind. Sometimes multiple physical aches and pains without medical explanation may be a hint of depression.
Prevalence
The following passage from Mental Health in the Workplace (Kahn 1993) describes the pervasiveness (and increase) of depression in the workplace:
“Depression … is one of the most common mental health problems in the workplace. Recent research … suggests that in industrialized countries the incidence of depression has increased with each decade since 1910, and the age at which someone is likely to become depressed has dropped with every generation born after 1940. Depressive illnesses are common and serious, taking a tremendous toll on both workers and workplace. Two out of ten workers can expect a depression during their lifetime, and women are one and a half times more likely than men to become depressed. One out of ten workers will develop a clinical depression serious enough to require time off from work.”
Thus, in addition to the qualitative aspects of depression, the quantitative/epidemiological aspects of the disease make it a major concern in the workplace.
Related Illnesses
Major depressive disorder is only one of a number of closely related illnesses, all under the category of “mood disorders”. The most well known of these is bipolar (or “manic-depressive”) illness, in which the patient has alternating periods of depression and mania, which includes a feeling of euphoria, a decreased need for sleep, excessive energy and rapid speech, and can progress to irritability and paranoia.
There are several different versions of bipolar disorder, depending on the frequency and severity of the depressive and manic episodes, the presence or absence of psychotic features (delusions, hallucinations) and so on. Similarly, there are several different variations on the theme of depression, depending on severity, presence or absence of psychosis, and types of symptom most prominent. Again, it is beyond the scope of this article to delineate all of these, but the reader is again referred to DSM IV for a complete listing of all the different forms of mood disorder.
Differential Diagnosis
The differential diagnosis of major depression involves three major areas: other medical disorders, other psychiatric disorders and medication-induced symptoms.
Just as important as the fact that many patients with depression first present to their general practitioners with physical complaints is the fact that many patients who initially present to a mental health clinician with depressive complaints may have an undiagnosed medical illness causing the symptoms. Some of the most common illnesses causing depressive symptoms are endocrine (hormonal), such as hypothyroidism, adrenal problems or changes related to pregnancy or the menstrual cycle. Particularly in older patients, neurological diseases, such as dementia, strokes or Parkinson’s disease, become more prominent in the differential diagnosis. Other illnesses that can present with depressive symptoms are mononucleosis, AIDS, chronic fatigue syndrome and some cancers and joint diseases.
Psychiatrically, the disorders which share many common features with depression are the anxiety disorders (including generalized anxiety, panic disorder and post-traumatic stress disorder), schizophrenia and drug and alcohol abuse. The list of medications that can cause depressive symptoms is quite lengthy, and includes pain medications, some antibiotics, many anti-hypertensives and cardiac drugs, and steroids and hormonal agents.
For further detail on all three areas of the differential diagnosis of depression, the reader is referred to Kaplan and Sadock’s Synopsis of Psychiatry (1994), or the more detailed Comprehensive Textbook of Psychiatry (Kaplan and Sadock 1995).
Workplace Aetiologies
Much can be found elsewhere in this Encyclopaedia regarding workplace stress, but what is important in this article is the manner in which certain aspects of stress can lead to depression. There are many schools of thought regarding the aetiology of depression, including biological, genetic and psychosocial. It is in the psychosocial realm that many factors relating to the workplace can be found.
Issues of loss or threatened loss can lead to depression and, in today’s climate of downsizing, mergers and shifting job descriptions, are common problems in the work environment. Another result of frequently changing job duties and the constant introduction of new technologies is to leave workers feeling incompetent or inadequate. According to psychodynamic theory, as the gap between one’s current self image and “ideal self” widens, depression ensues.
An animal experimental model known as “learned helplessness” can also be used to explain the ideological link between stressful workplace environments and depression. In these experiments, animals were exposed to electric shocks from which they could not escape. As they learned that none of the actions they took had any effect on their eventual fate, they displayed increasingly passive and depressive behaviours. It is not difficult to extrapolate this model to today’s workplace, where so many feel a sharply decreasing amount of control over both their day-to-day activities and long-range plans.
Treatment
In light of the aetiological link of the workplace to depression described above, a useful way of looking at the treatment of depression in the workplace is the primary, secondary, tertiary model of prevention. Primary prevention, or trying to eliminate the root cause of the problem, entails making fundamental organizational changes to ameliorate some of the stressors described above. Secondary prevention, or trying to “immunize” the individual from contracting the illness, would include such interventions as stress management training and lifestyle changes. Tertiary prevention, or helping to return the individual to health, involves both psychotherapeutic and psychopharmacological treatment.
There is an increasing array of psychotherapeutic approaches available to the clinician today. The psychodynamic therapies look at the patient’s struggles and conflicts in a loosely structured format that allows explorations of whatever material may come up in a session, however tangential it may initially appear. Some modifications of this model, with boundaries set in terms of number of sessions or breadth of focus, have been made to create many of the newer forms of brief therapy. Interpersonal therapy focuses more exclusively on the patterns of the patient’s relationships with others. An increasingly popular form of therapy is cognitive therapy, which is driven by the precept, “What you think is how you feel”. Here, in a very structured format, the patient’s “automatic thoughts” in response to certain situations are examined, questioned and then modified to produce a less maladaptive emotional response.
As rapidly as the psychotherapies have developed, the psychopharmacological armamentarium has probably grown even faster. In the few decades before the 1990s, the most common medications used to treat depression were the tricyclics (imipramine, amitriptyline and nortriptyline are examples) and the monoamine oxidase inhibitors (Nardil, Marplan and Parnate). These medications act on neurotransmitter systems thought to be involved with depression, but also affect many other receptors, resulting in a number of side effects. In the early 1990s, several new medications (fluoxetine, sertraline, Paxil, Effexor, fluvoxamine and nefazodone) were introduced. These medications have enjoyed rapid growth because they are “cleaner” (bind more specifically to depression-related neurotransmitter sites) and can thus effectively treat depression while causing much fewer side effects.
Summary
Depression is extremely important in the world of workplace mental health, both because of depression’s impact on the workplace, and the workplace’s impact on depression. It is a highly prevalent disease, and very treatable; but unfortunately frequently goes undetected and untreated, with serious consequences for both the individual and the employer. Thus, increased detection and treatment of depression can help lessen individual suffering and organizational losses.
Chemical Hazardous Material
Despite numerous studies, the role of chemical factors in causing cardiovascular diseases is still disputed, but probably is small. The calculation of the aetiological role of chemical occupational factors for cardiovascular diseases for the Danish population resulted in a value under 1% (Kristensen 1994). For a few materials such as carbon disulphide and organic nitrogen compounds, the effect on the cardiovascular system is generally recognized (Kristensen 1994). Lead seems to affect blood pressure and cerebrovascular morbidity. Carbon monoxide (Weir and Fabiano 1982) undoubtedly has acute effects, especially in provoking angina pectoris in pre-existing ischaemia, but probably does not increase the risk of the underlying arteriosclerosis, as was long suspected. Other materials like cadmium, cobalt, arsenic, antimony, beryllium, organic phosphates and solvents are under discussion, but not sufficiently documented as yet. Kristensen (1989, 1994) gives a critical overview. A selection of relevant activities and industrial branches can be found in Table 1.
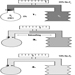
Table 1. Selection of activities and industrial branches that may be associated with cardiovascular hazards
|
Hazardous material |
Occupational branch affected/use |
|
Carbon disulphide (CS2 ) |
Rayon and synthetic fiber fabrication, rubber, |
|
Organic nitro-compounds |
Explosives and munitions manufacture, |
|
Carbon monoxide (CO) |
Employees in large industrial combustion |
|
Lead |
Smelting of lead ore and secondary raw |
|
Hydrocarbons, halogenated hydrocarbons |
Solvents (paints, lacquer) |
The exposure and effect data of important studies for carbon disulphide (CS2), carbon monoxide (CO) and nitroglycerine are given in the chemical section of the Encyclopaedia. This listing makes clear that problems of inclusion, combined exposures, varying consideration of compounding factors, changing target sizes and assessment strategies play a considerable role in the findings, so that uncertainties remain in the conclusions of these epidemiological studies.
In such situations clear pathogenetic conceptions and knowledge can support the suspected connections and thereby contribute to deriving and substantiating the consequences, including preventive measures. The effects of carbon disulphide are known on lipids and carbohydrate metabolism, on thyroid functioning (triggering hypothyroidism) and on coagulation metabolism (promoting thrombocyte aggregation, inhibiting plasminogen and plasmin activity). Changes in blood pressure such as hypertension are mostly traceable to vascular-based changes in the kidney, a direct causal link to high blood pressure due to carbon disulphide has not yet been excluded for certain, and a direct (reversible) toxic effect is suspected on the myocardium or an interference with the catecholamine metabolism. A successful 15-year intervention study (Nurminen and Hernberg 1985) documents the reversibility of the effect on the heart: a reduction in exposure was followed almost immediately by a decrease in cardiovascular mortality. In addition to the clearly direct cardiotoxic effects, arteriosclerotic changes in the brain, eye, kidney and coronary vasculature that can be considered the basis of encephalopathies, aneurysms in the retina area, nephropathies and chronic ischaemic heart disease have been proven among those who are exposed to CS2. Ethnic and nutritionally related components interfere in the pathomechanism; this was made clear in the comparative studies of Finnish and Japanese viscous rayon workers. In Japan, vascular changes in the area of the retina were found, whereas in Finland the cardiovascular effects dominated. Aneurysmatic changes in the retinal vasculature were observed at carbon disulphide concentrations under 3 ppm (Fajen, Albright and Leffingwell 1981). Reducing the exposure to 10 ppm clearly reduced cardiovascular mortality. This does not definitively clarify whether cardiotoxic effects are definitely excluded at doses under 10 ppm.
The acute toxic effects of organic nitrates involve widening of the vasa, accompanied by dropping blood pressure, increased heart rate, spotty erythema (flush), orthostatic dizziness and headaches. Since the half-life of the organic nitrate is short, the ailments soon subside. Normally, serious health considerations are not to be expected with acute intoxication. The so-called withdrawal syndrome appears when exposure is interrupted for employees with long-term exposure to organic nitrate, with a latency period of 36 to 72 hours. This includes ailments ranging from angina pectoris up to acute myocardial infarction and cases of sudden death. In the investigated deaths, often no coronary sclerotic changes were documented. The cause is therefore suspected to be “rebound vasospasm”. When the vasa-widening effect of the nitrate is removed, an autoregulative increase in resistance occurs in the vasa, including the coronary arteriae, which produces the above-mentioned results. In certain epidemiological studies, suspected associations between exposure duration and intensity of organic nitrate and ischaemic heart disease are considered uncertain, and pathogenetic plausibility for them is lacking.
Concerning lead, metallic lead in dust form, the salts of diva- lent lead and organic lead compounds are toxicologically impor- tant. Lead attacks the contractile mechanism of the vasa muscle cells and causes vascular spasms, which are considered causes for a series of symptoms of lead intoxication. Among these is tem- porary hypertension that appears with lead colic. Lasting high blood pressure from chronic lead intoxication can be explained by vasospasms as well as kidney changes. In epidemiological studies an association has been observed with longer exposure times between lead exposure and increased blood pressure, as well as an increased incidence of cerebrovascular diseases, whereas there was little evidence of increased cardiovascular diseases.
Epidemiological data and pathogenetic investigations to date have produced no clear results on the cardiovascular toxicity of other metals like cadmium, cobalt and arsenic. However, the hypothesis that halogenated hydrocarbon acts as a myocardial irritant is considered certain. The triggering mechanism of occasionally life-threatening arrhythmia from these materials presumably comes from myocardial sensitivity to epinephrine, which works as a natural carrier for the autonomic nervous system. Still being discussed is whether a direct cardiac effect exists such as reduced contractility, suppression of impulse formation centres, impulse transmission, or reflex impairment resulting from irrigation in the upper airway region. The sensitizing potential of hydrocarbons apparently depends on the degree of halogenation and on the type of the halogen contained, whereas chlorine-substituted hydrocarbons are supposed to have a stronger sensitizing effect than fluoride compounds. The maximum myocardial effect for hydrocarbons containing chlorine occurs at around four chlorine atoms per molecule. Short chain non-substituted hydrocarbons have a higher toxicity than ones with longer chains. Little is known about the arrhythmia-triggering dosage of the individual substances, as the reports on humans predominantly are case descriptions with exposure to high concentrations (accidental exposure and “sniffing”). According to Reinhardt et al. (1971), benzene, heptane, chloroform and trichlorethylene are especially sensitizing, whereas carbon tetrachloride and halothane have less arrhythmogenic effect.
The toxic effects of carbon monoxide result from tissue hypoxaemia, which results from the increased formation of CO-Hb (CO has 200-times greater affinity to haemoglobin than does oxygen) and the resulting reduced release of oxygen to the tissues. In addition to the nerves, the heart is one of the organs that react especially critically to such hypoxaemia. The resulting acute heart ailments have been repeatedly examined and described according to exposure time, breathing frequency, age and previous illnesses. Whereas among healthy subjects, cardiovascular effects first appear at CO-Hb concentrations of 35 to 40%, angina pectoris ailments could be experimentally produced in patients with ischaemic heart disease already at CO-Hb concentrations between 2 and 5% during physical exposure (Kleinman et al. 1989; Hinderliter et al. 1989). Deadly infarctions were observed among those with previous afflictions at 20% CO-Hb (Atkins and Baker 1985).
The effects of long-term exposure with low CO concentrations are still subject to controversy. Whereas experimental studies on animals possibly showed an atherogenic effect by way of hypoxia of the vasa walls or by direct CO effect on the vasa wall (increased vascular permeability), the flow characteristics of the blood (strengthened thrombocyte aggregation), or lipid metabolism, the corresponding proof for humans is lacking. The increased cardiovascular mortality among tunnel workers (SMR 1.35, 95% CI 1.09-1.68) can more likely be explained by acute exposure than from chronic CO effects (Stern et al. 1988). The role of CO in the cardiovascular effects of cigarette smoking is also not clear.
Work-Related Anxiety
Anxiety disorders as well as subclinical fear, worry and apprehension, and associated stress-related disorders such as insomnia, appear to be pervasive and increasingly prevalent in workplaces in the 1990s—so much so, in fact, that the Wall Street Journal has referred to the 1990s as the work-related “Age of Angst” (Zachary and Ortega 1993). Corporate downsizing, threats to existing benefits, lay-offs, rumours of impending lay-offs, global competition, skill obsolescence and “de-skilling”, re-structuring, re-engineering, acquisitions, mergers and similar sources of organizational turmoil have all been recent trends that have eroded workers’ sense of job security and have contributed to palpable, but difficult to precisely measure, “work-related anxiety” (Buono and Bowditch 1989). Although there appear to be some individual differences and situational moderator variables, Kuhnert and Vance (1992) reported that both blue-collar and white-collar manufacturing employees who reported more “job insecurity” indicated significantly more anxiety and obsessive-compulsive symptoms on a psychiatric checklist. For much of the 1980s and accelerating into the 1990s, the transitional organizational landscape of the US marketplace (or “permanent whitewater”, as it has been described) has undoubtedly contributed to this epidemic of work-related stress disorders, including, for example, anxiety disorders (Jeffreys 1995; Northwestern National Life 1991).
The problems of occupational stress and work-related psychological disorders appear to be global in nature, but there is a dearth of statistics outside of the United States documenting their nature and extent (Cooper and Payne 1992). The international data that are available, mostly from European countries, seem to confirm similar adverse mental health effects of job insecurity and high-strain employment on workers as those seen in US workers (Karasek and Theorell 1990). However, because of the very real stigma associated with mental disorders in most other countries and cultures, many, if not most, psychological symptoms, such as anxiety, related to work (outside of the United States) go unreported, undetected and untreated (Cooper and Payne 1992). In some cultures, these psychological disorders are somatized and manifested as “more acceptable” physical symptoms (Katon, Kleinman and Rosen 1982). A study of Japanese government workers has identified occupational stressors such as workload and role conflict as significant correlates of mental health in these Japanese workers (Mishima et al. 1995). Further studies of this kind are needed to document the impact of psychosocial job stressors on workers’ mental health in Asia, as well as in the developing and post-Communist countries.
Definition and Diagnosis of Anxiety Disorders
Anxiety disorders are evidently among the most prevalent of mental health problems afflicting, at any one time, perhaps 7 to 15% of the US adult population (Robins et al. 1981). Anxiety disorders are a family of mental health conditions which include agoraphobia (or, loosely, “houseboundness”), phobias (irrational fears), obsessive-compulsive disorder, panic attacks and generalized anxiety. According to the American Psychiatric Association’s Diagnostic and Statistical Manual of Mental Disorders, 4th edition (DSM IV), symptoms of a generalized anxiety disorder include feelings of “restlessness or feeling keyed up or on edge”, fatigue, difficulties with concentration, excess muscle tension and disturbed sleep (American Psychiatric Association 1994). An obsessive-compulsive disorder is defined as either persistent thoughts or repetitive behaviours that are excessive/unreasonable, cause marked distress, are time consuming and can interfere with a person’s functioning. Also, according to DSM IV, panic attacks, defined as brief periods of intense fear or discomfort, are not actually disorders per se but may occur in conjunction with other anxiety disorders. Technically, the diagnosis of an anxiety disorder can be made only by a trained mental health professional using accepted diagnostic criteria.
Occupational Risk Factors for Anxiety Disorders
There is a paucity of data pertaining to the incidence and prevalence of anxiety disorders in the workplace. Furthermore, since the aetiology of most anxiety disorders is multifactorial, we cannot rule out the contribution of individual genetic, developmental and non-work factors in the genesis of anxiety conditions. It seems likely that both work-related organizational and such individual risk factors interact, and that this interaction determines the onset, progression and course of anxiety disorders.
The term job-related anxiety implies that there are work conditions, tasks and demands, and/or related occupational stressors that are associated with the onset of acute and/or chronic states of anxiety or manifestations of anxiety. These factors may include an overwhelming workload, the pace of work, deadlines and a perceived lack of personal control. The demand-control model predicts that workers in occupations which offer little personal control and expose employees to high levels of psychological demand would be at risk of adverse health outcomes, including anxiety disorders (Karasek and Theorell 1990). A study of pill consumption (mostly tranquilizers) reported for Swedish male employees in high-strain occupations supported this prediction (Karasek 1979). Certainly, the evidence for an increased prevalence of depression in certain high-strain occupations in the United States is now compelling (Eaton et al. 1990). More recent epidemiological studies, in addition to theoretical and biochemical models of anxiety and depression, have linked these disorders not only by identifying their co-morbidity (40 to 60%), but also in terms of more fundamental commonalities (Ballenger 1993). Hence, the Encyclopaedia chapter on job factors associated with depression may provide pertinent clues to occupational and individual risk factors also associated with anxiety disorders. In addition to risk factors associated with high-strain work, a number of other workplace variables contributing to employee psychological distress, including an increased prevalence of anxiety disorders, have been identified and are briefly summarized below.
Individuals employed in dangerous lines of work, such as law enforcement and firefighting, characterized by the probability that a worker will be exposed to a hazardous agent or injurious activity, would also seem to be at risk of heightened and more prevalent states of psychological distress, including anxiety. However, there is some evidence that individual workers in such dangerous occupations who view their work as “exhilarating” (as opposed to dangerous) may cope better in terms of their emotional responses to work (McIntosh 1995). Nevertheless, an analysis of stress symptomatology in a large group of professional firefighters and paramedics identified a central feature of perceived apprehension or dread. This “anxiety stress pathway” included subjective reports of “being keyed up and jittery” and “being uneasy and apprehensive.” These and similar anxiety-related complaints were significantly more prevalent and frequent in the firefighter/paramedic group relative to a male community comparison sample (Beaton et al. 1995).
Another worker population evidently at risk of experiencing high, and at times debilitating, levels of anxiety are professional musicians. Professional musicians and their work are exposed to intense scrutiny by their supervisors; they must perform before the public and must cope with performance and pre-performance anxiety or “stage fright”; and they are expected (by others as well as by themselves) to produce “note-perfect performances” (Sternbach 1995). Other occupational groups, such as theatrical performers and even teachers who give public performances, may have acute and chronic anxiety symptoms related to their work, but very little data on the actual prevalence or significance of such occupational anxiety disorders have been collected.
Another class of work-related anxiety for which we have little data is “computer phobics”, people who have responded anxiously to the advent of computing technology (Stiles 1994). Even though each generation of computer software is arguably more “user-friendly”, many workers are uneasy, while other workers are literally panicked by challenges of “techno-stress”. Some fear personal and professional failure associated with their inability to acquire the necessary skills to cope with each successive generation of technology. Finally, there is evidence that employees subjected to electronic performance monitoring perceive their jobs as more stressing and report more psychological symptoms, including anxiety, than workers not so monitored (Smith et al. 1992).
Interaction of Individual and Occupational Risk Factors for Anxiety
It is likely that individual risk factors interact with and may potentiate the above-cited organizational risk factors at the onset, progression and course of anxiety disorders. For example, an individual employee with a “Type A personality” may be more prone to anxiety and other mental health problems in high-strain occupational settings (Shima et al. 1995). To offer a more specific example, an overly responsible paramedic with a “rescue personality” may be more on edge and hypervigilant while on duty then another paramedic with a more philosophical work attitude: “You can’t save them all” (Mitchell and Bray 1990). Individual worker personality variables may also serve to potentially buffer attendant occupational risk factors. For instance, Kobasa, Maddi and Kahn (1982) reported that corporate managers with “hardy personalities” seem better able to cope with work-related stressors in terms of health outcomes. Thus, individual worker variables need to be considered and evaluated within the context of the particular occupational demands to predict their likely interactive impact on a given employee’s mental health.
Prevention and Remediation ofWork-related Anxiety
Many of the US and global workplace trends cited at the beginning of this article seem likely to persist into the foreseeable future. These workplace trends will adversely impact workers’ psychological and physical health. Psychological job enhancement, in terms of interventions and workplace redesign, may deter and prevent some of these adverse effects. Consistent with the demand-control model, workers’ well-being can be improved by increasing their decision latitude by, for example, designing and implementing a more horizontal organizational structure (Karasek and Theorell 1990). Many of the recommendations made by NIOSH researchers, such as improving workers’ sense of job security and decreasing work role ambiguity, if implemented, would also likely reduce job strain and work-related psychological disorders considerably, including anxiety disorders (Sauter, Murphy and Hurrell 1992).
In addition to organizational policy changes, the individual employee in the modern workplace also has a personal responsibility to manage his or her own stress and anxiety. Some common and effective coping strategies employed by US workers include separating work and non-work activities, getting sufficient rest and exercise, and pacing oneself at work (unless, of course, the job is machine paced). Other helpful cognitive-behavioural alternatives in self-managing and preventing anxiety disorders include deep-breathing techniques, biofeedback-aided relaxation training, and meditation (Rosch and Pelletier 1987). In certain cases medications may be necessary to treat a severe anxiety disorder. These medications, including antidepressants and other anxiolytic agents, are generally available only by prescription.
Haematopoietic and Lymphatic System
The lymphohaemopoietic system consists of the blood, the bone marrow, the spleen, the thymus, lymphatic channels and lymph nodes. The blood and bone marrow together are referred to as the haematopoietic system. The bone marrow is the site of cell production, continually replacing the cellular elements of the blood (erythrocytes, neutrophils and platelets). Production is under tight control of a group of growth factors. Neutrophils and platelets are used as they perform their physiological functions, and erythrocytes eventually become senescent and outlive their usefulness. For successful function, the cellular elements of the blood must circulate in proper numbers and retain both their structural and physiological integrity. Erythrocytes contain haemoglobin, which permits uptake and delivery of oxygen to tissues to sustain cellular metabolism. Erythrocytes normally survive in the circulation for 120 days while sustaining this function. Neutrophils are found in blood on their way to tissues to participate in the inflammatory response to microbes or other agents. Circulating platelets play a key role in haemostasis.
The production requirement of the bone marrow is a prodigious one. Daily, the marrow replaces 3 billion erythrocytes per kilogram of body weight. Neutrophils have a circulating half-life of only 6 hours, and 1.6 billion neutrophils per kilogram of body weight must be produced each day. The entire platelet population must be replaced every 9.9 days. Because of the need to produce large numbers of functional cells, the marrow is remarkably sensitive to any infectious, chemical, metabolic or environmental insult that impairs DNA synthesis or disrupts the formation of the vital subcellular machinery of the red blood cells, white blood cells or platelets. Further, since the blood cells are marrow progeny, the peripheral blood serves as a sensitive and accurate mirror of bone marrow activity. Blood is readily available for assay via venipuncture, and examination of the blood can provide an early clue of environmentally induced illness.
The haematological system can be viewed as both serving as a conduit for substances entering the body and as an organ system that may be adversely affected by occupational exposures to potentially harmful agents. Blood samples may serve as a biological monitor of exposure and provide a way to assess the effects of occupational exposure on the lymphohaematopoietic system and other body organs.
Environmental agents can interfere with the haematopoietic system in several ways, including inhibition of haemoglobin synthesis, inhibition of cell production or function, leukaemogenesis and increased red blood cell destruction.
Abnormality of blood cell number or function caused directly by occupational hazards can be divided into those for which the haematological problem is the most important health effect, such as benzene-induced aplastic anaemia, and those for which the effects on the blood are direct but of less significance than the effects on other organ systems, such as lead-induced anaemia. Sometimes haematological disorders are a secondary effect of a workplace hazard. For example, secondary polycythaemia can be the result of an occupational lung disease. Table 1 lists those hazards which are reasonably well accepted as having a direct effect on the haematological system.
Table 1. Selected agents implicated in environmentally and occupationally acquired methaemoglobinaemia
- Nitrate-contaminated well water
- Nitrous gases (in welding and silos)
- Aniline dyes
- Food high in nitrates or nitrites
- Mothballs (containing naphthalene)
- Potassium chlorate
- Nitrobenzenes
- Phenylenediamine
- Toluenediamine
Examples of Workplace Hazards Primarily Affecting the Haematological System
Benzene
Benzene was identified as a workplace poison producing aplastic anaemia in the late 19th century (Goldstein 1988). There is good evidence that it is not benzene itself but rather one or more metabolites of benzene that is responsible for its haematological toxicity, although the exact metabolites and their subcellular targets have yet to be clearly identified (Snyder, Witz and Goldstein 1993).
Implicit in the recognition that benzene metabolism plays a role in its toxicity, as well as recent research on the metabolic processes involved in the metabolism of compounds such as benzene, is the likelihood that there will be differences in human sensitivity to benzene, based upon differences in metabolic rates conditioned by environmental or genetic factors. There is some evidence of a familial tendency towards benzene-induced aplastic anaemia, but this has not been clearly demonstrated. Cytochrome P-450(2E1) appears to play an important role in the formation of haematotoxic metabolites of benzene, and there is some suggestion from recent studies in China that workers with higher activities of this cytochrome are more at risk. Similarly, it has been suggested that Thalassaemia minor, and presumably other disorders in which there is increased bone marrow turnover, may predispose a person to benzene-induced aplastic anaemia (Yin et al. 1996). Although there are indications of some differences in susceptibility to benzene, the overall impression from the literature is that, in contrast to a variety of other agents such as chloramphenicol, for which there is a wide range in sensitivity, even including idiosyncratic reactions producing aplastic anaemia at relatively trivial levels of exposure, there is a virtual universal response to benzene exposure, leading to bone marrow toxicity and eventually aplastic anaemia in a dose-dependent fashion.
The effect of benzene on the bone marrow is thus analogous to the effect produced by chemotherapeutic alkylating agents used in the treatment of Hodgkin’s disease and other cancers (Tucker et al. 1988). With increasing dosage there is a progressive decline in all of the formed elements of the blood, which is sometimes manifested initially as anaemia, leucopenia or thrombocytopenia. It should be noted that it would be most unexpected to observe a person with thrombocytopenia that was not at least accompanied by a low normal level of the other formed blood elements. Further, such an isolated cytopenia would not be expected to be severe. In other words, an isolated white blood count of 2,000 per ml, where the normal range is 5,000 to 10,000, would suggest strongly that the cause of the leucopenia was other than benzene (Goldstein 1988).
The bone marrow has substantial reserve capacity. Following even a significant degree of hypoplasia of the bone marrow as part of a chemotherapeutic regimen, the blood count usually eventually returns to normal. However, individuals who have undergone such treatments cannot respond by producing as high a white blood cell count when exposed to a challenge to their bone marrow, such as endotoxin, as can individuals who have never previously been treated with such chemotherapeutic agents. It is reasonable to infer that there are dose levels of an agent such as benzene which can destroy bone marrow precursor cells and thus affect the reserve capability of the bone marrow without incurring sufficient damage to lead to a blood count that was lower than the laboratory range of normal. Because routine medical surveillance may not reveal abnormalities in a worker who may have indeed suffered from the exposure, the focus on worker protection must be preventive and employ basic principles of occupational hygiene. Although the extent of the development of bone marrow toxicity in relationship to benzene exposure at the workplace remains unclear, it does not appear that a single acute exposure to benzene is likely to cause aplastic anaemia. This observation might reflect the fact that bone marrow precursor cells are at risk only in certain phases of their cell cycle, perhaps when they are dividing, and not all the cells will be in that phase during a single acute exposure. The rapidity with which cytopenia develops depends in part on the circulating lifetime of the cell type. Complete cessation of bone marrow production would lead first to a leucopenia because white blood cells, particularly granulocytic blood cells, persist in circulation for less than a day. Next there would be a decrease in platelets, whose survival time is about ten days. Lastly there would be a decrease in red cells, which survive for a total of 120 days.
Benzene not only destroys the pluripotential stem cell, which is responsible for the production of red blood cells, platelets and granulocytic white blood cells, but it also has been found to cause a rapid loss in circulating lymphocytes in both laboratory animals and in humans. This suggests the potential for benzene to have an adverse effect on the immune system in exposed workers, an effect that has not been clearly demonstrated as yet (Rothman et al. 1996).
Benzene exposure has been associated with aplastic anaemia, which is frequently a fatal disorder. Death usually is caused by infection because the reduction in white blood cells, leucopenia, so compromises the body’s defence system, or by haemorrhage due to the reduction in platelets necessary for normal clotting. An individual exposed to benzene at a workplace who develops a severe aplastic anaemia must be considered to be a sentinel for similar effects in co-workers. Studies based on the discovery of a sentinel individual often have uncovered groups of workers who exhibit obvious evidence of benzene haematotoxicity. For the most part, those individuals who do not succumb relatively quickly to aplastic anaemia will usually recover following removal from the benzene exposure. In one follow-up study of a group of workers who previously had significant benzene-induced pancytopenia (decrease in all blood cell types) there were only minor residual haematological abnormalities ten years later (Hernberg et al. 1966). However, some workers in these groups, with initially relatively severe pancytopenia, progressed in their illnesses by first developing aplastic anaemia, then a myelodysplastic preleukaemic phase, and finally to the eventual development of acute myelogenous leukaemia (Laskin and Goldstein 1977). Such progression of disease is not unexpected since individuals with aplastic anaemia from any cause appear to have a higher-than-expected likelihood of developing acute myelogenous leukaemia (De Planque et al. 1988).
Other causes of aplastic anaemia
Other agents in the workplace have been associated with aplastic anaemia, the most notable being radiation. The effects of radiation on bone marrow stem cells have been employed in the therapy of leukaemia. Similarly, a variety of chemotherapeutic alkylating agents produce aplasia and pose a risk to workers responsible for producing or administering these compounds. Radiation, benzene and alkylating agents all appear to have a threshold level below which aplastic anaemia will not occur.
Protection of the production worker becomes more problematic when the agent has an idiosyncratic mode of action in which minuscule amounts may produce aplasia, such as chloramphenicol. Trinitrotoluene, which is absorbed readily through the skin, has been associated with aplastic anaemia in munition plants. A variety of other chemicals has been reported to be associated with aplastic anaemia, but it is often difficult to determine causality. An example is the pesticide lindane (gamma-benzene hexachloride). Case reports have appeared, generally following relatively high levels of exposure, in which lindane is associated with aplasia. This finding is far from being universal in humans, and there are no reports of lindane-induced bone marrow toxicity in laboratory animals treated with large doses of this agent. Bone marrow hypoplasia has also been associated with exposure to ethylene glycol ethers, various pesticides and arsenic (Flemming and Timmeny 1993).
Biological Hazards
“A biological hazardous material can be defined as a biological material capable of self-replication that can cause harmful effects in other organisms, especially humans” (American Industrial Hygiene Association 1986).
Bacteria, viruses, fungi and protozoa are among the biological hazardous materials that can harm the cardiovascular system through contact that is intentional (introduction of technology-related biological materials) or unintentional (non-technology-related contamination of work materials). Endotoxins and mycotoxins may play a role in addition to the infectious potential of the micro-organism. They can themselves be a cause or contributing factor in a developing disease.
The cardiovascular system can either react as a complication of an infection with a localized organ participation—vasculitis (inflammation of the blood vessels), endocarditis (inflammation of the endocardium, primarily from bacteria, but also from fungus and protozoa; acute form can follow septic occurrence; subacute form with generalization of an infection), myocarditis (heart muscle inflammation, caused by bacteria, viruses and protozoa), pericarditis (pericardium inflammation, usually accompanies myocarditis), or pancarditis (simultaneous appearance of endocarditis, myocarditis and pericarditis)—or be drawn as a whole into a systemic general illness (sepsis, septic or toxic shock).
The participation of the heart can appear either during or after the actual infection. As pathomechanisms the direct germ colon- ization or toxic or allergic processes should be considered. In addition to type and virulence of the pathogen, the efficiency of the immune system plays a role in how the heart reacts to an infection. Germ-infected wounds can induce a myo- or endo- carditis with, for example, streptococci and staphylococci. This can affect virtually all occupational groups after a workplace accident.
Ninety per cent of all traced endocarditis cases can be attributed to strepto- or staphylococci, but only a small portion of these to accident-related infections.
Table 1 gives an overview of possible occupation-related infectious diseases that affect the cardiovascular system.
Table 1. Overview of possible occupation-related infectious diseases that affect the cardiovascular system
|
Disease |
Effect on heart |
Occurrence/frequency of effects on heart in case of disease |
Occupational risk groups |
|
AIDS/HIV |
Myocarditis, Endocarditis, Pericarditis |
42% (Blanc et al. 1990); opportunistic infections but also by the HIV virus itself as lymphocytic myocarditis (Beschorner et al. 1990) |
Personnel in health and welfare services |
|
Aspergillosis |
Endocarditis |
Rare; among those with suppressed immune system |
Farmers |
|
Brucellosis |
Endocarditis, Myocarditis |
Rare (Groß, Jahn and Schölmerich 1970; Schulz and Stobbe 1981) |
Workers in meatpacking and animal husbandry, farmers, veterinarians |
|
Chagas’ disease |
Myocarditis |
Varying data: 20% in Argentina (Acha and Szyfres 1980); 69% in Chile (Arribada et al. 1990); 67% (Higuchi et al. 1990); chronic Chagas’ disease always with myocarditis (Gross, Jahn and Schölmerich 1970) |
Business travelers to Central and South America |
|
Coxsackiessvirus |
Myocarditis, Pericarditis |
5% to 15% with Coxsackie-B virus (Reindell and Roskamm 1977) |
Personnel in health and welfare services, sewer workers |
|
Cytomegaly |
Myocarditis, Pericarditis |
Extremely rare, especially among those with suppressed immune system |
Personnel who work with children (especially small children), in dialysis and transplant departments |
|
Diphtheria |
Myocarditis, Endocarditis |
With localized diphtheria 10 to 20%, more common with progressive D. (Gross, Jahn and Schölmerich 1970), especially with toxic development |
Personnel who work with children and in health services |
|
Echinococcosis |
Myocarditis |
Rare (Riecker 1988) |
Forestry workers |
|
Epstein-Barr virus infections |
Myocarditis, Pericarditis |
Rare; especially among those with defective immune system |
Health and welfare personnel |
|
Erysipeloid |
Endocarditis |
Varying data from rare (Gross, Jahn and Schölmerich 1970; Riecker 1988) to 30% (Azofra et al. 1991) |
Workers in meatpacking, fish processing, fishers, veterinarians |
|
Filariasia |
Myocarditis |
Rare (Riecker 1988) |
Business travelers in endemic areas |
|
Typhus among other rickettsiosis (exclud- ing Q fever) |
Myocarditis, Vasculitis of small vasa |
Data varies, through direct pathogen, toxic or resistance-reduction during fever resolution |
Business travelers in endemic areas |
|
Early summer meningo-encephalitis |
Myocarditis |
Rare (Sundermann 1987) |
Forestry workers, gardeners |
|
Yellow fever |
Toxic damage to vasa (Gross, Jahn and Schölmerich 1970), Myocarditis |
Rare; with serious cases |
Business travelers in endemic areas |
|
Haemorrhagic fever (Ebola, Marburg, Lassa, Dengue, etc.) |
Myocarditis and endocardial bleedings through general hemorrhage, cardiovascular failure |
No information available |
Health service employees in affected areas and in special laboratories, and workers in animal husbandry |
|
Influenza |
Myocarditis, Hemorrhages |
Data varying from rare to often (Schulz and Stobbe 1981) |
Health service employees |
|
Hepatitis |
Myocarditis (Gross, Willensand Zeldis 1981; Schulzand Stobbe 1981) |
Rare (Schulz and Stobbe 1981) |
Health and welfare employees, sewage and waste-water workers |
|
Legionellosis |
Pericarditis, Myocarditis, Endocarditis |
If occurs, probably rare (Gross, Willens and Zeldis 1981) |
Maintenance personnel in air conditioning, humidifiers, whirlpools, nursing staff |
|
Leishmaniasis |
Myocarditis (Reindell and Roskamm 1977) |
With visceral leishmaniasis |
Business travelers to endemic areas |
|
Leptospirosis (icteric form) |
Myocarditis |
Toxic or direct pathogen infection (Schulz and Stobbe 1981) |
Sewage and waste-water workers, slaughterhouse workers |
|
Listerellosis |
Endocarditis |
Very rare (cutaneous listeriosis predominant as occupational disease) |
Farmers, veterinarians, meat-processing workers |
|
Lyme disease |
In stage 2: Myocarditis Pancarditis In stage 3: Chronic carditis |
8% (Mrowietz 1991) or 13% (Shadick et al. 1994) |
Forestry workers |
|
Malaria |
Myocarditis |
Relatively frequent with malaria tropica (Sundermann 1987); direct infection of capillaries |
Business travelers in endemic areas |
|
Measles |
Myocarditis, Pericarditis |
Rare |
Personnel in health service and who work with children |
|
Foot-and-mouth disease |
Myocarditis |
Very rare |
Farmers, animal husbandry workers, (especially with cloven- hoofed animals) |
|
Mumps |
Myocarditis |
Rare—under 0.2-0.4% (Hofmann 1993) |
Personnel in health service and who work with children |
|
Mycoplasma- pneumonia infections |
Myocarditis, Pericarditis |
Rare |
Health service and welfare employees |
|
Ornithosis/Psittacosis |
Myocarditis, Endocarditis |
Rare (Kaufmann and Potter 1986; Schulz and Stobbe 1981) |
Ornamental bird and poultry raisers, pet shop workers, veterinarians |
|
Paratyphus |
Interstitial myocarditis |
Especially among older and very sick as toxic damage |
Development aid workers in tropics and subtropics |
|
Poliomyelitis |
Myocarditis |
Common in serious cases in the first and second weeks |
Health service employees |
|
Q fever |
Myocarditis, Endocarditis, Pericarditis |
Possible to age 20 after acute disease (Behymer and Riemann 1989); data from rare (Schulz and Stobbe 1981; Sundermann 1987) to 7.2% (Conolly et al. 1990); more frequent (68%) among chronic Q-fever with weak immune system or pre-existing heart disease (Brouqui et al. 1993) |
Animal husbandry workers, veterinarians, farmers, possibly also slaughterhouse and dairy workers |
|
Rubella |
Myocarditis, Pericarditis |
Rare |
Health service and child care employees |
|
Relapsing fever |
Myocarditis |
No information available |
Business travelers and health service workers in tropics and subtropics |
|
Scarlet fever and other streptococcal infections |
Myocarditis, Endocarditis |
In 1 to 2.5% rheumatic fever as complication (Dökert 1981), then 30 to 80% carditis (Sundermann 1987); 43 to 91% (al-Eissa 1991) |
Personnel in health service and who work with children |
|
Sleeping sickness |
Myocarditis |
Rare |
Business travelers to Africa between 20° Southern and Northern parallels |
|
Toxoplasmosis |
Myocarditis |
Rare, especially among those with weak immune systems |
People with occupational contact with animals |
|
Tuberculosis |
Myocarditis, Pericarditis |
Myocarditis especially in conjunction with miliary tuberculosis, pericarditis with high tuberculosis prevalence to 25%, otherwise 7% (Sundermann 1987) |
Health service employees |
|
Typhus abdominalis |
Myocarditis |
Toxic; 8% (Bavdekar et al. 1991) |
Development aid workers, personnel in microbiological laboratories (especially stool labs) |
|
Chicken pox, Herpes zoster |
Myocarditis |
Rare |
Employees in health service and who work with children |
Post-Traumatic Stress Disorder and its Relation to Occupational Health and Injury Prevention
Beyond the broad concept of stress and its relationship to general health issues, there has been little attention to the role of psychiatric diagnosis in the prevention and treatment of the mental health consequences of work-related injuries. Most of the work on job stress has been concerned with the effects of exposure to stressful conditions over time, rather than to problems associated with a specific event such as a traumatic or life-threatening injury or the witnessing of an industrial accident or act of violence. At the same time, Post-traumatic Stress Disorder (PTSD), a condition which has received considerable credibility and interest since the mid-1980s, is being more widely applied in contexts outside of cases involving war trauma and victims of crime. With respect to the workplace, PTSD has begun to appear as the medical diagnosis in cases of occupational injury and as the emotional outcome of exposure to traumatic situations occurring in the workplace. It is often the subject of controversy and some confusion with respect to its relationship to work conditions and the responsibility of the employer when claims of psychological injury are made. The occupational health practitioner is called upon increasingly to advise on company policy in the handling of these exposures and injury claims, and to render medical opinions with respect to the diagnosis, treatment and ultimate job status of these employees. Familiarity with PTSD and its related conditions is therefore increasingly important for the occupational health practitioner.
The following topics will be reviewed in this article:
- differential diagnosis of PTSD with other conditions such as primary depression and anxiety disorders
- relationship of PTSD to stress-related somatic complaints
- prevention of post-traumatic stress reactions in survivors and witnesses of psychologically traumatic events occurring in the workplace
- prevention and treatment of complications of work injury related to post-traumatic stress.
Post-traumatic Stress Disorder affects people who have been exposed to traumatizing events or conditions. It is characterized by symptoms of numbing, psychological and social withdrawal, difficulties controlling emotion, especially anger, and intrusive recollection and reliving of experiences of the traumatic event. By definition, a traumatizing event is one that is outside the normal range of everyday life events and is experienced as overwhelming by the individual. A traumatic event usually involves a threat to one’s own life or to someone close, or the witnessing of an actual death or serious injury, especially when this occurs suddenly or violently.
The psychiatric antecedents of our current concept of PTSD go back to the descriptions of “battle fatigue” and “shell shock” during and after the World Wars. However, the causes, symptoms, course and effective treatment of this often debilitating condition were still poorly understood when tens of thousands of Vietnam-era combat veterans began to appear in the US Veterans Administration Hospitals, offices of family doctors, jails and homeless shelters in the 1970s. Due in large part to the organized effort of veterans’ groups, in collaboration with the American Psychiatric Association, PTSD was first identified and described in 1980 in the 3rd edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM III) (American Psychiatric Association 1980). The condition is now known to affect a wide range of trauma victims, including survivors of civilian disasters, victims of crime, torture and terrorism, and survivors of childhood and domestic abuse. Although changes in the classification of the disorder are reflected in the current diagnostic manual (DSM IV), the diagnostic criteria and symptoms remain essentially unchanged (American Psychiatric Association 1994).
Diagnostic Criteria for Post-TraumaticStress Disorder
A. The person has been exposed to a traumatic event in which both of the following were present:
- The person experienced, witnessed, or was confronted with an event or events that involved actual or threatened death or serious injury, or a threat to the physical integrity of self or others.
- The person’s response involved intense fear, helplessness or horror.
B. The traumatic event is persistently re-experienced in one (or more) of the following ways:
- Recurrent and intrusive distressing recollections of the event, including images, thoughts or perceptions.
- Recurrent distressing dreams of the event.
- Acting or feeling as if the traumatic event were recurring.
- Intense psychological distress at exposure to internal or external cues that symbolize or resemble an aspect of the traumatic event.
- Physiological reactivity on exposure to internal or external cues that symbolize or resemble an aspect of the traumatic event.
C. Persistent avoidance of stimuli associated with the trauma and numbing of general responsiveness (not present before the trauma), as indicated by three (or more) of the following:
- Efforts to avoid thoughts, feelings or conversations associated with the trauma.
- Efforts to avoid activities, places or people that arouse recollections of the trauma.
- Inability to recall an important aspect of the trauma.
- Markedly diminished interest or participation in significant activities.
- Feeling of detachment or estrangement from others.
- Restricted range of affect (e.g., unable to have loving feelings).
- Sense of a foreshortened future (e.g., does not expect to have a career, marriage, children or a normal life span).
D. Persistent symptoms of increased arousal (not present before the trauma), as indicated by two (or more) of the following:
- Difficulty falling or staying asleep.
- Irritability or outbursts of anger.
- Difficulty concentrating.
- Hypervigilance.
- Exaggerated startle response.
E. Duration of the disturbance (symptoms in criteria B, C and D) is more than 1 month.
F. The disturbance causes clinically significant distress or impairment in social, occupational or other important areas of functioning.
Specify if:
Acute: if duration of symptoms is less than 3 months
Chronic: if duration of symptoms is 3 months or more.
Specify if:
With Delayed Onset: if onset of symptoms is at least 6 months after the stressor.
Psychological stress has achieved increasing recognition as an outcome of work-related hazards. The link between work hazards and post-traumatic stress was first established in the 1970s with the discovery of high incident rates of PTSD in workers in law enforcement, emergency medical, rescue and firefighting. Specific interventions have been developed to prevent PTSD in workers exposed to job-related traumatic stressors such as mutilating injury, death and use of deadly force. These interventions emphasize providing exposed workers with education about normal traumatic stress reactions, and the opportunity to actively surface their feelings and reactions with their peers. These techniques have become well established in these occupations in the United States, Australia and many European nations. Job-related traumatic stress, however, is not limited to workers in these high-risk industries. Many of the principles of preventive intervention developed for these occupations can be applied to programmes to reduce or prevent traumatic stress reactions in the general workforce.
Issues in Diagnosis and Treatment
Diagnosis
The key to the differential diagnosis of PTSD and traumatic-stress-related conditions is the presence of a traumatic stressor. Although the stressor event must conform to criterion A—that is, be an event or situation that is outside of the normal range of experience—individuals respond in various ways to similar events. An event that precipitates a clinical stress reaction in one person may not affect another significantly. Therefore, the absence of symptoms in other similarly exposed workers should not cause the practitioner to discount the possibility of a true post-trauma reaction in a particular worker. Individual vulnerability to PTSD has as much to do with the emotional and cognitive impact of an experience on the victim as it does to the intensity of the stressor itself. A prime vulnerability factor is a history of psychological trauma due to a previous traumatic exposure or significant personal loss of some kind. When a symptom picture suggestive of PTSD is presented, it is important to establish whether an event that may satisfy the criterion for a trauma has occurred. This is particularly important because the victim himself may not make the connection between his symptoms and the traumatic event. This failure to connect the symptom with the cause follows the common “numbing” reaction, which may cause forgetting or dissociation of the event, and because it is not unusual for symptom appearance to be delayed for weeks or months. Chronic and often severe depression, anxiety and somatic conditions are often the result of a failure to diagnose and treat. Thus, early diagnosis is particularly important because of the often hidden nature of the condition, even to the sufferer him- or herself, and because of the implications for treatment.
Treatment
Although the depression and anxiety symptoms of PTSD may respond to usual therapies such as pharmacology, effective treatment is different from those usually recommended for these conditions. PTSD may be the most preventable of all psychiatric conditions and, in the occupational health sphere, perhaps the most preventable of all work-related injuries. Because its occurrence is linked so directly to a specific stressor event, treatment can focus on prevention. If proper preventive education and counselling are provided soon after the traumatic exposure, subsequent stress reactions can be minimized or prevented altogether. Whether the intervention is preventive or therapeutic depends largely on timing, but the methodology is essentially similar. The first step in successful treatment or preventive intervention is allowing the victim to establish the connection between the stressor and his or her symptoms. This identification and “normalization” of what are typically frightening and confusing reactions is very important for reduction or prevention of symptoms. Once the normalization of the stress response has been accomplished, treatment addresses the controlled processing of the emotional and cognitive impact of the experience.
PTSD or conditions related to traumatic stress result from the sealing off of unacceptable or unacceptably intense emotional and cognitive reactions to traumatic stressors. It is generally considered that the stress syndrome can be prevented by providing the opportunity for controlled processing of the reactions to the trauma before the sealing off of the trauma occurs. Thus, prevention through timely and skilled intervention is the keystone for the treatment of PTSD. These treatment principles may depart from the traditional psychiatric approach to many conditions. Therefore, it is important that employees at risk of post-traumatic stress reactions be treated by mental health professionals with specialized training and experience in treating trauma-related conditions. The length of treatment is variable. It will depend on the timing of the intervention, the severity of the stressor, symptom severity and the possibility that a traumatic exposure may precipitate an emotional crisis linked to earlier or related experiences. A further issue in treatment concerns the importance of group treatment modalities. Victims of trauma can achieve enormous benefit from the support of others who have shared the same or similar traumatic stress experience. This is of particular importance in the workplace context, when groups of co-workers or entire work organizations are affected by a tragic accident, act of violence or traumatic loss.
Prevention of Post-Traumatic Stress Reactionsafter Incidents of Workplace Trauma
A range of events or situations occurring in the workplace may put workers at risk of post-traumatic stress reactions. These include violence or threat of violence, including suicide, inter-employee violence and crime, such as armed robbery; fatal or severe injury; and sudden death or medical crisis, such as heart attack. Unless properly managed, these situations can cause a range of negative outcomes, including post-traumatic stress reactions that may reach clinical levels, and other stress-related effects that will affect health and work performance, including avoidance of the workplace, concentration difficulties, mood disturbances, social withdrawal, substance abuse and family problems. These problems can affect not only line employees but management staff as well. Managers are at particular risk because of conflicts between their operational responsibilities, their feelings of personal responsibility for the employees in their charge and their own sense of shock and grief. In the absence of clear company policies and prompt assistance from health personnel to deal with the aftermath of the trauma, managers at all levels may suffer from feelings of helplessness that compound their own traumatic stress reactions.
Traumatic events in the workplace require a definite response from upper management in close collaboration with health, safety, security, communications and other functions. A crisis response plan fulfils three primary goals:
- prevention of post-traumatic stress reactions by reaching affected individuals and groups before they have a chance to seal over
- communication of crisis-related information in order to contain fears and control rumours
- fostering of confidence that management is in control of the crisis and demonstrating concern for employees’ welfare.
The methodology for the implementation of such a plan has been fully described elsewhere (Braverman 1992a,b; 1993b). It emphasizes adequate communication between management and employees, assembling of groups of affected employees and prompt preventive counselling of those at highest risk for post-traumatic stress because of their levels of exposure or individual vulnerability factors.
Managers and company health personnel must function as a team to be sensitive for signs of continued or delayed trauma-related stress in the weeks and months after the traumatic event. These can be difficult to identify for manager and health professional alike, because post-traumatic stress reactions are often delayed, and they can masquerade as other problems. For a supervisor or for the nurse or counsellor who becomes involved, any signs of emotional stress, such as irritability, withdrawal or a drop in productivity, may signal a reaction to a traumatic stressor. Any change in behaviour, including increased absenteeism, or even a marked increase in work hours (“workaholism”) can be a signal. Indications of drug or alcohol abuse or change in moods should be explored as possibly linked to post-traumatic stress. A crisis response plan should include training for managers and health professionals to be alert for these signs so that intervention can be rendered at the earliest possible point.
Stress-related Complications of Occupational Injury
It has been our experience reviewing workers’ compensation claims up to five years post-injury that post-traumatic stress syndromes are a common outcome of occupational injury involving life-threatening or disfiguring injury, or assault and other exposures to crime. The condition typically remains undiagnosed for years, its origins unsuspected by medical professionals, claims administrators and human resource managers, and even the employee him- or herself. When unrecognized, it can slow or even prevent recovery from physical injury.
Disabilities and injuries linked to psychological stress are among the most costly and difficult to manage of all work-related injuries. In the “stress claim”, an employee maintains he or she has been emotionally damaged by an event or conditions at work. Costly and hard to fight, stress claims usually result in litigation and in the separation of the employee. There exists, however, a vastly more frequent but seldom recognized source of stress-related claims. In these cases, serious injury or exposure to life-threatening situations results in undiagnosed and untreated psychological stress conditions that significantly affect the outcome of work-related injuries.
On the basis of our work with traumatic worksite injuries and violent episodes over a wide range of worksites, we estimate that at least half of disputed workers’ compensation claims involve unrecognized and untreated post-traumatic stress conditions or other psychosocial components. In the push to resolve medical problems and determine the employee’s employment status, and because of many systems’ fear and mistrust of mental health intervention, emotional stress and psychosocial issues take a back seat. When no one deals with it, stress can take the form of a number of medical conditions, unrecognized by the employer, the risk manager, the health care provider and the employee him- or herself. Trauma-related stress also typically leads to avoidance of the workplace, which increases the risk of conflicts and disputes regarding return to work and claims of disability.
Many employers and insurance carriers believe that contact with a mental health professional leads directly to an expensive and unmanageable claim. Unfortunately, this is often the case. Statistics bear out that claims for mental stress are more expensive than claims for other kinds of injuries. Furthermore, they are increasing faster than any other kind of injury claim. In the typical “physical-mental” claim scenario, the psychiatrist or psychologist appears only at the point—typically months or even years after the event—when there is a need for expert assessment in a dispute. By this time, the psychological damage has been done. The trauma-related stress reaction may have prevented the employee from returning to the workplace, even though he or she appeared visibly healed. Over time, the untreated stress reaction to the original injury has resulted in a chronic anxiety or depression, a somatic illness or a substance abuse disorder. Indeed, it is rare that mental health intervention is rendered at the point when it can prevent the trauma-related stress reaction and thus help the employee fully recover from the trauma of a serious injury or assault.
With a small measure of planning and proper timing, the costs and suffering associated with injury-related stress are among the most preventable of all injuries. The following are the components of an effective post-injury plan (Braverman 1993a):
Early intervention
Companies should require a brief mental health intervention whenever a severe accident, assault or other traumatic event impacts on an employee. This evaluation should be seen as preventive, rather than as tied to the standard claims procedure. It should be provided even if there is no lost time, injury or need for medical treatment. The intervention should emphasize education and prevention, rather than a strictly clinical approach that may cause the employee to feel stigmatized. The employer, perhaps in conjunction with the insurance provider, should take responsibility for the relatively small cost of providing this service. Care should be taken that only professionals with specialized expertise or training in post-traumatic stress conditions be involved.
Return to work
Any counselling or assessment activity should be coordinated with a return-to-work plan. Employees who have undergone a trauma often feel afraid or tentative about returning to the worksite. Combining brief education and counselling with visits to the workplace during the recovery period has been used to great advantage in accomplishing this transition and speeding return to work. Health professionals can work with the supervisor or manager in developing gradual re-entry into job functioning. Even when there is no remaining physical limitation, emotional factors may necessitate accommodations, such as allowing a bank teller who was robbed to work in another area of the bank for part of the day as she gradually becomes comfortable returning to work at the customer window.
Follow-up
Post-traumatic reactions are often delayed. Follow-up at 1- and 6-month intervals with employees who have returned to work is important. Supervisors are also provided with fact sheets on how to spot possible delayed or long-term problems associated with post-traumatic stress.
Summary: The Link between Post-Traumatic Stress Studies and Occupational Health
Perhaps more than any other health science, occupational medicine is concerned with the relationship between human stress and disease. Indeed, much of the research in human stress in this century has taken place within the occupational health field. As the health sciences in general became more involved in prevention, the workplace has become increasingly important as an arena for research into the contribution of the physical and psychosocial environment to disease and other health outcomes, and into methods for the prevention of stress-related conditions. At the same time, since 1980 a revolution in the study of post-traumatic stress has brought important progress to the understanding of the human stress response. The occupational health practitioner is at the intersection of these increasingly important fields of study.
As the landscape of work undergoes revolutionary transformation, and as we learn more about productivity, coping and the stressful impact of continued change, the line between chronic stress and acute or traumatic stress has begun to blur. The clinical theory of traumatic stress has much to tell us about how to prevent and treat work-related psychological stress. As in all health sciences, knowledge of the causes of a syndrome can help in prevention. In the area of traumatic stress, the workplace has shown itself to be an excellent place to promote health and healing. By being well acquainted with the symptoms and causes of post-traumatic stress reactions, occupational health practitioners can increase their effectiveness as agents of prevention.
Leukaemia, Malignant Lymphomas and Multiple Myeloma
Leukaemias
Leukaemias constitute 3% of all cancers worldwide (Linet 1985). They are a group of malignancies of blood precursor cells, classified according to cell type of origin, degree of cellular differentiation, and clinical and epidemiological behaviour. The four common types are acute lymphocytic leukaemia (ALL), chronic lymphocytic leukaemia (CLL), acute myelocytic leukaemia (AML) and chronic myelocytic leukaemia (CML). ALL develops rapidly, is the most common form of leukaemia in childhood and originates in the white blood corpuscles in the lymph nodes. CLL arises in bone marrow lymphocytes, develops very slowly and is more common in aged persons. AML is the common form of acute leukaemia in adults. Rare types of acute leukaemia include monocytic, basophilic, eosinophilic, plasma-, erythro- and hairy-cell leukaemias. These rarer forms of acute leukaemia are sometimes lumped together under the heading acute non-lymphocytic leukaemia (ANLL), due in part to the belief that they arise from a common stem cell. Most cases of CML are characterized by a specific chromosomal abnormality, the Philadelphia chromosome. The eventual outcome of CML often is leukaemic transformation to AML. Transformation to AML also can occur in polycythaemia vera and essential thrombocythaemia, neoplastic disorders with elevated red cell or platelet levels, as well as myelofibrosis and myeloid dysplasia. This has led to characterizing these disorders as related myeloproliferative diseases.
The clinical picture varies according to the type of leukaemia. Most patients suffer from fatigue and malaise. Haematological count anomalies and atypical cells are suggestive of leukaemia and indicate a bone marrow examination. Anaemia, thrombocytopenia, neutropenia, elevated leucocyte count and elevated number of blast cells are typical signs of acute leukaemia.
Incidence: The annual overall age-adjusted incidence of leukaemias varies between 2 and 12 per 100,000 in men and between 1 and 11 per 100,000 in women in different populations. High figures are encountered in North American, western European and Israeli populations, while low ones are reported for Asian and African populations. The incidence varies according to age and to type of leukaemia. There is a marked increase in the incidence of leukaemia with age, and there is also a childhood peak which occurs around two to four years of age. Different leukaemia subgroups display different age patterns. CLL is about twice as frequent in men as in women. Incidence and mortality figures of adult leukaemias have tended to stay relatively stable over the past few decades.
Risk factors: Familial factors in the development of leukaemia have been suggested, but the evidence for this is inconclusive. Certain immunological conditions, some of which are hereditary, appear to predispose to leukaemia. Down’s syndrome is predictive of acute leukaemia. Two oncogenic retroviruses (human T-cell leukaemia virus-I, human T-lymphotropic virus-II) have been identified as being related to the development of leukaemias. These viruses are thought to be early-stage carcinogens and as such are insufficient causes of leukaemia (Keating, Estey and Kantarjian 1993).
Ionizing radiation and benzene exposure are established environmental and occupational causes of leukaemias. The incidence of CLL, however, has not been associated with exposure to radiation. Radiation and benzene-induced leukaemias are recognized as occupational diseases in a number of countries.
Much less consistently, leukaemia excesses have been reported for the following groups of workers: drivers; electricians; telephone linepersons and electronic engineers; farmers; flour millers; gardeners; mechanics, welders and metal workers; textile workers; paper-mill workers; and workers in the petroleum industry and distribution of petroleum products. Some particular agents in the occupational environment have been consistently associated with increased risk of leukaemia. These agents include butadiene, electromagnetic fields, engine exhaust, ethylene oxide, insecticides and herbicides, machining fluids, organic solvents, petroleum products (including gasoline), styrene and unidentified viruses. Paternal and maternal exposures to these agents prior to conception have been suggested to increase the leukaemia risk in the offspring, but the evidence at this time is insufficient to establish such exposure as causative.
Treatment and prevention: Up to 75% of male cases of leukaemia may be preventable (International Agency for Research on Cancer 1990). Avoidance of exposure to radiation and benzene will reduce the risk of leukaemias, but the potential reduction worldwide has not been estimated. Treatments of leukaemias include chemotherapy (single agents or combinations), bone marrow transplant and interferons. Bone marrow transplant in both ALL and AML is associated with a disease-free survival between 25 and 60%. The prognosis is poor for patients who do not achieve remission or who relapse. Of those who relapse, about 30% achieve a second remission. The major cause of failure to achieve remission is death from infection and haemorrhage. The survival of untreated acute leukaemia is 10% within 1 year of diagnosis. The median survival of patients with CLL before the initiation of treatment is 6 years. The length of survival depends on the stage of the disease when the diagnosis is initially made.
Leukaemias may occur following medical treatment with radiation and certain chemotherapeutic agents of another malignancy, such as Hodgkin’s disease, lymphomas, myelomas, and ovarian and breast carcinomas. Most of these secondary cases of leukaemia are acute non-lymphocytic leukaemias or myelodysplastic syndrome, which is a preleukaemic condition. Chromosomal abnormalities appear to be more readily observed in both treatment-related leukaemias and in leukaemias associated with radiation and benzene exposure. These acute leukaemias also share a tendency to resist therapy. Activation of the ras oncogene has been reported to occur more frequently in patients with AML who worked in professions deemed to be at high risk of exposure to leukaemogens (Taylor et al. 1992).
Malignant Lymphomas and Multiple Myeloma
Malignant lymphomas constitute a heterogeneous group of neoplasms primarily affecting lymphoid tissues and organs. Malignant lymphomas are divided into two major cellular types: Hodgkin’s disease (HD) (International Classification of Disease, ICD-9 201) and non-Hodgkin lymphomas (NHL) (ICD-9 200, 202). Multiple myeloma (MM) (ICD-9 203) represents a malignancy of plasma cells within the bone marrow and accounts usually for less than 1% of all malignancies (International Agency for Research on Cancer 1993). In 1985, malignant lymphomas and multiple myelomas ranked seventh among all cancers worldwide. They represented 4.2% of all estimated new cancer cases and amounted to 316,000 new cases (Parkin, Pisani and Ferlay 1993).
Mortality and incidence of malignant lymphomas do not reveal a consistent pattern across socio-economic categories worldwide. Children’s HD has a tendency to be more common in less developed nations, while relatively high rates have been observed in young adults in countries in more developed regions. In some countries, NHL seems to be in excess among people in higher socio-economic groups, while in other countries no such clear gradient has been observed.
Occupational exposures may increase the risk of malignant lymphomas, but the epidemiological evidence is still inconclusive. Asbestos, benzene, ionizing radiation, chlorinated hydrocarbon solvents, wood dust and chemicals in leather and rubber-tire manufacturing are examples of agents that have been associated with the risk of unspecified malignant lymphomas. NHL is more common among farmers. Further suspect occupational agents for HD, NHL and MM are mentioned below.
Hodgkin’s disease
Hodgkin’s disease is a malignant lymphoma characterized by the presence of multinucleated giant (Reed-Sternberg) cells. Lymph nodes in the mediastinum and neck are involved in about 90% of the cases, but the disease may occur in other sites as well. Histological subtypes of HD differ in their clinical and epidemiological behaviour. The Rye classification system includes four subtypes of HD: lymphocytic predominance, nodular sclerosis, mixed cellularity and lymphocytic depletion. The diagnosis of HD is made by biopsy and treatment is radiation therapy alone or in combination with chemotherapy.
The prognosis of HD patients depends on the stage of the disease at diagnosis. About 85 to 100% of patients without massive mediastinal involvement survive for about 8 years from the start of the treatment without further relapse. When there is massive mediastinal involvement, about 50% of the cases suffer a relapse. Radiation therapy and chemotherapy may involve various side effects, such as secondary acute myelocytic leukaemia discussed earlier.
The incidence of HD has not undergone major changes over time but for a few exceptions, such as the populations of the Nordic countries, in which the rates have declined (International Agency for Research on Cancer 1993).
Available data show that in the 1980s the populations of Costa Rica, Denmark and Finland had median annual incidence rates of HD of 2.5 per 100,000 in men and 1.5 per 100,000 in women (standardized to world population); these figures yielded a sex ratio of 1.7. The highest rates in males were recorded for populations in Italy, the United States, Switzerland and Ireland, while the highest female rates were in the United States and Cuba. Low incidence rates have been reported for Japan and China (International Agency for Research on Cancer 1992).
Viral infection has been suspected as involved in the aetiology of HD. Infectious mononucleosis, which is induced by the Epstein-Barr virus, a herpes virus, has been shown to be associated with increased risk of HD. Hodgkin’s disease may also cluster in families, and other time-space constellations of cases have been observed, but the evidence that there are common aetiological factors behind such clusters is weak.
The extent to which occupational factors can lead to increased risk for HD has not been established. There are three predominant suspect agents—organic solvents, phenoxy herbicides and wood dust—but the epidemiological evidence is limited and controversial.
Non-Hodgkin lymphoma
About 98% of the NHLs are lymphocytic lymphomas. At least four different classifications of lymphocytic lymphomas have been commonly used (Longo et al. 1993). In addition, an endemic malignancy, Burkitt’s lymphoma, is endemic in certain areas of tropical Africa and New Guinea.
Thirty to fifty per cent of NHLs are curable with chemotherapy and/or radiotherapy. Bone marrow transplants may be necessary.
Incidence: High annual incidences of NHL (over 12 per 100,000, standardized to world standard population) have been reported during the 1980s for the White population in the United States, particularly San Francisco and New York City, as well as in some Swiss cantons, in Canada, in Trieste (Italy) and Porto Alegre (Brazil, in men). The incidence of NHL is usually higher in men than in women, with the typical excess in men being 50 to 100% greater than in women. In Cuba, and in the White population of Bermuda, however, the incidence is slightly higher in women (International Agency for Research on Cancer 1992).
NHL incidence and mortality rates have been rising in a number of countries worldwide (International Agency for Research on Cancer 1993). By 1988, the average annual incidence in US White men increased by 152%. Some of the increase is due to changes in diagnostic practices of physicians and part due to an increase in immunosuppressive conditions which are induced by the human immunodeficiency virus (HIV, associated with AIDS), other viruses and immunosuppressive chemotherapy. These factors do not explain the entire increase, and a considerable proportion of residual increase may be explained by dietary habits, environmental exposures such as hair dyes, and possibly familial tendencies, as well as some rare factors (Hartge and Devesa 1992).
Occupational determinants have been suspected to play a role in the development of NHL. It is currently estimated that 10% of NHLs are thought to be related to occupational exposures in the United States (Hartge and Devesa 1992), but this percentage varies by time period and location. The occupational causes are not well established. Excess risk of NHL has been associated with electric power plant jobs, farming, grain handling, metal working, petroleum refining and woodworking, and has been found among chemists. Occupational exposures that have been associated with an increased NHL risk include ethylene oxide, chlorophenols, fertilizers, herbicides, insecticides, hair dyes, organic solvents and ionizing radiation. A number of positive findings for phenoxyacetic acid herbicide exposure have been reported (Morrison et al. 1992). Some of the herbicides involved were contaminated with 2,3,7,8-tetrachlorodibenzo-para-dioxin (TCDD). The epidemiological evidence for occupational aetiologies of NHL is still limited, however.
Multiple myeloma
Multiple myeloma (MM) involves predominantly bone (especially the skull), bone marrow and kidney. It represents malignant proliferation of B-lymphocyte-derived cells that synthesize and secrete immunoglobulins. The diagnosis is made using radiology, a test for the MM-specific Bence-Jones proteinuria, determination of abnormal plasma cells in the bone marrow, and immunoelectrophoresis. MM is treated with bone marrow transplantation, radiation therapy, conventional chemotherapy or polychemotherapy, and immunological therapy. Treated MM patients survive 28 to 43 months on the average (Ludwig and Kuhrer 1994).
The incidence of MM increases sharply with increasing age. High age-standardized annual incidence rates (5 to 10 per 100,000 in men and 4 to 6 per 100,000 in women) have been encountered in the United States Black populations, in Martinique and among the Maoris in New Zealand. Many Chinese, Indian, Japanese and Filipino populations have low rates (less than 10 per 100,000 person-years in men and less than 0.3 per 100,000 person-years in women) (International Agency for Research on Cancer 1992). The rate of multiple myeloma has been on the increase in Europe, Asia, Oceania and in both the Black and White United States populations since the 1960s, but the increase has tended to level off in a number of European populations (International Agency for Research on Cancer 1993).
Throughout the world there is an almost consistent excess among males in the incidence of MM. This excess is typically of the order of 30 to 80%.
Familial and other case clusterings of MM have been reported, but the evidence is inconclusive as to the causes of such clusterings. The excess incidence among the United States Black population as contrasted with the White population points towards the possibility of differential host susceptibility among population groups, which may be genetic. Chronic immunological disorders have on occasion been associated with the risk of MM. The data on social class distribution of MM are limited and unreliable for conclusions on any gradients.
Occupational factors: Epidemiological evidence of an elevated risk of MM in gasoline-exposed workers and refinery workers suggests a benzene aetiology (Infante 1993). An excess of multiple myeloma has repeatedly been observed in farmers and farm workers. Pesticides represent a suspect group of agents. The evidence for carcinogenicity is, however, insufficient for phenoxyacetic acid herbicides (Morrison et al. 1992). Dioxins are sometimes impurities in some phenoxyacetic acid herbicides. There is a reported significant excess of MM in women residing in a zone contaminated with 2,3,7,8-tetrachlorodibenzo-para-dioxin after an accident in a plant near Seveso, Italy (Bertazzi et al. 1993). The Seveso results were based on two cases which occurred during ten years of follow-up, and further observation is needed to confirm the association. Another possible explanation for the increased risk in farmers and farm workers is exposure to some viruses (Priester and Mason 1974).
Further suspect occupations and occupational agents that have been associated with increased risk of MM include painters, truck drivers, asbestos, engine exhaust, hair-colouring products, radiation, styrene, vinyl chloride and wood dust. The evidence for these occupations and agents remains inconclusive.
Stress and Burnout and their Implication in the Work Environment
“An emerging global economy mandates serious scientific attention to discoveries that foster enhanced human productivity in an ever-changing and technologically sophisticated work world” (Human Capital Initiative 1992). Economic, social, psychological, demographic, political and ecological changes around the world are forcing us to reassess the concept of work, stress and burnout on the workforce.
Productive work “calls for a primary focus on reality external to one self. Work therefore emphasizes the rational aspects of people and problem solving” (Lowman 1993). The affective and mood side of work is becoming an ever-increasing concern as the work environment becomes more complex.
A conflict that may arise between the individual and the world of work is that a transition is called for, for the beginning worker, from the self-centredness of adolescence to the disciplined subordination of personal needs to the demands of the workplace. Many workers need to learn and adapt to the reality that personal feelings and values are often of little importance or relevance to the workplace.
In order to continue a discussion of work-related stress, one needs to define the term, which has been used widely and with varying meanings in the behavioural science literature. Stress involves an interaction between a person and the work environment. Something happens in the work arena which presents the individual with a demand, constraint, request or opportunity for behaviour and consequent response. “There is a potential for stress when an environmental situation is perceived as presenting a demand which threatens to exceed the person’s capabilities and resources for meeting it, under conditions where he/she expects a substantial differential in the rewards and costs from meeting the demand versus not meeting it” (McGrath 1976).
It is appropriate to state that the degree to which the demand exceeds the perceived expectation and the degree of differential rewards expected from meeting or not meeting that demand reflect the amount of stress that the person experiences. McGrath further suggests that stress may present itself in the following ways: “Cognitive-appraisal wherein subjectively experienced stress is contingent upon the person’s perception of the situation. In this category the emotional, physiological and behavioural responses are significantly influenced by the person’s interpretation of the ‘objective’ or external stress situation.”
Another component of stress is the individual’s past experience with a similar situation and his or her empirical response. Along with this is the reinforcement factor, whether positive or negative, successes or failures which can operate to reduce or enhance, respectively, levels of subjectively experienced stress.
Burnout is a form of stress. It is a process defined as a feeling of progressive deterioration and exhaustion and an eventual depletion of energy. It is also often accompanied by a loss of motivation, a feeling that suggests “enough, no more”. It is an overload that tends during the course of time to affect attitudes, mood and general behaviour (Freudenberger 1975; Freudenberger and Richelson 1981). The process is subtle; it develops slowly and sometimes occurs in stages. It is often not perceived by the person most affected, since he or she is the last individual to believe that the process is taking place.
The symptoms of burnout manifest themselves on a physical level as ill-defined psychosomatic complaints, sleep disturbances, excessive fatigue, gastrointestinal symptoms, backaches, headaches, various skin conditions or vague cardiac pains of an unexplained origin (Freudenberger and North 1986).
Mental and behavioural changes are more subtle. “Burnout is often manifest by a quickness to be irritated, sexual problems (e.g. impotence or frigidity), fault finding, anger and low frustration threshold” (Freudenberger 1984a).
Further affective and mood signs may be progressive detachment, loss of self-confidence and lowered self-esteem, depression, mood swings, an inability to concentrate or pay attention, an increased cynicism and pessimism, as well as a general sense of futility. Over a period of time the contented person becomes angry, the responsive person becomes silent and withdrawn and the optimist becomes a pessimist.
The affect feelings that appear to be most common are anxiety and depression. The anxiety most typically associated with work is performance anxiety. The forms of work conditions that are relevant in promoting this form of anxiety are role ambiguity and role overload (Srivastava 1989).
Wilke (1977) has indicated that “one area that presents particular opportunity for conflict for the personality-disordered individual concerns the hierarchical nature of work organizations. The source of such difficulties can rest with the individual, the organization, or some interactive combination.”
Depressive features are frequently found as part of the presenting symptoms of work-related difficulties. Estimates from epidemiological data suggest that depression affects 8 to 12% of men and 20 to 25% of women. The life expectancy experience of serious depressive reactions virtually assures that workplace issues for many people will be affected at some time by depression (Charney and Weissman 1988).
The seriousness of these observations was validated by a study conducted by Northwestern National Life Insurance Company—“Employee Burnout: America’s Newest Epidemic” (1991). It was conducted among 600 workers nationwide and identified the extent, causes, costs and solutions related to workplace stress. The most striking research findings were that one in three Americans seriously thought about quitting work in 1990 because of job stress, and a similar portion expected to experience job burnout in the future. Nearly half of the 600 respondents experienced stress levels as “extremely or very high.” Workplace changes such as cutting employee benefits, change of ownership, required frequent overtime or reduced workforce tend to speed up job stress.
MacLean (1986) further elaborates on job stressors as uncomfortable or unsafe working conditions, quantitative and qualitative overload, lack of control over the work process and work rate, as well as monotony and boredom.
Additionally, employers are reporting an ever-increasing number of employees with alcohol and drug abuse problems (Freudenberger 1984b). Divorce or other marital problems are frequently reported as employee stressors, as are long-term or acute stressors such as caring for an elderly or disabled relative.
Assessment and classification to diminish the possibility of burnout may be approached from the points of view related to vocational interests, vocational choices or preferences and characteristics of people with different preferences (Holland 1973). One might utilize computer-based vocational guidance systems, or occupational simulation kits (Krumboltz 1971).
Biochemical factors influence personality, and the effects of their balance or imbalance on mood and behaviour are found in the personality changes attendant on menstruation. In the last 25 years a great deal of work has been done on the adrenal catecholamines, epinephrine and norepinephrine and other biogenic amines. These compounds have been related to the experiencing of fear, anger and depression (Barchas et al. 1971).
The most commonly used psychological assessment devices are:
- Eysenck Personality Inventory and Mardsley Personality Inventory
- Gordon Personal Profile
- IPAT Anxiety Scale Questionnaire
- Study of Values
- Holland Vocational Preference Inventory
- Minnesota Vocational Interest Test
- Rorschach Inkblot Test
- Thematic Apperception Test
A discussion of burnout would not be complete without a brief overview of the changing family-work system. Shellenberger, Hoffman and Gerson (1994) indicated that “Families are struggling to survive in an increasingly complex and bewildering world. With more choices than they can consider, people are struggling to find the right balance between work, play, love and family responsibility.”
Concomitantly, women’s work roles are expanding, and over 90% of women in the US cite work as a source of identity and self-worth. In addition to the shifting roles of men and women, the preservation of two incomes sometimes requires changes in living arrangements, including moving for a job, long-distance commuting or establishing separate residences. All of these factors can put a great strain on a relationship and on work.
Solutions to offer to diminish burnout and stress on an individual level are:
- Learn to balance your life.
- Share your thoughts and communicate your concerns.
- Limit alcohol intake.
- Re-evaluate personal attitudes.
- Learn to set priorities.
- Develop interests outside of work.
- Do volunteer work.
- Re-evaluate your need for perfectionism.
- Learn to delegate and ask for assistance.
- Take time off.
- Exercise, and eat nutritional meals.
- Learn to take yourself less seriously.
On a larger scale, it is imperative that government and corporations accommodate to family needs. To reduce or diminish stress in the family-work system will require a significant reconfiguration of the entire structure of work and family life. “A more equitable arrangement in gender relationships and the possible sequencing of work and non-work over the life span with parental leaves of absence and sabbaticals from work becoming common occurrences” (Shellenberger, Hoffman and Gerson 1994).
As indicated by Entin (1994), increased differentiation of self, whether in a family or corporation, has important ramifications in reducing stress, anxiety and burnout.
Individuals need to be more in control of their own lives and take responsibility for their actions; and both individuals and corporations need to re-examine their value systems. Dramatic shifts need to take place. If we do not heed the statistics, then most assuredly burnout and stress will continue to remain the significant problem it has become for all society.
Agents or Work Conditions Affecting the Blood
Circulating Red Blood Cells
Interference in haemoglobin oxygen deliverythrough alteration of haeme
The major function of the red cell is to deliver oxygen to the tissue and to remove carbon dioxide. The binding of oxygen in the lung and its release as needed at the tissue level depends upon a carefully balanced series of physicochemical reactions. The result is a complex dissociation curve which serves in a healthy individual to maximally saturate the red cell with oxygen under standard atmospheric conditions, and to release this oxygen to the tissues based upon oxygen level, pH and other indicators of metabolic activity. Delivery of oxygen also depends upon the flow rate of oxygenated red cells, a function of viscosity and of vascular integrity. Within the range of the normal haematocrit (the volume of packed red cells), the balance is such that any decrease in blood count is offset by the decrease in viscosity, allowing improved flow. A decrease in oxygen delivery to the extent that someone is symptomatic is usually not observed until the haematocrit is down to 30% or less; conversely, an increase in haematocrit above the normal range, as seen in polycythaemia, may decrease oxygen delivery due to the effects of increased viscosity on blood flow. An exception is iron deficiency, in which symptoms of weakness and lassitude appear, primarily due to the lack of iron rather than to any associated anaemia (Beutler, Larsh and Gurney 1960).
Carbon monoxide is a ubiquitous gas which can have severe, possibly fatal, effects on the ability of haemoglobin to transport oxygen. Carbon monoxide is discussed in detail in the chemicals section of this Encyclopaedia.
Methaemoglobin-producing compounds. Methaemoglobin is another form of haemoglobin that is incapable of delivering oxygen to the tissues. In haemoglobin, the iron atom at the centre of the haeme portion of the molecule must be in its chemically reduced ferrous state in order to participate in the transport of oxygen. A certain amount of the iron in haemoglobin is continuously oxidized to its ferric state. Thus, approximately 0.5% of total haemoglobin in the blood is methaemoglobin, which is the chemically oxidized form of haemoglobin that cannot transport oxygen. An NADH-dependent enzyme, methaemoglobin reductase, reduces ferric iron back to ferrous haemoglobin.
A number of chemicals in the workplace can induce levels of methaemoglobin that are clinically significant, as for example in industries using aniline dyes. Other chemicals that have been found frequently to cause methaemoglobinaemia in the workplace are nitrobenzenes, other organic and inorganic nitrates and nitrites, hydrazines and a variety of quinones (Kiese 1974). Some of these chemicals are listed in Table 1 and are discussed in more detail in the chemicals section of this Encyclopaedia. Cyanosis, confusion and other signs of hypoxia are the usual symptoms of methaemoglobinaemia. Individuals who are chronically exposed to such chemicals may have blueness of the lips when methaemoglobin levels are approximately 10% or greater. They may have no other overt effects. The blood has a characteristic chocolate brown colour with methaemoglobinaemia. Treatment consists of avoiding further exposure. Significant symptoms may be present, usually at methaemoglobin levels greater than 40%. Therapy with methylene blue or ascorbic acid can accelerate reduction of the methaemoglobin level. Individuals with glucose-6-phosphate dehydrogenase deficiency may have accelerated haemolysis when treated with methylene blue (see below for discussion of glucose-6-phosphate dehydrogenase deficiency).
There are inherited disorders leading to persistent methaemoglobinaemia, either due to heterozygosity for an abnormal haemoglobin, or to homozygosity for deficiency of red cell NADH-dependent methaemoglobin reductase. Individuals who are heterozygous for this enzyme deficiency will not be able to decrease elevated methaemoglobin levels caused by chemical exposures as rapidly as will individuals with normal enzyme levels.
In addition to oxidizing the iron component of haemoglobin, many of the chemicals causing methaemoglobinaemia, or their metabolites, are also relatively non-specific oxidizing agents, which at high levels can cause a Heinz-body haemolytic anaemia. This process is characterized by oxidative denaturation of haemoglobin, leading to the formation of punctate membrane-bound red cell inclusions known as Heinz bodies, which can be identified with special stains. Oxidative damage to the red cell membrane also occurs. While this may lead to significant haemolysis, the compounds listed in Table 1 primarily produce their adverse effects through the formation of methaemoglobin, which may be life threatening, rather than through haemolysis, which is usually a limited process.
In essence, two different red cell defence pathways are involved: (1) the NADH-dependent methaemoglobin reductase required to reduce methaemoglobin to normal haemoglobin; and (2) the NADPH-dependent process through the hexose monophosphate (HMP) shunt, leading to the maintenance of reduced glutathione as a means to defend against oxidizing species capable of producing Heinz-body haemolytic anaemia (figure 1). Heinz-body haemolysis can be exacerbated by the treatment of methaemoglobinaemic patients with methylene blue because it requires NADPH for its methaemoglobin-reducing effects. Haemolysis will also be a more prominent part of the clinical picture in individuals with (1)deficiencies in one of the enzymes of the NADPH oxidant defence pathway, or (2) an inherited unstable haemoglobin. Except for the glucose-6-phosphate dehydrogenase (G6PD) deficiency, described later in this chapter, these are relatively rare disorders.
Figure 1. Red blood cell enzymes of oxidant defence and related reactions
GSH + GSH + (O) ←-Glutathione peroxidase-→ GSSG + H2O
GSSG + 2NADPH ←-Glutathione peroxidase-→ 2GSH + 2NADP
Glucose-6-Phosphate + NADP ←-G6PD-→ 6-Phosphogluconate + NADPH
Fe+++·Haemoglobin (Methaemoglobin) + NADH ←-Methaemoglobin reductase-→ Fe++·Haemoglobin
Another form of haemoglobin alteration produced by oxidizing agents is a denatured species known as sulphaemoglobin. This irreversible product can be detected in the blood of individuals with significant methaemoglobinaemia produced by oxidant chemicals. Sulphaemoglobin is the name also given, and more appropriately, to a specific product formed during hydrogen sulphide poisoning.
Haemolytic agents: There are a variety of haemolytic agents in the workplace. For many the toxicity of concern is methaemoglobinaemia. Other haemolytic agents include naphthalene and its derivatives. In addition, certain metals, such as copper, and organometals, such as tributyl tin, will shorten red cell survival, at least in animal models. Mild haemolysis can also occur during traumatic physical exertion (march haemoglobinuria); a more modern observation is elevated white blood counts with prolonged exertion (jogger’s leucocytosis). The most important of the metals that affects red cell formation and survival in workers is lead, described in detail in the chemicals section of this Encyclopaedia.
Arsine: The normal red blood cell survives in the circulation for 120 days. Shortening of this survival can lead to anaemia if not compensated by an increase in red cell production by the bone marrow. There are essentially two types of haemolysis: (1) intravascular haemolysis, in which there is an immediate release of haemoglobin within the circulation; and (2) extravascular haemolysis, in which red cells are destroyed within the spleen or the liver.
One of the most potent intravascular haemolysins is arsine gas (AsH3). Inhalation of a relatively small amount of this agent leads to swelling and eventual bursting of red blood cells within the circulation. It may be difficult to detect the causal relation of workplace arsine exposure to an acute haemolytic episode (Fowler and Wiessberg 1974). This is partly because there is frequently a delay between exposure and onset of symptoms, but primarily because the source of exposure is often not evident. Arsine gas is made and used commercially, often now in the electronics industry. However, most of the published reports of acute haemolytic episodes have been through the unexpected liberation of arsine gas as an unwanted by-product of an industrial process—for example, if acid is added to a container made of arsenic-contaminated metal. Any process that chemically reduces arsenic, such as acidification, can lead to the liberation of arsine gas. As arsenic can be a contaminant of many metals and organic materials, such as coal, arsine exposure can often be unexpected. Stibine, the hydride of antimony, appears to produce a haemolytic effect similar to arsine.
Death can occur directly due to complete loss of red blood cells. (A haematocrit of zero has been reported.) However, a major concern at arsine levels less than those producing complete haemolysis is acute renal failure due to the massive release of haemoglobin within the circulation. At much higher levels, arsine may produce acute pulmonary oedema and possibly direct renal effects. Hypotension may accompany the acute episode. There is usually a delay of at least a few hours between inhalation of arsine and the onset of symptoms. In addition to red urine due to haemoglobinuria, the patient will frequently complain of abdominal pain and nausea, symptoms that occur concomitantly with acute intravascular haemolysis from a number of causes (Neilsen 1969).
Treatment is aimed at maintenance of renal perfusion and transfusion of normal blood. As the circulating red cells affected by arsine appear to some extent to be doomed to intravascular haemolysis, an exchange transfusion in which arsine-exposed red cells are replaced by unexposed cells would appear to be optimal therapy. As in severe life-threatening haemorrhage, it is important that replacement red cells have adequate 2,3-diphosphoglyceric acid (DPG) levels so as to be able to deliver oxygen to the tissue.
Other Haematological Disorders
White blood cells
There are a variety of drugs, such as propylthiourea (PTU), which are known to affect the production or survival of circulating polymorphonuclear leucocytes relatively selectively. In contrast, non-specific bone marrow toxins affect the precursors of red cells and platelets as well. Workers engaged in the preparation or administration of such drugs should be considered at risk. There is one report of complete granulocytopenia in a worker poisoned with dinitrophenol. Alteration in lymphocyte number and function, and particularly of subtype distribution, is receiving more attention as a possible subtle mechanism of effects due to a variety of chemicals in the workplace or general environment, particularly chlorinated hydrocarbons, dioxins and related compounds. Validation of the health implications of such changes is required.
Coagulation
Similar to leucopenia, there are many drugs that selectively decrease the production or survival of circulating platelets, which could be a problem in workers involved in the preparation or administration of such agents. Otherwise, there are only scattered reports of thrombocytopenia in workers. One study implicates toluene diisocyanate (TDI) as a cause of thrombocytopenic purpura. Abnormalities in the various blood factors involved in coagulation are not generally noted as a consequence of work. Individuals with pre-existing coagulation abnormalities, such as haemophilia, often have difficulty entering the workforce. However, although a carefully considered exclusion from a few selected jobs is reasonable, such individuals are usually capable of normal functioning at work.
Haematological Screening and Surveillance in the Workplace
Markers of susceptibility
Due in part to the ease in obtaining samples, more is known about inherited variations in human blood components than for those in any other organ. Extensive studies sparked by recognition of familial anaemias have led to fundamental knowledge concerning the structural and functional implications of genetic alterations. Of pertinence to occupational health are those inherited variations that might lead to an increased susceptibility to workplace hazards. There are a number of such testable variations that have been considered or actually used for the screening of workers. The rapid increase in knowledge concerning human genetics makes it a certainty that we will have a better understanding of the inherited basis of variation in human response, and we will be more capable of predicting the extent of individual susceptibility through laboratory tests.
Before discussing the potential value of currently available susceptibility markers, the major ethical considerations in the use of such tests in workers should be emphasized. It has been questioned whether such tests favour exclusion of workers from a site rather than a focus on improving the worksite for the benefit of the workers. At the very least, before embarking on the use of a susceptibility marker at a workplace, the goals of the testing and consequences of the findings must be clear to all parties.
The two markers of haematological susceptibility for which screening has taken place most frequently are sickle cell trait and G6PD deficiency. The former is at most of marginal value in rare situations, and the latter is of no value whatsoever in most of the situations for which it has been advocated (Goldstein, Amoruso and Witz 1985).
Sickle cell disease, in which there is homozygosity for haemoglobin S (HbS), is a fairly common disorder among individuals of African descent. It is a relatively severe disease that often, but not always, precludes entering the workforce. The HbS gene may be inherited with other genes, such as HbC, which may reduce the severity of its effects. The basic defect in individuals with sickle cell disease is the polymerization of HbS, leading to microinfarction. Microinfarction can occur in episodes, known as sickle cell crises, and can be precipitated by external factors, particularly those leading to hypoxia and, to a lesser extent, dehydration. With a reasonably wide variation in the clinical course and well-being of those with sickle cell disease, employment evaluation should focus on the individual case history. Jobs that have the possibility of hypoxic exposures, such as those requiring frequent air travel, or those with a likelihood of significant dehydration, are not appropriate.
Much more common than sickle cell disease is sickle cell trait, the heterozygous condition in which there is inheritance of one gene for HbS and one for HbA. Individuals with this genetic pattern have been reported to undergo sickle cell crisis under extreme conditions of hypoxia. Some consideration has been given to excluding individuals with sickle cell trait from workplaces where hypoxia is a common risk, probably limited to the jobs on military aircraft or submarines, and perhaps on commercial aircraft. However, it must be emphasized that individuals with sickle cell trait do very well in almost every other situation. For example, athletes with sickle cell trait had no adverse effects from competing at the altitude of Mexico City (2,200m, or 7,200ft) during the 1968 Summer Olympics. Accordingly, with the few exceptions described above, there is no reason to consider exclusion or modification of work schedules for those with sickle cell trait.
Another common genetic variant of a red blood cell component is the A– form of G6PD deficiency. It is inherited on the X chromosome as a sex-linked recessive gene and is present in approximately one in seven Black males and one in 50 Black females in the United States. In Africa, the gene is particularly prevalent in areas of high malaria risk. As with sickle cell trait, G6PD deficiency provides a protective advantage against malaria. Under usual circumstances, individuals with this form of G6PD deficiency have red blood counts and indices within the normal range. However, due to the inability to regenerate reduced glutathione, their red blood cells are susceptible to haemolysis following ingestion of oxidant drugs and in certain disease states. This susceptibility to oxidizing agents has led to workplace screening on the erroneous assumption that individuals with the common A– variant of G6PD deficiency will be at risk from the inhalation of oxidant gases. In fact, it would require exposure to levels many times higher than the levels at which such gases would cause fatal pulmonary oedema before the red cells of G6PD-deficient individuals would receive oxidant stress sufficient to be of concern (Goldstein, Amoruso and Witz 1985). G6PD deficiency will increase the likelihood of overt Heinz-body haemolysis in individuals exposed to aniline dyes and other methaemoglobin-provoking agents (Table 1), but in these cases the primary clinical problem remains the life-threatening methaemoglobinaemia. While knowledge of G6PD status might be useful in such cases, primarily to guide therapy, this knowledge should not be used to exclude workers from the workplace.
There are many other forms of familial G6PD deficiency, all far less common then the A– variant (Beutler 1990). Certain of these variants, particularly in individuals from the Mediterranean basin and Central Asia, have much lower levels of G6PD activity in their red blood cells. Consequently the affected individual can be severely compromised by ongoing haemolytic anaemia. Deficiencies in other enzymes active in defence against oxidants have also been reported as have unstable haemoglobins that render the red cell more susceptible to oxidant stress in the same manner as in G6PD deficiency.
Surveillance
Surveillance differs substantially from clinical testing in both the evaluation of ill patients and the regular screening of presumably healthy individuals. In an appropriately designed surveillance programme, the aim is to prevent overt disease by picking up subtle early changes through the use of laboratory testing. Therefore, a slightly abnormal finding should automatically trigger a response—or at least a thorough review—by physicians.
In the initial review of haematological surveillance data in a workforce potentially exposed to a haematotoxin such as benzene, there are two major approaches that are particularly helpful in distinguishing false positives. The first is the degree of the difference from normal. As the count gets further removed from the normal range, there is a rapid drop-off in the likelihood that it represents just a statistical anomaly. Second, one should take advantage of the totality of data for that individual, including normal values, keeping in mind the wide range of effects produced by benzene. For example, there is a much greater probability of a benzene effect if a slightly low platelet count is accompanied by a low-normal white blood cell count, a low-normal red cell count, and a high-normal red cell mean corpuscular volume (MCV). Conversely, the relevance of this same platelet count to benzene haematotoxicity can be discounted if the other blood counts are at the opposite end of the normal spectrum. These same two considerations can be used in judging whether the individual should be removed from the workforce while awaiting further testing and whether the additional testing should consist only of a repeat complete blood count (CBC).
If there is any doubt as to the cause of the low count, the entire CBC should be repeated. If the low count is due to laboratory variability or some short-term biological variability within the individual, it is less likely that the blood count will again be low. Comparison with preplacement or other available blood counts should help distinguish those individuals who have an inherent tendency to be on the lower end of the distribution. Detection of an individual worker with an effect due to a haematological toxin should be considered a sentinel health event, prompting careful investigation of working conditions and of co-workers (Goldstein 1988).
The wide range in normal laboratory values for blood counts can present an even greater challenge since there can be a substantial effect while counts are still within the normal range. For example, it is possible that a worker exposed to benzene or ionizing radiation may have a fall in haematocrit from 50 to 40%, a fall in the white blood cell count from 10,000 to 5,000 per cubic millimetre and a fall in the platelet count from 350,000 to 150,000 per cubic millimetre—that is, more than a 50% decrease in platelets; yet all these values are within the “normal” range of blood counts. Accordingly, a surveillance programme that looks solely at “abnormal” blood counts may miss significant effects. Therefore, blood counts that decrease over time while staying in the normal range need particular attention.
Another challenging problem in workplace surveillance is the detection of a slight decrease in the mean blood count of an entire exposed population—for example, a decrease in mean white blood cell count from 7,500 to 7,000 per cubic millimetre because of a widespread exposure to benzene or ionizing radiation. Detection and appropriate evaluation of any such observation requires meticulous attention to standardization of laboratory test procedures, the availability of an appropriate control group and careful statistical analysis.
More...
Cognitive Disorders
A cognitive disorder is defined as a significant decline in one’s ability to process and recall information. The DSM IV (American Psychiatric Association 1994) describes three major types of cognitive disorder: delirium, dementia and amnestic disorder. A delirium develops over a short period of time and is characterized by an impairment of short-term memory, disorientation and perceptual and language problems. Amnestic disorders are characterized by impairment of memory such that sufferers are unable to learn and recall new information. However, no other declines in cognitive functioning are associated with this type of disorder. Both delirium and amnestic disorders are usually due to the physiological effects of a general medical condition (e.g., head injuries, high fevers) or of substance use. There is little reason to suspect that occupational factors play a direct role in the development of these disorders.
However, research has suggested that occupational factors may influence the likelihood of developing the multiple cognitive deficits involved in dementia. Dementia is characterized by memory impairment and at least one of the following problems: (a) reduced language function; (b) a decline in one’s ability to think abstractly; or (c) an inability to recognize familiar objects even though one’s senses (e.g., vision, hearing, touch) are not impaired. Alzheimer’s disease is the most common type of dementia.
The prevalence of dementia increases with age. Approximately 3% of people over the age of 65 years will suffer from a severe cognitive impairment during any given year. Recent studies of elderly populations have found a link between a person’s occupational history and his or her likelihood of suffering from dementia. For example, a study of the rural elderly in France (Dartigues et al. 1991) found that people whose primary occupation had been farm worker, farm manager, provider of domestic service or blue-collar worker had a significantly elevated risk of having a severe cognitive impairment when compared to those whose primary occupation had been teacher, manager, executive or professional. Furthermore, this elevated risk was not due to differences between the groups of workers in terms of age, sex, education, drinking of alcoholic beverages, sensory impairments or the taking of psychotropic drugs.
Because dementia is so rare among people younger than 65 years, no study has examined occupation as a risk factor among this population. However, a large study in the United States (Farmer et al. 1995) has shown that people under the age of 65 who have high levels of education are less likely to experience declines in cognitive functioning than are similarly aged people with less education. The authors of this study commented that education level may be a “marker variable” that is actually reflecting the effects of occupational exposures. At this point, such a conclusion is highly speculative.
Although several studies have found an association between one’s principal occupation and dementia among the elderly, the explanation or mechanism underlying the association is not known. One possible explanation is that some occupations involve higher exposure to toxic materials and solvents than do other occupations. For example, there is growing evidence that toxic exposures to pesticides and herbicides can have adverse neurological effects. Indeed, it has been suggested that such exposures may explain the elevated risk of dementia found among farm workers and farm managers in the French study described above. In addition, some evidence suggests that the ingestion of certain minerals (e.g., aluminium and calcium as components of drinking water) may affect the risk of cognitive impairment. Occupations may involve differential exposure to these minerals. Further research is needed to explore possible pathophysiological mechanisms.
Psychosocial stress levels of employees in various occupations may also contribute to the link between occupation and dementia. Cognitive disorders are not among the mental health problems that are commonly thought to be stress related. A review of the role of stress in psychiatric disorders focused on anxiety disorders, schizophrenia and depression, but made no mention of cognitive disorders (Rabkin 1993). One type of disorder, called dissociative amnesia, is characterized by an inability to recall a previous traumatic or stressful event but carries with it no other type of memory impairment. This disorder is obviously stress-related, but is not categorized as a cognitive disorder according to the DSM IV.
Although psychosocial stress has not been explicitly linked to the onset of cognitive disorders, it has been demonstrated that the experience of psychosocial stress affects how people process information and their ability to recall information. The arousal of the autonomic nervous system that often accompanies exposure to stressors alerts a person to the fact that “all is not as expected or as it should be” (Mandler 1993). At first, this arousal may enhance a person’s ability to focus attention on the central issues and to solve problems. However, on the negative side, the arousal uses up some of the “available conscious capacity” or the resources that are available for processing incoming information. Thus, high levels of psychosocial stress ultimately (1) limit one’s ability to scan all of the relevant available information in an orderly fashion, (2) interfere with one’s ability to rapidly detect peripheral cues, (3) decrease one’s ability to sustain focused attention and (4) impair some aspects of memory performance. To date, even though these decrements in information-processing skills can result in some of the symptomatology associated with cognitive disorders, no relationship has been demonstrated between these minor impairments and the likelihood of exhibiting a clinically diagnosed cognitive disorder.
A third possible contributor to the relationship between occupation and cognitive impairment may be the level of mental stimulation demanded by the job. In the study of rural elderly residents in France described above, the occupations associated with the lowest risk of dementia were those that involved substantial intellectual activity (e.g., physician, teacher, lawyer). One hypothesis is that the intellectual activity or mental stimulation inherent in these jobs produces certain biological changes in the brain. These changes, in turn, protect the worker from decline in cognitive function. The well-documented protective effect of education on cognitive functioning is consistent with such a hypothesis.
It is premature to draw any implications for prevention or treatment from the research findings summarized here. Indeed, the association between one’s lifetime principal occupation and the onset of dementia among the elderly may not be due to occupational exposures or the nature of the job. Rather, the relationship between occupation and dementia may be due to differences in the characteristics of workers in various occupations. For example, differences in personal health behaviours or in access to quality medical care may account for at least part of the effect of occupation. None of the published descriptive studies can rule out this possibility. Further research is needed to explore whether specific psychosocial, chemical and physical occupational exposures are contributing to the aetiology of this cognitive disorder.
Karoshi: Death from Overwork
What Is Karoshi?
Karoshi is a Japanese word which means death from overwork. The phenomenon was first identified in Japan, and the word is being adopted internationally (Drinkwater 1992). Uehata (1978) reported 17 karoshi cases at the 51st annual meeting of the Japan Association of Industrial Health. Among them seven cases were compensated as occupational diseases, but ten cases were not. In 1988 a group of lawyers established the National Defense Counsel for Victims of Karoshi (1990) and started telephone consultation to handle inquiries about karoshi-related workers’ compensation insurance. Uehata (1989) described karoshi as a sociomedical term that refers to fatalities or associated work disability due to cardiovascular attacks (such as strokes, myocardial infarction or acute cardiac failure) which could occur when hypertensive arteriosclerotic diseases are aggravated by a heavy workload. Karoshi is not a pure medical term. The media have frequently used the word because it emphasizes that sudden deaths (or disabilities) were caused by overwork and should be compensated. Karoshi has become an important social problem in Japan.
Research on Karoshi
Uehata (1991a) conducted a study of 203 Japanese workers (196 males and seven females) who had cardiovascular attacks. They or their next of kin consulted with him regarding workers’ compensation claims between 1974 and 1990. A total of 174 workers had died; 55 cases had already been compensated as occupational disease. A total of 123 workers had suffered strokes (57 arachnoidal bleedings, 46 cerebral bleedings, 13 cerebral infarctions, seven unknown types); 50, acute heart failure; 27, myocardial infarctions; and four, aortic ruptures. Autopsies were performed in only 16 cases. More than half of the workers had histories of hypertension, diabetes or other atherosclerotic problems. A total of 131 cases had worked for long hours—more than 60 hours per week, more than 50 hours overtime per month or more than half of their fixed holidays. Eighty-eight workers had identifiable trigger events within 24 hours before their attack. Uehata concluded that these were mostly male workers, working for long hours, with other stressful overload, and that these working styles exacerbated their other lifestyle habits and resulted in the attacks, which were finally triggered by minor work-related troubles or events.
Karasek Model and Karoshi
According to the demand-control model by Karasek (1979), a high-strain job—one with a combination of high demand and low control (decision latitude)—increases the risk of psychological strain and physical illness; an active job—one with a combination of high demand and high control—requires learning motivation to develop new behaviour patterns. Uehata (1991b) reported that the jobs in karoshi cases were characterized by a higher degree of work demands and lower social support, whereas the degree of work control varied greatly. He described the karoshi cases as very delighted and enthusiastic about their work, and consequently likely to ignore their needs for regular rest and so on—even the need for health care. It is suggested that workers in not only high-strain jobs but also active jobs could be at high risk. Managers and engineers have high decision latitude. If they have extremely high demands and are enthusiastic in their work, they may not control their working hours. Such workers may be a risk group for karoshi.
Type A Behaviour Pattern in Japan
Friedman and Rosenman (1959) proposed the concept of Type A behaviour pattern (TABP). Many studies have showed that TABP is related to the prevalence or incidence of coronary heart disease (CHD).
Hayano et al. (1989) investigated the characteristics of TABP in Japanese employees using the Jenkins Activity Survey (JAS). Responses of 1,682 male employees of a telephone company were analysed. The factor structure of the JAS among the Japanese was in most respects equal to that found in the Western Collaborative Group Study (WCGS). However, the average score of factor H (hard-driving and competitiveness) among the Japanese was considerably lower than that in the WCGS.
Monou (1992) reviewed TABP research in Japan and summarized as follows: TABP is less prevalent in Japan than in the United States; the relationship between TABP and coronary heart disease in Japan seems to be significant but weaker than that in the US; TABP among Japanese places more emphasis on “workaholism” and “directivity into the group” than in the US; the percentage of highly hostile individuals in Japan is lower than in the US; there is no relationship between hostility and CHD.
Japanese culture is quite different from those of Western countries. It is strongly influenced by Buddhism and Confucianism. Generally speaking, Japanese workers are organization centred. Cooperation with colleagues is emphasized rather than competition. In Japan, competitiveness is a less important factor for coronary-prone behaviour than job involvement or a tendency to overwork. Direct expression of hostility is suppressed in Japanese society. Hostility may be expressed differently than in Western countries.
Working Hours of Japanese Workers
It is well known that Japanese workers work long hours compared with workers in other developed industrial countries. Normal annual working hours of manufacturing workers in 1993 were 2,017 hours in Japan; 1,904 in the United States; 1,763 in France; and 1,769 in the UK (ILO 1995). However, Japanese working hours are gradually decreasing. Average annual working hours of manufacturing employees in enterprises with 30 employees or more was 2,484 hours in 1960, but 1,957 hours in 1994. Article 32 of the Labor Standards Law, which was revised in 1987, provides for a 40-hour week. The general introduction of the 40-hour week is expected to take place gradually in the 1990s. In 1985, the 5-day work week was granted to 27% of all employees in enterprises with 30 employees or more; in 1993, it was granted to 53% of such employees. The average worker was allowed 16 paid holidays in 1993; however, workers actually used an average of 9 days. In Japan, paid holidays are few, and workers tend to save them to cover absence due to sickness.
Why do Japanese workers work such long hours? Deutschmann (1991) pointed out three structural conditions underlying the present pattern of long working hours in Japan: first, the continuing need of Japanese employees to increase their income; second, the enterprise-centred structure of industrial relations; and third, the holistic style of Japanese personnel management. These conditions were based on historical and cultural factors. Japan was defeated in war in 1945 for the first time in history. After the war Japan was a cheap wage country. The Japanese were used to working long and hard to earn their subsistence. As labour unions were cooperative with employers, there have been relatively few labour disputes in Japan. Japanese companies adopted the seniority-oriented wage system and lifetime employment. The number of hours is a measure of the loyalty and cooperativeness of an employee, and becomes a criterion for promotion. Workers are not forced to work long hours; they are willing to work for their companies, as if the company is their family. Working life has priority over family life. Such long working hours have contributed to the remarkable economic achievements of Japan.
National Survey of Workers’ Health
The Japanese Ministry of Labour conducted surveys on the state of employees’ health in 1982, 1987 and 1992. In the survey in 1992, 12,000 private worksites employing 10 or more workers were identified, and 16,000 individual workers from them were randomly selected nationwide based on industry and job classification to fill out questionnaires. The questionnaires were mailed to a representative at the workplace who then selected workers to complete the survey.
Sixty-five per cent of these workers complained of physical fatigue due to their usual work, and 48% complained of mental fatigue. Fifty-seven per cent of workers stated that they had strong anxieties, worries or stress concerning their job or working life. The prevalence of stressed workers was increasing, as the prevalence had been 55% in 1987 and 51% in 1982. The main causes of stress were: unsatisfactory relations in the workplace, 48%; quality of work, 41%; quantity of work, 34%.
Eighty-six per cent of these worksites conducted periodic health examinations. Worksite health promotion activities were conducted at 44% of the worksites. Of these worksites, 48% had sports events, 46% had exercise programmes and 35% had health counselling.
National Policy to Protect and PromoteWorkers’ Health
The purpose of the Industrial Safety and Health Law in Japan is to secure the safety and health of workers in workplaces as well as to facilitate the establishment of a comfortable working environment. The law states that the employer shall not only comply with the minimum standards for preventing occupational accidents and diseases, but also endeavour to ensure the safety and health of workers in workplaces through the realization of a comfortable working environment and the improvement of working conditions.
Article 69 of the law, amended in 1988, states that the employer shall make continuous and systematic efforts for the maintenance and promotion of workers’ health by taking appropriate measures, such as providing health education and health counselling services to the workers. The Japanese Ministry of Labour publicly announced guidelines for measures to be taken by employers for the maintenance and promotion of workers’ health in 1988. It recommends worksite health promotion programmes called the Total Health Promotion Plan (THP): exercise (training and counselling), health education, psychological counselling and nutritional counselling, based on the health status of employees.
In 1992, the guidelines for the realization of a comfortable working environment were announced by the Ministry of Labour in Japan. The guidelines recommend the following: the working environment should be properly maintained under comfortable conditions; work conditions should be improved to reduce the workload; and facilities should be provided for the welfare of employees who need to recover from fatigue. Low-interest loans and grants for small and medium-sized enterprises for workplace improvement measures have been introduced to facilitate the realization of a comfortable working environment.
Conclusion
The evidence that overwork causes sudden death is still incomplete. More studies are needed to clarify the causal relationship. To prevent karoshi, working hours should be reduced. Japanese national occupational health policy has focused on work hazards and health care of workers with problems. The psychological work environment should be improved as a step towards the goal of a comfortable working environment. Health examinations and health promotion programmes for all workers should be encouraged. These activities will prevent karoshi and reduce stress.
Introduction
Magnitude of the Problem
The first clear-cut evidence of cancer causation involved an occupational carcinogen (Checkoway, Pearce and Crawford-Brown 1989). Pott (1775) identified soot as the cause of scrotal cancer in London chimney-sweeps, and graphically described the abysmal working conditions, which involved children climbing up narrow chimneys that were still hot. Despite this evidence, reports of the need to prevent fires in chimneys were used to delay legislation on child labour in this industry until 1840 (Waldron 1983). An experimental model of soot carcinogenesis was first demonstrated in the 1920s (Decoufle 1982), 150 years after the original epidemiological observation.
In subsequent years, a number of other occupational causes of cancer have been demonstrated through epidemiological studies (although the association with cancer has usually first been noted by occupational physicians or by workers). These include arsenic, asbestos, benzene, cadmium, chromium, nickel and vinyl chloride. Such occupational carcinogens are very important in public health terms because of the potential for prevention through regulation and improvements in industrial hygiene practices (Pearce and Matos 1994). In most instances, these are hazards which markedly increase the relative risk of a particular type or types of cancer. It is possible that other occupational carcinogens remain undetected because they involve only a small increase in risk or because they simply have not been studied (Doll and Peto 1981). Some key facts about occupational cancer are given in table 1.
Table 1. Occupational cancer: Key facts.
- Some 20 agents and mixtures are established occupational carcinogens; a similar number of chemicals are highly suspected occupational carcinogens.
- In industrialized countries, occupation is causally linked to 2 to 8% of all cancers; among exposed workers, however, this proportion is higher.
- No reliable estimates are available on either the burden of occupational cancer or the extent of workplace exposure to carcinogens in developing countries.
- The relatively low overall burden of occupational cancer in industrialized countries is the result of strict regulations on several known carcinogens; exposure to other known or highly suspected agents, however, is still allowed.
- Although several occupational cancers are listed as occupational diseases in many countries, a very small fraction of cases is actually recognized and compensated.
- Occupational cancer is-to a very large extent-a preventable disease.
Occupational causes of cancer have received considerable emphasis in epidemiological studies in the past. However, there has been much controversy regarding the proportion of cancers which are attributable to occupational exposures, with estimates ranging from 4 to 40% (Higginson 1969; Higginson and Muir 1976; Wynder and Gori 1977; Higginson and Muir 1979; Doll and Peto 1981; Hogan and Hoel 1981; Vineis and Simonato 1991; Aitio and Kauppinen 1991). The attributable cancer risk is the total cancer experience in a population that would not have occurred if the effects associated with the occupational exposures of concern were absent. It may be estimated for the exposed population, as well as for a broader population. A summary of existing estimates is shown in table 2. Universal application of the International Classification of Diseases is what makes such tabulations possible (see box).
Table 2. Estimated proportions of cancer (PAR) attributable to occupations in selected studies.
| Study | Population | PAR and cancer site | Comments |
| Higginson 1969 | Not stated | 1% Oral cancer 1-2% Lung cancer 10% Bladder cancer 2% Skin cancer |
No detailed presentation of exposure levels and other assumptions |
| Higginson and Muir 1976 | Not stated | 1-3% Total cancer | No detailed presentation of assumptions |
| Wynder and Gori 1977 | Not stated | 4% Total cancer in men, 2% for women |
Based on one PAR for bladder cancer and two personal communications |
| Higginson and Muir 1979 | West Midland, United Kingdom | 6% Total cancer in men, 2% total cancer |
Based on 10% of non-tobacco related lung cancer, mesothelioma, bladder cancer (30%), and leukaemia in women (30%) |
| Doll and Peto 1981 | United States early 1980 | 4% (range 2-8%) Total cancer |
Based on all studied cancer sites; reported as ‘tentative’ estimate |
| Hogan and Hoel 1981 | United States | 3% (range 1.4-4%) Total cancer |
Risk associated with occupational asbestos exposure |
| Vineis and Simonato 1991 | Various | 1-5% Lung cancer, 16-24% bladder cancer |
Calculations on the basis of data from case-control studies. Percentage for lung cancer considers only exposure to asbestos. In a study with a high proportion of subjects exposed to ionising radiation, a 40% PAR was estimated. Estimates of PAR in a few studies on bladder cancer were between 0 and 3%. |
The International Classification of Diseases
Human diseases are classified according to the International Classification of Diseases (ICD), a system that was started in 1893 and is regularly updated under the coordination of the World Health Organization. The ICD is used in almost all countries for tasks such as death certification, cancer registration and hospital discharge diagnosis. The Tenth Revision (ICD-10), which was approved in 1989 (World Health Organization 1992), differs considerably from the previous three revisions, which are similar to each other and have been in use since the 1950s. It is therefore likely that the Ninth Revision (ICD-9, World Health Organization 1978), or even earlier revisions, will still be used in many countries during the coming years.
The large variability in the estimates arises from the differences in the data sets used and the assumptions applied. Most of the published estimates on the fraction of cancers attributed to occupational risk factors are based on rather simplified assumptions. Furthermore, although cancer is relatively less common in developing countries due to the younger age structure (Pisani and Parkin 1994), the proportion of cancers due to occupation may be higher in developing countries due to the relatively high exposures which are encountered (Kogevinas, Boffetta and Pearce 1994).
The most generally accepted estimates of cancers attributable to occupations are those presented in a detailed review on the causes of cancer in the population of the United States in 1980 (Doll and Peto 1981). Doll and Peto concluded that about 4% of all the deaths due to cancer may be caused by occupational carcinogens within “acceptable limits” (i.e., still plausible in view of all the evidence at hand) of 2 and 8%. These estimates being proportions, they are dependent on how causes other than occupational exposures contribute to produce cancers. For example, the proportion would be higher in a population of lifetime non-smokers (such as the Seventh-Day Adventists) and lower in a population in which, say, 90% are smokers. Also the estimates do not apply uniformly to both sexes or to different social classes. Furthermore, if one considers not the whole population (to which the estimates refer), but the segments of the adult population in which exposure to occupational carcinogens almost exclusively occurs (manual workers in mining, agriculture and industry, broadly taken, who in the United States numbered 31 million out of a population, aged 20 and over, of 158 million in the late 1980s), the proportion of 4% in the overall population would increase to about 20% among those exposed.
Vineis and Simonato (1991) provided estimates on the number of cases of lung and bladder cancer attributable to occupation. Their estimates were derived from a detailed review of case-control studies, and demonstrate that in specific populations located in industrial areas, the proportion of lung cancer or bladder cancer from occupational exposures may be as high as 40% (these estimates being dependent not only on the local prevailing exposures, but also to some extent on the method of defining and assessing exposure).
Mechanisms and Theories of Carcinogenesis
Studies of occupational cancer are complicated because there are no “complete” carcinogens; that is, occupational exposures increase the risk of developing cancer, but this future development of cancer is by no means certain. Furthermore, it may take 20 to 30 years (and at least five years) between an occupational exposure and the subsequent induction of cancer; it may also take several more years for cancer to become clinically detectable and for death to occur (Moolgavkar et al. 1993). This situation, which also applies to non-occupational carcinogens, is consistent with current theories of cancer causation.
Several mathematical models of cancer causation have been proposed (e.g., Armitage and Doll 1961), but the model which is simplest and most consistent with current biological knowledge is that of Moolgavkar (1978). This assumes that a healthy stem cell occasionally mutates (initiation); if a particular exposure encourages the proliferation of intermediate cells (promotion) then it becomes more likely that at least one cell will undergo one or more further mutations producing a malignant cancer (progression) (Ennever 1993).
Thus, occupational exposures can increase the risk of developing cancer either by causing mutations in DNA or by various “epigenetic” mechanisms of promotion (those not involving damage to DNA), including increased cell proliferation. Most occupational carcinogens which have been discovered to date are mutagens, and therefore appear to be cancer initiators. This explains the long “latency” period which is required for further mutations to occur; in many instances the necessary further mutations may never occur, and cancer may never develop.
In recent years, there has been increasing interest in occupational exposures (e.g., benzene, arsenic, phenoxy herbicides) which do not appear to be mutagens, but which may act as promoters. Promotion may occur relatively late in the carcinogenic process, and the latency period for promoters may therefore be shorter than for initiators. However, the epidemiological evidence for cancer promotion remains very limited at this time (Frumkin and Levy 1988).
Transfer of Hazards
A major concern in recent decades has been the problem of the transfer of hazardous industries to the developing world (Jeyaratnam 1994). Such transfers have occurred in part due to the stringent regulation of carcinogens and increasing labour costs in the industrialized world, and in part from low wages, unemployment and the push for industrialization in the developing world. For example, Canada now exports about half of its asbestos to the developing world, and a number of asbestos-based industries have been transferred to developing countries such as Brazil, India, Pakistan, Indonesia and South Korea (Jeyaratnam 1994). These problems are further compounded by the magnitude of the informal sector, the large numbers of workers who have little support from unions and other worker organizations, the insecure status of workers, the lack of legislative protection and/or the poor enforcement of such protection, the decreasing national control over resources, and the impact of the third world debt and associated structural adjustment programmes (Pearce et al. 1994).
As a result, it cannot be said that the problem of occupational cancer has been reduced in recent years, since in many instances the exposure has simply been transferred from the industrialized to the developing world. In some instances, the total occupational exposure has increased. Nevertheless, the recent history of occupational cancer prevention in industrialized countries has shown that it is possible to use substitutes for carcinogenic compounds in industrial processes without leading industry to ruin, and similar successes would be possible in developing countries if adequate regulation and control of occupational carcinogens were in place.
Prevention of Occupational Cancer
Swerdlow (1990) outlined a series of options for the prevention of exposure to occupational causes of cancer. The most successful form of prevention is to avoid the use of recognized human carcinogens in the workplace. This has rarely been an option in industrialized countries, since most occupational carcinogens have been identified by epidemiological studies of populations that were already occupationally exposed. However, at least in theory, developing countries could learn from the experience of industrialized countries and prevent the introduction of chemicals and production processes that have been found to be hazardous to the health of workers.
The next best option for avoiding exposure to established carcinogens is their removal once their carcinogenicity has been established or suspected. Examples include the closure of plants making the bladder carcinogens 2-naphthylamine and benzidine in the United Kingdom (Anon 1965), termination of British gas manufacture involving coal carbonization, closure of Japanese and British mustard gas factories after the end of the Second World War (Swerdlow 1990) and gradual elimination of the use of benzene in the shoe industry in Istanbul (Aksoy 1985).
In many instances, however, complete removal of a carcinogen (without closing down the industry) is either not possible (because alternative agents are not available) or is judged politically or economically unacceptable. Exposure levels must therefore be reduced by changing production processes and through industrial hygiene practices. For example, exposures to recognized carcinogens such as asbestos, nickel, arsenic, benzene, pesticides and ionizing radiation have been progressively reduced in industrialized countries in recent years (Pearce and Matos 1994).
A related approach is to reduce or eliminate the activities that involve the heaviest exposures. For example, after an 1840 act was passed in England and Wales prohibiting chimney-sweeps from being sent up chimneys, the number of cases of scrotal cancer decreased (Waldron 1983). Exposure also can be minimized through the use of protective equipment, such as masks and protective clothing, or by imposing more stringent industrial hygiene measures.
An effective overall strategy in the control and prevention of exposure to occupational carcinogens generally involves a combination of approaches. One successful example is a Finnish registry which has as its objectives to increase awareness about carcinogens, to evaluate exposure at individual workplaces and to stimulate preventive measures (Kerva and Partanen 1981). It contains information on both workplaces and exposed workers, and all employers are required to maintain and update their files and to supply information to the registry. The system appears to have been at least partially successful in decreasing carcinogenic exposures in the workplace (Ahlo, Kauppinen and Sundquist 1988).
Occupational Carcinogens
The control of occupational carcinogens is based on the critical review of scientific investigations both in humans and in experimental systems. There are several review programmes being undertaken in different countries aimed at controlling occupational exposures which could be carcinogenic to humans. The criteria used in different programmes are not entirely consistent, leading occasionally to differences in the control of agents in different countries. For example, 4,4-methylene-bis-2-chloroaniline (MOCA) was classified as an occupational carcinogen in Denmark in 1976 and in the Netherlands in 1988, but only in 1992 has a notation “suspected human carcinogen” been introduced by the American Conference of Governmental Industrial Hygienists in the United States.
The International Agency for Research on Cancer (IARC) has established, within the framework of its Monographs programme, a set of criteria to evaluate the evidence of the carcinogenicity of specific agents. The IARC Monographs programme represents one of the most comprehensive efforts to review systematically and consistently cancer data, is highly regarded in the scientific community and serves as the basis for the information in this article. It also has an important impact on national and international occupational cancer control activities. The evaluation scheme is given in table 1.
Table 1. Evaluation of evidence of carcinogenicity in the IARC Monographs programme.
1. The evidence for the induction of cancer in humans, which obviously plays an important role in the identification of human carcinogens is considered. Three types of epidemiological studies contribute to an assessment of carcinogenicity in humans: cohort studies, case-control studies and correlation (or ecological) studies. Case reports of cancer in humans may also be reviewed. The evidence relevant to carcinogenicity from studies in humans is classified into one of the following categories:
- Sufficient evidence of carcinogenicity: A causal relationship has been established between exposure to the agent, mixture or exposure circumstance and human cancer. That is, a positive relationship has been observed between the exposure and cancer in studies in which chance, bias and confounding could be ruled out with reasonable confidence.
- Limited evidence of carcinogenicity: A positive association has been observed between exposure to the agent, mixture or exposure circumstance and cancer for which a causal interpretation is considered to be credible, but chance, bias or confounding could not be ruled out with reasonable confidence.
- Inadequate evidence of carcinogenicity: The available studies are of insufficient quality, consistency or statistical power to permit a conclusion regarding the presence or absence of a causal association, or no data on cancer in humans are available.
- Evidence suggesting lack of carcinogenicity: There are several adequate studies covering the full range of levels of exposure that human beings are known to encounter, which are mutually consistent in not showing a positive association between exposure to the agent and the studied cancer at any observed level of exposure.
2. Studies in which experimental animals (mainly rodents) are exposed chronically to potential carcinogens and examined for evidence of cancer are reviewed and the degree of evidence of carcinogenicity is then classified into categories similar to those used for human data.
3. Data on biological effects in humans and experimental animals that are of particular relevance are reviewed. These may include toxicological, kinetic and metabolic considerations and evidence of DNA binding, persistence of DNA lesions or genetic damage in exposed humans. Toxicological information, such as that on cytotoxicity and regeneration, receptor binding and hormonal and immunological effects, and data on structure-activity relationship are used when considered relevant to the possible mechanism of the carcinogenic action of the agent.
4. The body of evidence is considered as a whole, in order to reach an overall evaluation of the carcinogenicity to humans of an agent, mixture or circumstance of exposure (see table 2).
Agents, mixtures and exposure circumstances are evaluated within the IARC Monographs if there is evidence of human exposure and data on carcinogenicity (either in humans or in experimental animals) (for IARC classification groups, see table 2).
Table 2. IARC Monograph programme classification groups.
The agent, mixture or exposure circumstance is described according to the wording of one of the following categories:
| Group 1— | The agent (mixture) is carcinogenic to humans. The exposure circumstance entails exposures that are carcinogenic to humans. |
| Group 2A— | The agent (mixture) is probably carcinogenic to humans. The exposure circumstance entails exposures that are probably carcinogenic to humans. |
| Group 2B— | The agent (mixture) is possibly carcinogenic to humans. The exposure circumstance entails exposures that are possibly carcinogenic to humans. |
| Group 3— | The agent (mixture, exposure circumstance) is not classifiable as to its carcinogenicity to humans. |
| Group 4— | The agent (mixture, exposure circumstance) is probably not carcinogenic to humans. |
Known and Suspected Occupational Carcinogens
At present, there are 22 chemicals, groups of chemicals or mixtures for which exposures are mostly occupational, without considering pesticides and drugs, which are established human carcinogens (table 3). While some agents such as asbestos, benzene and heavy metals are currently widely used in many countries, other agents have mainly an historical interest (e.g., mustard gas and 2-naphthylamine).
Table 3. Chemicals, groups of chemicals or mixtures for which exposures are mostly occupational (excluding pesticides and drugs).
Group 1-Chemicals carcinogenic to humans1
| Exposure2 | Human target organ(s) | Main industry/use |
| 4-Aminobiphenyl (92-67-1) | Bladder | Rubber manufacture |
| Arsenic (7440-38-2) and arsenic compounds3 | Lung, skin | Glass, metals, pesticides |
| Asbestos (1332-21-4) | Lung, pleura, peritoneum | Insulation, filter material, textiles |
| Benzene (71-43-2) | Leukaemia | Solvent, fuel |
| Benzidine (92-87-5) | Bladder | Dye/pigment manufacture, laboratory agent |
| Beryllium (7440-41-7) and beryllium compounds | Lung | Aerospace industry/metals |
| Bis(chloromethyl)ether (542-88-11) | Lung | Chemical intermediate/by-product |
| Chloromethyl methylether (107-30-2) (technical grade) | Lung | Chemical intermediate/by-product |
| Cadmium (7440-43-9) and cadmium compounds | Lung | Dye/pigment manufacture |
| Chromium (VI) compounds | Nasal cavity, lung | Metal plating, dye/pigment manufacture |
| Coal-tar pitches (65996-93-2) | Skin, lung, bladder | Building material, electrodes |
| Coal-tars (8007-45-2) | Skin, lung | Fuel |
| Ethylene oxide (75-21-8) | Leukaemia | Chemical intermediate, sterilant |
| Mineral oils, untreated and mildly treated | Skin | Lubricants |
| Mustard gas (sulphur mustard) (505-60-2) |
Pharynx, lung | War gas |
| 2-Naphthylamine (91-59-8) | Bladder | Dye/pigment manufacture |
| Nickel compounds | Nasal cavity, lung | Metallurgy, alloys, catalyst |
| Shale-oils (68308-34-9) | Skin | Lubricants, fuels |
| Soots | Skin, lung | Pigments |
| Talc containing asbestiform fibers | Lung | Paper, paints |
| Vinyl chloride (75-01-4) | Liver, lung, blood vessels | Plastics, monomer |
| Wood dust | Nasal cavity | Wood industry |
1 Evaluated in the IARC Monographs, Volumes 1-63 (1972-1995) (excluding pesticides and drugs).
2 CAS Registry Nos. appear between parentheses.
3 This evaluation applies to the group of chemicals as a whole and not necessarily to all individual chemicals within the group.
An additional 20 agents are classified as probably carcinogenic to humans (Group 2A); they are listed in table 4, and include exposures that are currently prevalent in many countries, such as crystalline silica, formaldehyde and 1,3-butadiene. A large number of agents are classified as possible human carcinogens (Group 2B, table 5) - for example, acetaldehyde, dichloromethane and inorganic lead compounds. For the majority of these chemicals the evidence of carcinogenicity comes from studies in experimental animals.
Table 4. Chemicals, groups of chemicals or mixtures for which exposures are mostly occupational (excluding pesticides and drugs).
Group 2A—Probably carcinogenic to humans1
| Exposure2 | Suspected human target organ(s) | Main industry/use |
| Acrylonitrile (107-13-1) | Lung, prostate, lymphoma | Plastics, rubber, textiles, monomer |
| Benzidine-based dyes | – | Paper, leather, textile dyes |
| 1,3-Butadiene (106-99-0) | Leukaemia, lymphoma | Plastics, rubber, monomer |
| p-Chloro-o-toluidine (95-69-2) and its strong acid salts | Bladder | Dye/pigment manufacture, textiles |
| Creosotes (8001-58-9) | Skin | Wood preservation |
| Diethyl sulphate (64-67-5) | – | Chemical intermediate |
| Dimethylcarbamoyl chloride (79-44-7) | – | Chemical intermediate |
| Dimethyl sulphate (77-78-1) | – | Chemical intermediate |
| Epichlorohydrin (106-89-8) | – | Plastics/resins monomer |
| Ethylene dibromide (106-93-4) | – | Chemical intermediate, fumigant, fuels |
| Formaldehyde (50-0-0) | Nasopharynx | Plastics, textiles, laboratory agent |
| 4,4´-Methylene- bis-2-chloroaniline (MOCA) (101-14-4) |
Bladder | Rubber manufacture |
| Polychlorinated biphenyls (1336-36-3) | Liver, bile ducts, leukaemia, lymphoma | Electrical components |
| Silica (14808-60-7), crystalline | Lung | Stone cutting, mining, glass, paper |
| Styrene oxide (96-09-3) | – | Plastics, chemical intermediate |
| Tetrachloroethylene (127-18-4) |
Oesophagus, lymphoma | Solvent, dry cleaning |
| Trichloroethylene (79-01-6) | Liver, lymphoma | Solvent, dry cleaning, metal |
| Tris(2,3-dibromopropylphosphate (126-72-7) |
– | Plastics, textiles, flame retardant |
| Vinyl bromide (593-60-2) | – | Plastics, textiles, monomer |
| Vinyl fluoride (75-02-5) | – | Chemical intermediate |
1 Evaluated in the IARC Monographs, Volumes 1-63 (1972-1995) (excluding pesticides and drugs).
2 CAS Registry Nos. appear between parentheses.
Table 5. Chemicals, groups of chemicals or mixtures for which exposures are mostly occupational (excluding pesticides and drugs).
Group 2B—Possibly carcinogenic to humans1
| Exposure2 | Main industry/use |
| Acetaldehyde (75-07-0) | Plastics manufacture, flavors |
| Acetamide (60-35-5) | Solvent, chemical intermediate |
| Acrylamide (79-06-1) | Plastics, grouting agent |
| p-Aminoazotoluene (60-09-3) | Dye/pigment manufacture |
| o-Aminoazotoluene (97-56-3) | Dyes/pigments, textiles |
| o-Anisidine (90-04-0) | Dye/pigment manufacture |
| Antimony trioxide (1309-64-4) | Flame retardant, glass, pigments |
| Auramine (492-80-8) (technical-grade) | Dyes/pigments |
| Benzyl violet 4B (1694-09-3) | Dyes/pigments |
| Bitumens (8052-42-4), extracts of steam-refined and air-refined |
Building material |
| Bromodichloromethane (75-27-4) | Chemical intermediate |
| b-Butyrolactone (3068-88-0) | Chemical intermediate |
| Carbon-black extracts | Printing inks |
| Carbon tetrachloride (56-23-5) | Solvent |
| Ceramic fibers | Plastics, textiles, aerospace |
| Chlorendic acid (115-28-6) | Flame retardant |
| Chlorinated paraffins of average carbon chain length C12 and average degree of chlorination approximately 60% | Flame retardant |
| a-Chlorinated toluenes | Dye/pigment manufacture, chemical intermediate |
| p-Chloroaniline (106-47-8) | Dye/pigment manufacture |
| Chloroform (67-66-3) | Solvent |
| 4-Chloro-o-phenylenediamine (95-83-9) | Dyes/pigments, hair dyes |
| CI Acid Red 114 (6459-94-5) | Dyes/pigments, textiles, leather |
| CI Basic Red 9 (569-61-9) | Dyes/pigments, inks |
| CI Direct Blue 15 (2429-74-5) | Dyes/pigments, textiles, paper |
| Cobalt (7440-48-4)and cobalt compounds | Glass, paints, alloys |
| p-Cresidine (120-71-8) | Dye/pigment manufacture |
| N,N´-Diacetylbenzidine (613-35-4) | Dye/pigment manufacture |
| 2,4-Diaminoanisole (615-05-4) | Dye/pigment manufacture, hair dyes |
| 4,4´-Diaminodiphenyl ether (101-80-4) | Plastics manufacture |
| 2,4-Diaminotoluene (95-80-7) | Dye/pigment manufacture, hair dyes |
| p-Dichlorobenzene (106-46-7) | Chemical intermediate |
| 3,3´-Dichlorobenzidine (91-94-1) | Dye/pigment manufacture |
| 3,3´-Dichloro-4,4´-diaminodiphenyl ether (28434-86-8) | Not used |
| 1,2-Dichloroethane (107-06-2) | Solvent, fuels |
| Dichloromethane (75-09-2) | Solvent |
| Diepoxybutane (1464-53-5) | Plastics/resins |
| Diesel fuel, marine | Fuel |
| Di(2-ethylhexyl)phthalate (117-81-7) | Plastics, textiles |
| 1,2-Diethylhydrazine (1615-80-1) | Laboratory reagent |
| Diglycidyl resorcinol ether (101-90-6) | Plastics/resins |
| Diisopropyl sulphate (29973-10-6) | Contaminant |
| 3,3´-Dimethoxybenzidine (o-Dianisidine) (119-90-4) |
Dye/pigment manufacture |
| p-Dimethylaminoazobenzene (60-11-7) | Dyes/pigments |
| 2,6-Dimethylaniline (2,6-Xylidine)(87-62-7) | Chemical intermediate |
| 3,3´-Dimethylbenzidine (o-Tolidine)(119-93-7) | Dye/pigment manufacture |
| Dimethylformamide (68-12-2) | Solvent |
| 1,1-Dimethylhydrazine (57-14-7) | Rocket fuel |
| 1,2-Dimethylhydrazine (540-73-8) | Research chemical |
| 1,4-Dioxane (123-91-1) | Solvent |
| Disperse Blue 1 (2475-45-8) | Dyes/pigments, hair dyes |
| Ethyl acrylate (140-88-5) | Plastics, adhesives, monomer |
| Ethylene thiourea (96-45-7) | Rubber chemical |
| Fuel oils, residual (heavy) | Fuel |
| Furan (110-00-9) | Chemical intermediate |
| Gasoline | Fuel |
| Glasswool | Insulation |
| Glycidaldehyde (765-34-4) | Textile, leather manufacture |
| HC Blue No. 1 (2784-94-3) | Hair dyes |
| Hexamethylphosphoramide (680-31-9) | Solvent, plastics |
| Hydrazine (302-01-2) | Rocket fuel, chemical intermediate |
| Lead (7439-92-1) and lead compounds, inorganic | Paints, fuels |
| 2-Methylaziridine(75-55-8) | Dyes, paper, plastics manufacture |
| 4,4’-Methylene-bis-2-methylaniline (838-88-0) | Dye/pigment manufacture |
| 4,4’-Methylenedianiline(101-77-9) | Plastics/resins, dye/pigment manufacture |
| Methylmercury compounds | Pesticide manufacture |
| 2-Methyl-1-nitroanthraquinone (129-15-7) (uncertain purity) | Dye/pigment manufacture |
| Nickel, metallic (7440-02-0) | Catalyst |
| Nitrilotriacetic acid (139-13-9) and its salts | Chelating agent, detergent |
| 5-Nitroacenaphthene (602-87-9) | Dye/pigment manufacture |
| 2-Nitropropane (79-46-9) | Solvent |
| N-Nitrosodiethanolamine (1116-54-7) | Cutting fluids, impurity |
| Oil Orange SS (2646-17-5) | Dyes/pigments |
| Phenyl glycidyl ether (122-60-1) | Plastics/adhesives/resins |
| Polybrominated biphenyls (Firemaster BP-6) (59536-65-1) | Flame retardant |
| Ponceau MX (3761-53-3) | Dyes/pigments, textiles |
| Ponceau 3R (3564-09-8) | Dyes/pigments, textiles |
| 1,3-Propane sulphone (1120-71-4) | Dye/pigment manufacture |
| b-Propiolactone (57-57-8) | Chemical intermediate; plastics manufacture |
| Propylene oxide (75-56-9) | Chemical intermediate |
| Rockwool | Insulation |
| Slagwool | Insulation |
| Styrene (100-42-5) | Plastics |
| 2,3,7,8-Tetrachlorodibenzo-p-dioxin (TCDD) (1746-01-6) | Contaminant |
| Thioacetamide (62-55-5) | Textile, paper, leather, rubber manufacture |
| 4,4’-Thiodianiline (139-65-1) | Dye/pigment manufacture |
| Thiourea (62-56-6) | Textile, rubber ingredient |
| Toluene diisocyanates (26471-62-5) | Plastics |
| o-Toluidine (95-53-4) | Dye/pigment manufacture |
| Trypan blue (72-57-1) | Dyes/pigments |
| Vinyl acetate (108-05-4) | Chemical intermediate |
| Welding fumes | Metallurgy |
1 Evaluated in the IARC Monographs, Volumes 1-63 (1972-1995) (excluding pesticides and drugs).
2 CAS Registry Nos. appear between parentheses.
Occupational exposures may also occur during the production and use of some pesticides and drugs. Table 6 presents an evaluation of the carcinogenicity of pesticides; two of them, captafol and ethylene dibromide, are classified as probable human carcinogens, while a total of 20 others, including DDT, atrazine and chlorophenols, are classified as possible human carcinogens.
Table 6. Pesticides evaluated in IARC Monographs, Volumes 1-63(1972-1995)
| IARC Group | Pesticide1 |
| 2A—Probably carcinogenic to humans | Captafol (2425-06-1) Ethylene dibromide (106-93-4) |
| 2B—Possibly carcinogenic to humans | Amitrole (61-82-5) Atrazine (1912-24-9) Chlordane (57-74-9) Chlordecone (Kepone) (143-50-0) Chlorophenols Chlorophenoxy herbicides DDT (50-29-3) 1,2-Dibromo-3-chloropropane (96-12-8) 1,3-Dichloropropene (542-75-6) (technical-grade) Dichlorvos (62-73-7) Heptachlor (76-44-8) Hexachlorobenzene (118-74-1) Hexachlorocyclohexanes (HCH) Mirex (2385-85-5) Nitrofen (1836-75-5), technical-grade Pentachlorophenol (87-86-5) Sodium o-phenylphenate (132-27-4) Sulphallate (95-06-7) Toxaphene (Polychlorinated camphenes) (8001-35-2) |
1 CAS Registry Nos. appear between parentheses.
Several drugs are human carcinogens (table 9): they are mainly alkylating agents and hormones; 12 more drugs, including chloramphenicol, cisplatine and phenacetin, are classified as probable human carcinogens (Group 2A). Occupational exposure to these known or suspected carcinogens, used mainly in chemotherapy, can occur in pharmacies and during their administration by nursing staff.
Table 7. Drugs evaluated in IARC Monographs, Volumes 1-63 (1972-1995).
| Drug1 | Target organ2 |
| IARC GROUP 1—Carcinogenic to humans | |
| Analgesic mixtures containing phenacetin | Kidney, bladder |
| Azathioprine (446-86-6) | Lymphoma, hepatobiliary system, skin |
| N,N-Bis(2-chloroethyl)- b-naphthylamine (Chlornaphazine) (494-03-1) | Bladder |
| 1,4-Butanediol dimethanesulphonate (Myleran) (55-98-1) |
Leukaemia |
| Chlorambucil (305-03-3) | Leukaemia |
| 1-(2-Chloroethyl)-3-(4-methylcyclohexyl)-1-nitrosourea (Methyl-CCNU) (13909-09-6) | Leukaemia |
| Cyclosporin (79217-60-0) | Lymphoma, skin |
| Cyclophosphamide (50-18-0) (6055-19-2) | Leukaemia, bladder |
| Diethylstilboestrol (56-53-1) | Cervix, vagina, breast |
| Melphalan (148-82-3) | Leukaemia |
| 8-Methoxypsoralen (Methoxsalen) (298-81-7) plus ultraviolet A radiation | Skin |
| MOPP and other combined chemotherapy including alkylating agents | Leukaemia |
| Oestrogen replacement therapy | Uterus |
| Oestrogens, nonsteroidal | Cervix, vagina, breast |
| Oestrogens, steroidal | Uterus |
| Oral contraceptives, combined | Liver |
| Oral contraceptives, sequential | Uterus |
| Thiotepa (52-24-4) | Leukaemia |
| Treosulfan (299-75-2) | Leukaemia |
| IARC GROUP 2A—Probably carcinogenic to humans | |
| Adriamycin (23214-92-8) | – |
| Androgenic (anabolic) steroids | (Liver) |
| Azacitidine (320-67-2) | – |
| Bischloroethyl nitrosourea (BCNU) (154-93-8) | (Leukaemia) |
| Chloramphenicol (56-75-7) | (Leukaemia) |
| 1-(2-Chloroethyl)-3-cyclohexyl-1-nitrosourea (CCNU) (13010-47-4) | – |
| Chlorozotocine (54749-90-5) | – |
| Cisplatin (15663-27-1) | – |
| 5-Methoxypsoralen (484-20-8) | – |
| Nitrogen mustard (51-75-2) | (Skin) |
| Phenacetin (62-44-2) | (Kidney, bladder) |
| Procarbazine hydrochloride (366-70-1) | – |
1 CAS Registry Nos. appear between parentheses.
2 Suspected target organs are given in parentheses.
Several environmental agents are known or suspected causes of cancer in humans and are listed in table 8; although exposure to such agents is not primarily occupational, there are groups of individuals exposed to them because of their work: examples are uranium miners exposed to radon decay products, hospital workers exposed to hepatitis B virus, food processors exposed to aflatoxins from contaminated foods, outdoor workers exposed to ultraviolet radiation or diesel engine exhaust, and bar staff or waiters exposed to environmental tobacco smoke.
The IARC Monograph programme has covered most of the known or suspected causes of cancer; there are, however, some important groups of agents that have not been evaluated by IARC—namely, ionizing radiation and electrical and magnetic fields.
Table 8. Environmental agents/exposures known or suspected to cause cancer in humans.1
| Agent/exposure | Target organ2 | Strength of evidence3 |
| Air pollutants | ||
| Erionite | Lung, pleura | 1 |
| Asbestos | Lung, pleura | 1 |
| Polycyclic aromatic hydrocarbons4 | (Lung, bladder) | S |
| Water pollutants | ||
| Arsenic | Skin | 1 |
| Chlorination by-products | (Bladder) | S |
| Nitrate and nitrite | (Oesophagus, stomach) | S |
| Radiation | ||
| Radon and its decay products | Lung | 1 |
| Radium, thorium | Bone | E |
| Other X-irradiation | Leukaemia, breast, thyroid, others | E |
| Solar radiation | Skin | 1 |
| Ultraviolet radiation A | (Skin) | 2A |
| Ultraviolet radiation B | (Skin) | 2A |
| Ultraviolet radiation C | (Skin) | 2A |
| Use of sunlamps and sunbeds | (Skin) | 2A |
| Electric and magnetic fields | (Leukaemia) | S |
| Biological agents | ||
| Chronic infection with hepatitis B virus | Liver | 1 |
| Chronic infection with hepatitis C virus | Liver | 1 |
| Infection with Helicobacter pylori | Stomach | 1 |
| Infection with Opistorchis viverrini | Bile ducts | 1 |
| Infection with Chlonorchis sinensis | (Liver) | 2A |
| Human Papilloma virus types 16 and18 | Cervix | 1 |
| Human Papilloma virus types 31 and 33 | (Cervix) | 2A |
| Human Papilloma virus types other than 16, 18, 31 and 33 | (Cervix) | 2B |
| Infection with Schistosoma haematobium | Bladder | 1 |
| Infection with Schistosoma japonicum | (Liver, colon) | 2B |
| Tobacco, alcohol and related substances | ||
| Alcoholic beverages | Mouth, pharynx, oesophagus, liver, larynx | 1 |
| Tobacco smoke | Lip, mouth, pharynx, oesophagus, pancreas, larynx, lung, kidney, bladder, (others) | 1 |
| Smokeless tobacco products | Mouth | 1 |
| Betel quid with tobacco | Mouth | 1 |
| Dietary factors | ||
| Aflatoxins | Liver | 1 |
| Aflatoxin M1 | (Liver) | 2B |
| Ochratoxin A | (Kidney) | 2B |
| Toxins derived from Fusarium moniliforme | (Oesophagus) | 2B |
| Chinese style salted fish | Nasopharynx | 1 |
| Pickled vegetables (traditional in Asia) | (Oesophagus, stomach) | 2B |
| Bracken fern | (Oesophagus) | 2B |
| Safrole | – | 2B |
| Coffee | (Bladder) | 2B |
| Caffeic acid | – | 2B |
| Hot mate | (Oesophagus) | 2A |
| Fresh fruits and vegetables (protective) | Mouth, oesophagus, stomach, colon, rectum, larynx, lung (others) | E |
| Fat | (Colon, breast, endometrium) | S |
| Fiber (protective) | (Colon, rectum) | S |
| Nitrate and nitrite | (Oesophagus, stomach) | S |
| Salt | (Stomach) | S |
| Vitamin A, b-carotene (protective) | (Mouth, oesophagus, lung, others) | S |
| Vitamin C (protective) | (Oesophagus, stomach) | S |
| IQ | (Stomach, colon, rectum) | 2A |
| MeIQ | – | 2B |
| MeIQx | – | 2B |
| PhIP | – | 2B |
| Reproductive and sexual behavior | ||
| Late age at first pregnancy | Breast | E |
| Low parity | Breast, ovary, corpus uteri | E |
| Early age at first intercourse | Cervix | E |
| Number of sexual partners | Cervix | E |
1 Agents and exposures, as well as medicines, occurring mainly in the occupational setting are excluded.
2 Suspected target organs are given in parentheses.
3 IARC Monograph evaluation reported wherever available (1: human carcinogen; 2A: probable human carcinogen; 2B: possible human carcinogen); otherwise E: established carcinogen; S: suspected carcinogen.
4 Human exposure to polycyclic aromatic hydrocarbons occurs in mixtures, such as engine emissions, combustion fumes and soots. Several mixtures and individual hydrocarbons have been evaluated by IARC.
Industries and Occupations
Current understanding of the relationship between occupational exposures and cancer is far from complete; in fact, only 22 individual agents are established occupational carcinogens (table 9), and for many more experimental carcinogens no definitive evidence is available based on exposed workers. In many cases, there is considerable evidence of increased risks associated with particular industries and occupations, although no specific agents can be identified as aetiological factors. Table 10 present lists of industries and occupations associated with excess carcinogenic risks, together with the relevant cancer sites and the known (or suspected) causative agent(s).
Table 9. Industries, occupations and exposures recognized as presenting a carcinogenic risk.
| Industry (ISIC code) | Occupation/process | Cancer site/type | Known or suspected causative agent |
| Agriculture, forestry and fishing (1) | Vineyard workers using arsenic insecticides Fishermen | Lung, skin Skin, lip | Arsenic compounds Ultraviolet radiation |
| Mining and quarrying (2) | Arsenic mining Iron ore (haematite) mining Asbestos mining Uranium mining Talc mining and milling | Lung, skin Lung Lung, pleural and peritoneal mesothelioma Lung Lung | Arsenic compounds Radon decay products Asbestos Radon decay products Talc containing asbestiform fibers |
| Chemical (35) | Bis(chloromethyl) ether (BCME) and chloromethyl-methyl ether (CMME) production workers and users Vinyl chloride production Isopropyl alcohol manufacture (strong-acid process) Pigment chromate production Dye manufacturers and users Auramine manufacture p-chloro-o-toluidine production | Lung (oat-cell carcinoma) Liver angiosarcoma Sinonasal Lung, sinonasal Bladder Bladder Bladder | BCME, CMME Vinyl chloride monomer Not identified Chromium (VI) compounds Benzidine, 2-naphthylamine, 4-aminobiphenyl Auramine and other aromatic amines used in the process p-chloro-o-toluidine and its strong acid salts |
| Leather (324) | Boot and shoe manufacture | Sinonasal, leukaemia | Leather dust, benzene |
| Wood and wood products (33) | Furniture and cabinet makers | Sinonasal | Wood dust |
| Pesticides and herbicides production (3512) | Arsenical insecticides production and packaging | Lung | Arsenic compounds |
| Rubber industry (355) | Rubber manufacture Calendering, tyre curing, tyre building Millers, mixers Synthetic latex production, tyre curing, calender operatives, reclaim, cable makers Rubber film production | Leukaemia Bladder Leukaemia Bladder Bladder Leukaemia | Benzene Aromatic amines Benzene Aromatic amines Aromatic amines Benzene |
| Asbestos production (3699) | Insulated material production (pipes, sheeting, textile, clothes, masks, asbestos cement products) | Lung, pleural and peritoneal mesothelioma | Asbestos |
| Metals (37) | Aluminum production Copper smelting Chromate production, chromium plating Iron and steel founding Nickel refining Pickling operations Cadmium production and refining; nickel-cadmium battery manufacture; cadmium pigment manufacture; cadmium alloy production; electroplating; zinc smelters; brazing and polyvinyl chloride compounding Beryllium refining and machining; production of beryllium-containing products | Lung, bladder Lung Lung, sinonasal Lung Sinonasal, lung Larynx, lung Lung Lung | Polycyclic aromatic hydrocarbons, tar Arsenic compounds Chromium (VI) compounds Not identified Nickel compounds Inorganic acid mists containing sulphuric acid Cadmium and cadmium compounds Beryllium and beryllium compounds |
| Shipbuilding, motor vehicle and railroad equipment manufacture (385) | Shipyard and dockyard, motor vehicle and railroad manufacture workers | Lung, pleural and peritoneal mesothelioma | Asbestos |
| Gas (4) | Coke plant workers Gas workers Gas-retort house workers | Lung Lung, bladder, scrotum Bladder | Benzo(a)pyrene Coal carbonization products, 2-naphthylamine Aromatic amines |
| Construction (5) | Insulators and pipe coverers Roofers, asphalt workers | Lung, pleural and peritoneal mesothelioma Lung | Asbestos Polycyclic aromatic hydrocarbons |
| Other | Medical personnel (9331) Painters (construction, automotive industry and other users) | Skin, leukaemia Lung | Ionizing radiation Not identified |
Table 10. Industries, occupations and exposures reported to present a cancer excess but for which the assessment of the carcinogenic risk is not definitive.
| Industry (ISIC code) | Occupation/process | Cancer site/type | Known (or suspected) causative agent |
| Agriculture, forestry and fishing (1) | Farmers, farm workers Herbicide application Insecticide application | Lymphatic and haematopoietic system (leukaemia, lymphoma) Malignant lymphomas, soft-tissue sarcomas Lung, lymphoma | Not identified Chlorophenoxy herbicides, chlorophenols (presumably contaminated with polychlorinated dibenzodioxins) Non-arsenical insecticides |
| Mining and quarrying (2) | Zinc-lead mining Coal Metal mining Asbestos mining | Lung Stomach Lung Gastrointestinal tract | Radon decay products Coal dust Crystalline silica Asbestos |
| Food industry (3111) | Butchers and meat workers | Lung | Viruses, PAH1 |
| Beverage industry (3131) | Beer brewers | Upper aero-digestive tract | Alcohol consumption |
| Textile manufacture (321) | Dyers Weavers | Bladder Bladder, sinonasal, mouth | Dyes Dusts from fibers and yarns |
| Leather (323) | Tanners and processors Boot and shoe manufacture and repair | Bladder, pancreas, lung Sinonasal, stomach, bladder | Leather dust, other chemicals, chromium Not identified |
| Wood and wood products (33), pulp and paper industry (341) | Lumbermen and sawmill workers Pulp and papermill workers Carpenters, joiners Woodworkers, unspecified Plywood production, particle-board production | Nasal cavity, Hodgkin lymphoma, skin Lymphopoietic tissue, lung Nasal cavity, Hodgkin lymphoma Lymphomas Nasopharynx, sinonasal | Wood dust, chlorophenols, creosotes Not identified Wood dust, solvents Not identified Formaldehyde |
| Printing (342) | Rotogravure workers, binders, printing pressmen, machine-room workers and other jobs | Lymphocytic and haemopoietic system, oral, lung, kidney | Oil mist, solvents |
| Chemical (35) | 1,3-Butadiene production Acrylonitrile production Vinylidene chloride production Isopropyl alcohol manufacture (strong-acid process) Polychloroprene production Dimethylsulphate production Epichlorohydrin production Ethylene oxide production Ethylene dibromide production Formaldehyde production Flame retardant and plasticizer use Benzoyl chloride production | Lymphocytic and haemopoietic system Lung, colon Lung Larynx Lung Lung Lung, lymphatic and haemopoietic system (leukaemia) Lymphatic and haemopoietic system (leukaemia), stomach Digestive system Nasopharynx, sinonasal Skin (melanoma) Lung | 1,3-Butadiene Acrylonitrile Vinylidene chloride (mixed exposure with acrylonitrile) Not identified Chloroprene Dimethylsulphate Epichlorohydrin Ethylene oxide Ethylene dibromide Formaldehyde Polychlorinated biphenyls Benzoyl chloride |
| Herbicides production (3512) | Chlorophenoxy herbicide production | Soft-tissue sarcoma | Chlorophenoxy herbicides, chlorophenols (contaminated with polychlorinated dibenzodioxins) |
| Petroleum (353) | Petroleum refining | Skin, leukaemia, brain | Benzene, PAH, untreated and mildly treated mineral oils |
| Rubber (355) | Various occupations in rubber manufacture Styrene-butadiene rubber production | Lymphoma, multiple myeloma, stomach, brain, lung Lymphatic and haematopoietic system | Benzene, MOCA,2 other not identified 1,3-Butadiene |
| Ceramic, glass and refractory brick (36) | Ceramic and pottery workers Glass workers (art glass, container and pressed ware) | Lung Lung | Crystalline silica Arsenic and other metal oxides, silica, PAH |
| Asbestos production (3699) | Insulation material production (pipes, sheeting, textiles, clothes, masks, asbestos cement products) | Larynx, gastrointestinal tract | Asbestos |
| Metals (37, 38) | Lead smelting Cadmium production and refining; nickel-cadmium battery manufacture; cadmium pigment manufacture; cadmium alloy production; electroplating; zinc smelting; brazing and polyvinyl chloride compounding Iron and steel founding | Respiratory and digestive systems Prostate Lung | Lead compounds Cadmium and cadmium compounds Crystalline silica |
| Shipbuilding (384) | Shipyard and dockyard workers | Larynx, digestive system | Asbestos |
| Motor vehicle manufacturing (3843, 9513) | Mechanics, welders, etc. | Lung | PAH, welding fumes, engine exhaust |
| Electricity (4101, 9512) | Generation, production, distribution, repair | Leukaemia, brain tumors Liver, bile ducts | Extremely low frequency magnetic fields PCBs3 |
| Construction (5) | Insulators and pipe coverers Roofers, asphalt workers | Larynx, gastrointestinal tract Mouth, pharynx, larynx, oesophagus, stomach | Asbestos PAH, coal tar, pitch |
| Transport (7) | Railroad workers, filling station attendants, bus and truck drivers, operators of excavating machines | Lung, bladder Leukaemia | Diesel engine exhaust Extremely low frequency magnetic fields |
| Other | Service station attendants (6200) Chemists and other laboratory workers (9331) Embalmers, medical personnel (9331) Health workers (9331) Laundry and dry cleaners (9520) Hairdressers (9591) Radium dial workers | Leukaemia and lymphoma Leukaemia and lymphoma, pancreas Sinonasal, nasopharynx Liver Lung, oesophagus, bladder Bladder, leukaemia and lymphoma Breast | Benzene Not identified (viruses, chemicals) Formaldehyde Hepatitis B virus Tri- and tetrachloroethylene and carbon tetrachloride Hair dyes, aromatic amines Radon |
1 PAH, polycyclic aromatic hydrocarbon.
2 MOCA, 4,4’-methylene-bis-2-chloroaniline.
3 PCBs, polychlorinated biphenyls.
Table 9 presents industries, occupations and exposures in which the presence of a carcinogenic risk is considered to be established, whereas Table 10 shows industrial processes, occupations and exposures for which an excess cancer risk has been reported but evidence is not considered to be definitive. Also included in table 10 are some occupations and industries already listed in table 9, for which there is inconclusive evidence of association with cancers other than those mentioned in table 9. For example, the asbestos production industry is included in table 9 in relation to lung cancer and pleural and peritoneal mesothelioma, whereas the same industry is included in table 10 in relation to gastrointestinal neoplasms. A number of industries and occupations listed intables 9 and 10 have also been evaluated under the IARC Monographs programme. For example, “occupational exposure to strong inorganic acid mist containing sulphuric acid” was classified in Group 1 (carcinogenic to humans).
Constructing and interpreting such lists of chemical or physical carcinogenic agents and associating them with specific occupations and industries is complicated by a number of factors: (1) information on industrial processes and exposures is frequently poor, not allowing a complete evaluation of the importance of specific carcinogenic exposures in different occupations or industries; (2) exposures to well-known carcinogenic exposures, such as vinyl chloride and benzene, occur at different intensities in different occupational situations; (3) changes in exposure occur over time in a given occupational situation, either because identified carcinogenic agents are substituted by other agents or (more frequently) because new industrial processes or materials are introduced; (4) any list of occupational exposures can refer only to the relatively small number of chemical exposures which have been investigated with respect to the presence of a carcinogenic risk.
All of the above issues emphasize the most critical limitation of a classification of this type, and in particular its generalization to all areas of the world: the presence of a carcinogen in an occupational situation does not necessarily mean that workers are exposed to it and, in contrast, the absence of identified carcinogens does not exclude the presence of yet unidentified causes of cancer.
A particular problem in developing countries is that much of the industrial activity is fragmented and takes place in local settings. These small industries are often characterized by old machinery, unsafe buildings, employees with limited training and education, and employers with limited financial resources. Protective clothing, respirators, gloves and other safety equipment are seldom available or used. The small companies tend to be geographically scattered and inaccessible to inspections by health and safety enforcement agencies.
" DISCLAIMER: The ILO does not take responsibility for content presented on this web portal that is presented in any language other than English, which is the language used for the initial production and peer-review of original content. Certain statistics have not been updated since the production of the 4th edition of the Encyclopaedia (1998)."