Children categories

94. Education and Training Services (7)

94. Education and Training Services
Chapter Editor: Michael McCann
Table of Contents
Tables and Figures
Tables
Click a link below to view table in article context.
1. Diseases affecting day-care workers & teachers
2. Hazards & precautions for particular classes
3. Summary of hazards in colleges & universities
Figures
Point to a thumbnail to see figure caption, click to see figure in article context.

95. Emergency and Security Services (9)

95. Emergency and Security Services
Chapter Editor: Tee L. Guidotti
Table of Contents
Tables and Figures
Tables
Click a link below to view table in article context.
1. Recommendations & criteria for compensation
Figures
Point to a thumbnail to see figure caption, click to see figure in article context.

96. Entertainment and the Arts (31)

96. Entertainment and the Arts
Chapter Editor: Michael McCann
Table of Contents
Tables and Figures
Arts and Crafts
Performing and Media Arts
Entertainment
Tables
Click a link below to view table in article context.
1. Precautions associated with hazards
2. Hazards of art techniques
3. Hazards of common stones
4. Main risks associated with sculpture material
5. Description of fibre & textile crafts
6. Description of fibre & textile processes
7. Ingredients of ceramic bodies & glazes
8. Hazards & precautions of collection management
9. Hazards of collection objects
Figures
Point to a thumbnail to see figure caption, click to see the figure in the article context.

97. Health Care Facilities and Services (25)

97. Health Care Facilities and Services
Chapter Editor: Annelee Yassi
Table of Contents
Tables and Figures
Health Care: Its Nature and Its Occupational Health Problems
Annalee Yassi and Leon J. Warshaw
Social Services
Susan Nobel
Home Care Workers: The New York City Experience
Lenora Colbert
Occupational Health and Safety Practice: The Russian Experience
Valery P. Kaptsov and Lyudmila P. Korotich
Ergonomics and Health Care
Hospital Ergonomics: A Review
Madeleine R. Estryn-Béhar
Strain in Health Care Work
Madeleine R. Estryn-Béhar
Case Study: Human Error and Critical Tasks: Approaches for Improved System Performance
Work Schedules and Night Work in Health Care
Madeleine R. Estryn-Béhar
The Physical Environment and Health Care
Exposure to Physical Agents
Robert M. Lewy
Ergonomics of the Physical Work Environment
Madeleine R. Estryn-Béhar
Prevention and Management of Back Pain in Nurses
Ulrich Stössel
Case Study: Treatment of Back Pain
Leon J. Warshaw
Health Care Workers and Infectious Disease
Overview of Infectious Diseases
Friedrich Hofmann
Prevention of Occupational Transmission of Bloodborne Pathogens
Linda S. Martin, Robert J. Mullan and David M. Bell
Tuberculosis Prevention, Control and Surveillance
Robert J. Mullan
Chemicals in the Health Care Environment
Overview of Chemical Hazards in Health Care
Jeanne Mager Stellman
Managing Chemical Hazards in Hospitals
Annalee Yassi
Waste Anaesthetic Gases
Xavier Guardino Solá
Health Care Workers and Latex Allergy
Leon J. Warshaw
The Hospital Environment
Buildings for Health Care Facilities
Cesare Catananti, Gianfranco Damiani and Giovanni Capelli
Hospitals: Environmental and Public Health Issues
M.P. Arias
Hospital Waste Management
M.P. Arias
Managing Hazardous Waste Disposal Under ISO 14000
Jerry Spiegel and John Reimer
Tables
Click a link below to view table in article context.
1. Examples of health care functions
2. 1995 integrated sound levels
3. Ergonomic noise reduction options
4. Total number of injuries (one hospital)
5. Distribution of nurses’ time
6. Number of separate nursing tasks
7. Distribution of nurses' time
8. Cognitive & affective strain & burn-out
9. Prevalence of work complaints by shift
10. Congenital abnormalities following rubella
11. Indications for vaccinations
12. Post-exposure prophylaxis
13. US Public Health Service recommendations
14. Chemicals’ categories used in health care
15. Chemicals cited HSDB
16. Properties of inhaled anaesthetics
17. Choice of materials: criteria & variables
18. Ventilation requirements
19. Infectious diseases & Group III wastes
20. HSC EMS documentation hierarchy
21. Role & responsibilities
22. Process inputs
23. List of activities
Figures
Point to a thumbnail to see figure caption, click to see the figure in the article context.

98. Hotels and Restaurants (4)

98. Hotels and Restaurants
Chapter Editor: Pam Tau Lee
Table of Contents

99. Office and Retail Trades (7)
99. Office and Retail Trades
Chapter Editor: Jonathan Rosen
Table of Contents
Tables and Figures
The Nature of Office and Clerical Work
Charles Levenstein, Beth Rosenberg and Ninica Howard
Professionals and Managers
Nona McQuay
Offices: A Hazard Summary
Wendy Hord
Bank Teller Safety: The Situation in Germany
Manfred Fischer
Telework
Jamie Tessler
The Retail Industry
Adrienne Markowitz
Case Study: Outdoor Markets
John G. Rodwan, Jr.
Tables
Click a link below to view table in article context.
1. Standard professional jobs
2. Standard clerical jobs
3. Indoor air pollutants in office buildings
4. Labour statistics in the retail industry
Figures
Point to a thumbnail to see figure caption, click to see figure in article context.

100. Personal and Community Services (6)
100. Personal and Community Services
Chapter Editor: Angela Babin
Table of Contents
Tables and Figures
Indoor Cleaning Services
Karen Messing
Barbering and Cosmetology
Laura Stock and James Cone
Laundries, Garment and Dry Cleaning
Gary S. Earnest, Lynda M. Ewers and Avima M. Ruder
Funeral Services
Mary O. Brophy and Jonathan T. Haney
Domestic Workers
Angela Babin
Case Study: Environmental Issues
Michael McCann
Click a link below to view table in article context.
1. Postures observed during dusting in a hospital
2. Dangerous chemicals used in cleaning
Figures
Point to a thumbnail to see figure caption, click to see figure in article context.

101. Public and Government Services (12)

101. Public and Government Services
Chapter Editor: David LeGrande
Table of Contents
Tables and Figurs
Occupational Health and Safety Hazards in Public and Governmental Services
David LeGrande
Case Report: Violence and Urban Park Rangers in Ireland
Daniel Murphy
Inspection Services
Jonathan Rosen
Postal Services
Roxanne Cabral
Telecommunications
David LeGrande
Hazards in Sewage (Waste) Treatment Plants
Mary O. Brophy
Domestic Waste Collection
Madeleine Bourdouxhe
Street Cleaning
J.C. Gunther, Jr.
Sewage Treatment
M. Agamennone
Municipal Recycling Industry
David E. Malter
Waste Disposal Operations
James W. Platner
The Generation and Transport of Hazardous Wastes: Social and Ethical Issues
Colin L. Soskolne
Tables
Click a link below to view table in article context.
1. Hazards of inspection services
2. Hazardous objects found in domestic waste
3. Accidents in domestic waste collection (Canada)
4. Injuries in the recycling industry
Figures
Point to a thumbnail to see figure caption, click to see figure in article context.

102. Transport Industry and Warehousing (18)

102. Transport Industry and Warehousing
Chapter Editor: LaMont Byrd
Table of Contents
Tables and Figures
General Profile
LaMont Byrd
Case Study: Challenges to Workers’ Health and Safety in the Transportation and Warehousing Industry
Leon J. Warshaw
Air Transport
Airport and Flight Control Operations
Christine Proctor, Edward A. Olmsted and E. Evrard
Case Studies of Air Traffic Controllers in the United States and Italy
Paul A. Landsbergis
Aircraft Maintenance Operations
Buck Cameron
Aircraft Flight Operations
Nancy Garcia and H. Gartmann
Aerospace Medicine: Effects of Gravity, Acceleration and Microgravity in the Aerospace Environment
Relford Patterson and Russell B. Rayman
Helicopters
David L. Huntzinger
Road Transport
Truck and Bus Driving
Bruce A. Millies
Ergonomics of Bus Driving
Alfons Grösbrink and Andreas Mahr
Motor Vehicle Fuelling and Servicing Operations
Richard S. Kraus
Case Study: Violence in Gasoline Stations
Leon J. Warshaw
Rail Transport
Rail Operations
Neil McManus
Case Study: Subways
George J. McDonald
Water Transport
Water Transportation and the Maritime Industries
Timothy J. Ungs and Michael Adess
Storage
Storage and Transportation of Crude Oil, Natural Gas, Liquid Petroleum Products and Other Chemicals
Richard S. Kraus
Warehousing
John Lund
Case Study: US NIOSH Studies of Injuries among Grocery Order Selectors
Tables
Click a link below to view table in article context.
1. Bus driver seat measurements
2. Illumination levels for service stations
3. Hazardous conditions & administration
4. Hazardous conditions & maintenance
5. Hazardous conditions & right of way
6. Hazard control in the Railway industry
7. Merchant vessel types
8. Health hazards common across vessel types
9. Notable hazards for specific vessel types
10. Vessel hazard control & risk-reduction
11. Typical approximate combustion properties
12. Comparison of compressed & liquified gas
13. Hazards involving order selectors
14. Job safety analysis: Fork-lift operator
15. Job safety analysis: Order selector
Figures
Point to a thumbnail to see figure caption, click to see figure in article context.
Hospitals: Environmental and Public Health Issues
A hospital is not an isolated social environment; it has, given its mission, very serious intrinsic social responsibilities. A hospital needs to be integrated with its surroundings and should minimize its impact upon them, thus contributing to the welfare of the people who live near it.
From a regulatory perspective, the health industry has never been considered to be on the same level as other industries when they are ranked according to the health risks they pose. The result is that specific legislation in this sphere has been non-existent until recently, although in the last few years this deficiency has been addressed. While in many other kinds of industrial activities, health and safety is an integral part of the organization, most health centres still pay little or no attention to it.
One reason for this could be the attitudes of HCWs themselves, who may be preoccupied more with research and the acquisition of the latest technologies and diagnostic and treatment techniques than with looking into the effects that these advances could have on their own health and on the environment.
New developments in science and health care must be combined with environmental protection, because environmental policies in a hospital affect the quality of life of HCWs within the hospital and those who live outside it.
Integrated Health, Safety and Environmental Programmes
HCWs represent a major group, comparable in size to the large enterprises of the private sector. The number of people who pass through a hospital every day is very large: visitors, inpatients, outpatients, medical and commercial representatives, subcontractors and so on. All of them, to a greater or lesser degree, are exposed to the potential risks posed by the activities of the medical centre and, at the same time, contribute on a certain level to the improvement or the worsening of the safety and the care of the centre’s surroundings.
Strict measures are needed in order to safeguard HCWs, the general public and the surrounding environment from the deleterious effects that may stem from hospital activities. These activities include the use of ever more sophisticated technology, the more frequent use of extremely powerful drugs (the effects of which can have a profound and irreparable impact on the people who prepare or administer them), the too-often uncontrolled use of chemical products and the incidence of infectious diseases, some of which are incurable.
The risks of working in a hospital are many. Some are easy to identify, while others are very hard to detect; the measures to be taken should therefore always be rigorous.
Different groups of health professionals are particularly exposed to risks common to the health care industry in general, as well as to specific risks related to their profession and/or to the activities they perform in the course of their work.
The concept of prevention, therefore, must of necessity be incorporated to the health care field and encompass:
- safety in the broadest sense, including psychosociology and ergonomics as part of the programmes to improve the quality of life in the workplace
- hygiene, minimizing as much as possible any physical, chemical or biological factor that may affect the health of people in the work environment
- environment, following policies to protect nature and people in the surrounding community and decreasing the impact on the environment.
We should be aware that the environment is directly and intimately related to the safety and hygiene in the workplace, because natural resources are consumed at work, and because these resources are later reincorporated into our surroundings. Our quality of life will be good or bad depending on whether we make correct use of these resources and use appropriate technologies.
Everyone’s involvement is necessary in order to contribute to further:
- nature conservancy policies, designed to guarantee the survival of the natural heritage that surrounds us
- environmental improvement policies as well as policies to control indoor and environmental pollution in order to integrate human activity with the environment
- environmental research and training policies to improve working conditions as well as to reduce environmental impact
- planning organizational policies designed to set goals and develop norms and methodology for workers’ health and the environment.
Goals
Such a programme should endeavour to:
- change the culture and habits of health professionals in order to stimulate behaviour more conducive to safeguarding their health
- set goals and develop internal safety, hygiene and environmental guidelines through adequate planning and organization
- improve the methods of work to avoid a negative impact on health and the environment through environmental research and education
- increase the involvement of all personnel and have them take responsibility for health in the workplace
- create an adequate programme to establish and publicize the guidelines as well as to monitor their continued implementation
- correctly classify and manage the waste generated
- optimize costs, avoiding added expenditures that cannot be justified by the increased levels of safety and health or environmental quality.
Plan
A hospital should be conceived as a system that, through a number of processes, generates services. These services are the main goal of the activities performed in a hospital.
For the process to begin, certain commitments of energy, investments and technology are needed, which in turn will generate their own emissions and wastes. Their only aim is to provide service.
In addition to these prerequisites, consideration should be given to the conditions of the areas of the building where these activities will take place, since they have been designed a certain way and built with basic construction materials.
Control, planning and coordination are all necessary for an integrated safety, health and environmental project to succeed.
Methodology
Because of the complexity and the variety of risks in the health care field, multidisciplinary groups are required if solutions to each particular problem are to be found.
It is important for health care workers to be able to collaborate with safety studies, participating in the decisions that will be made to improve their working conditions. This way changes will be seen with a better attitude and the guidelines will be more readily accepted.
The safety, hygiene and environmental service should advise, stimulate and coordinate the programmes developed at the health centre. Responsibility for their implementation should fall upon whoever heads up the service where this programme will be followed. This is the only way to involve the entire organization.
In each particular case, the following will be selected:
- the system involved
- the parameters of the study
- the time needed to carry it out.
The study will consist of:
- an initial diagnosis
- analysis of the risk
- deciding on the course of action.
In order to implement the plan successfully it will always be necessary to:
- educate and inform people of the risks
- improve the management of human resources
- improve the channels of communication.
This type of study may be a global one encompassing the centre as a whole (e.g., internal plan for the disposal of hospital wastes) or partial, encompassing only one concrete area (e.g., where cancer chemotherapeutic drugs are prepared).
The study of these factors will give an idea of the degree to which safety measures are disregarded, as much from the legal as from the scientific point of view. The concept of “legal” here encompasses advances in science and technology as they occur, which requires the constant revision and modification of established norms and guidelines.
It would be convenient indeed if the regulations and the laws by which safety, hygiene and the environment are regulated were the same in all countries, something that would make the installation, management and use of technology or products from other countries much easier.
Results
The following examples show some of the measures that can be taken while following the aforementioned methodology.
Laboratories
An advisory service can be developed involving professionals of the various laboratories and coordinated by the safety and hygiene service of the medical centre. The main goal would be to improve the safety and health of the occupants of all the labs, involving and giving responsibility to the entire professional staff of each and trying at the same time to make sure that these activities do not have a negative impact on public health and the environment.
The measures taken should include:
- instituting the sharing of materials, products and equipment among the different laboratories, in order to optimize resources
- reducing the stocks of chemical products in laboratories
- creating a manual of basic norms of safety and hygiene
- planning courses to educate all laboratory workers on these matters
- training for emergencies.
Mercury
Thermometers, when broken, release mercury into the environment. A pilot project has been started with “unbreakable” thermometers to consider eventually substituting them for the glass thermometers. In some countries, such as the United States, electronic thermometers have replaced mercury thermometers to a very great extent.
Training the workers
The training and the commitment of the workers is the most important part of an integrated safety, health and environment programme. Given enough resources and time, the technicalities of almost any problem can be solved, but a complete solution will not be achieved without informing the workers of the risks and training them to avoid or control them. The training and education must be continuous, integrating health and safety techniques into all the other training programmes in the hospital.
Conclusions
The results that have been achieved so far in applying this work model allow us so far to be optimistic. They have shown that when people are informed about the whys and wherefores, their attitude toward change is very positive.
The response of health care personnel has been very good. They feel more motivated in their work and more valued when they have participated directly in the study and in the decision-making process. This participation, in turn, helps to educate the individual health care worker and to increase the degree of responsibility he or she is willing to accept.
The attainment of the goals of this project is a long-term objective, but the positive effects it generates more than compensate for the effort and the energy invested in it.
Restaurants
Restaurants can range in size from a small local diner to a large hotel restaurant, and generally consist of three main areas: the kitchen, where the preparation and cooking of meals takes place; the food service, which provides the service of food to guests in the restaurant; and the bar, a lounge which provides live or recorded entertainment and sales of alcoholic beverages and food.
Kitchens
Kitchen personnel include chefs and cooks, who are responsible for preparing and cooking food; pantry persons, who prepare the food for cooking and also keep an inventory of stock; and stewards, who are responsible for the cleaning and maintenance of the kitchen area.
Several different types of accidents can occur in the kitchen area, such as burns from deep fryers, slipping on grease and cuts from knives. Lack of maintenance or improper maintenance in the kitchen area can lead to accidents. Floors that have been mopped should always have a “Wet Floor” placard posted, or kitchen personnel may slip and injure themselves. Trays of food or dishes must be stored securely or they will topple over. Non-slip mats and non-slip floor waxes should be used at entrances and exits. Passageways should always be kept free of boxes, trash cans and other obstacles. Conditions that could cause an accident, such as loose floor tiles, exposed wiring, spills and so on, should always be reported and dealt with as soon as possible and a reporting mechanism should be in place in the workplace.
Another cause of accidents is not using the proper equipment to reach items kept on upper shelves. Items on high shelves should only be retrieved by using a ladder or step stool and not by climbing on boxes or chairs. This means that ladders and step stools must be kept in a convenient location and be in good repair.
Machines, cutting equipment and knives
Accidents and injuries can be common in the kitchen unless safety procedures are properly exercised. The type of machinery used and the high level of activity and pressure in restaurant kitchens during serving hours increase the risk of accidents.
Some common types of machinery used in kitchens are meat grinders, mixers, ice machines and dishwashing machines. Misuse or improper use of this machinery can result in cuts, limbs caught in moving parts and electric shock. To prevent these types of accidents from occurring, kitchen personnel should receive thorough training prior to using the equipment, and should follow the manufacturer’s instructions for safe operation. Other measures to prevent injury are: ensuring equipment is turned off and unplugged before cleaning; wearing snug-fitting clothing with no loose jewellery that can fall off or be caught in the equipment while operating the machinery (long-haired employees should wear hair nets for the same reason); and regular servicing by authorized personnel. One must always avoid pushing food through equipment with one’s hands.
Meat slicers are commonly used in kitchens for slicing meats, fruits and vegetables, and are potentially the most dangerous of any kitchen equipment. Mechanical machine guards must always be in place when slicers are being used. Caution must always be used when cleaning the equipment, particularly when the blades are exposed. When workers finish using the slicer, it should be returned to the zero position and unplugged.
Knives can inflict severe wounds if they are improperly used or stored. Kitchen personnel frequently use knives to chop and dice vegetables and meat prior to cooking. Methods to prevent injuries include: using knives only for the purpose for which they were intended (e.g., not as can openers); ensuring that knives are sharp, since a dull knife requires more pressure and is more likely to slip; carrying knives by the handle, with the blade pointed down; and storing knives in their proper place immediately after cleaning.
Stoves and ovens
Skin burns are the main hazard experienced by kitchen personnel using stoves and ovens. Burns can range from a slight scald to a third-degree burn. Preventive measures include always using oven mitts when lifting pot lids, when transporting pots and when removing hot items from the oven. Oven areas must always be kept free of grease build-up to prevent slipping or accidental fires. If gas ovens are being used, the pilot light must be lit before lighting the oven.
Deep fat fryers are commonly used in kitchens for deep frying various meats and vegetables. The most common hazard associated with these units is skin burns from the splashing of hot grease. Measures that can be taken to ensure the safe use of deep fat fryers are: ensuring that the oil does not overheat and start a fire; cleaning away any grease on the floor around the fryer; preventing overflows by not overfilling the fryer with oil; and using extreme care when filtering or changing the fat in the fryer. Personal protective equipment such as gloves, aprons and long sleeved shirts should always be worn.
Microwave ovens are frequently used in kitchens in order to quickly heat or cook food. The hazards associated with improperly maintained microwave ovens are electrical shock or exposure to leaked microwave radiation. Depending on the amount of leaked radiation and the length of exposure, microwave radiation can damage sensitive human organs. The radiation can also damage medical equipment implanted in the human body, such as pacemakers. Microwave ovens must be kept free of food and grease spills around the doors and seals, since these residues may prevent the oven doors from closing properly and lead to leakage of microwaves. Notices should be posted near the ovens with full instructions on their safe use. All ovens should be checked regularly for proper performance and microwave leakage. They should be repaired or adjusted by trained service personnel.
Tableside cooking
Tableside cooking or serving of flaming foods can result in severe burn injuries to both the server and the customer if improper techniques are used. This type of service should be performed only by staff trained in tableside cooking and in the use of liquid or semi-solid fuel. A carbon dioxide fire extinguisher should be available in case of fire.
Walk-in refrigerators and freezers
Large walk-in refrigerators and freezers are commonly used in restaurant kitchens to store prepared food and ingredients. In addition to the temperature, the major hazard associated with walk-in refrigeration units is that kitchen personnel can be trapped in them if the door accidentally closes behind them. All walk-in cooling equipment must be equipped with interior door opening handles and with alarm switches, and all personnel who use these units should be familiar with the location of these devices.
Care should be taken when walking inside refrigeration units since condensation can cause the floors to become very slippery. To further prevent falling injuries, refrigerator floors should always be kept clear of food scraps and grease. At closing time, a check should always be made to ensure that no one has remained behind in the refrigerators.
Temperature extremes
In the restaurant kitchen almost all personnel are exposed to heat stress; however, the chef or cook is the most exposed since he or she works in close proximity to hot stoves and ovens. Dangerously high air temperatures near stoves and ovens, combined with the heavy uniforms many chefs are required to wear, can cause a number of heat-related health problems. For example, high blood pressure, skin disorders, headaches and fatigue have often been experienced by kitchen personnel. Heat exhaustion and heat stroke can also occur. In extreme cases, fainting and loss of consciousness have been known to happen.
Methods to prevent heat stress include improving ventilation with oven hoods that draw away hot air, implementing work/rest schedules and drinking plenty of water while working. Kitchen personnel should also be educated in recognizing the symptoms of heat disorders.
Kitchen personnel are often exposed to temperature extremes when walking back and forth between walk-in refrigerators and hot kitchens. These sudden changes in temperature can result in respiratory problems. Some kitchen workers are required to work inside refrigerators for extended periods of time, unpacking produce, while arranging boxes of meats and cleaning the interior. These individuals should be given appropriate protective garments to wear while working in these areas.
Ventilation
Good ventilation systems are necessary to remove odour, grease and smoke from kitchen areas. Airborne grease can settle on kitchen equipment and cause it to become slippery. Ventilation systems include fans, air ducts and hoods. These systems should have filters removed and cleaned regularly.
Clean-up
Dish washing
Dishwashing machines can cause skin burns from handling hot dishes and can scald a worker who reaches into the machines before the dishwashing cycle is finished. Dishwashing machines should never be overloaded, since this could cause the machine to jam or to stop operating. Gloves should be used when removing hot dishes directly from the dishwasher.
Cleaning products
In order to keep restaurant kitchens as clean and hygienic as possible, several types of cleaning products and agents are used. Ammonia solutions are often used to clean grease from oven ranges and can be particularly irritating to skin and eyes. Good ventilation should always be provided by fans or oven hoods when using ammonia products.
Other products used include drain cleaners, which are caustic and can cause skin burns and damage to eyes. To protect against splashing, rubber gloves or a face mask should be worn when using these cleaners. Soaps and detergents that are present in floor cleaning products may cause dermatitis or throat irritation, if soap dust is inhaled. Disposable respirators (face masks) may be needed by employees who are sensitive to this type of dust.
To further ensure that cleaning products do not pose a risk to employees, proper handling procedures should always be followed. Cleaning products should always be stored in clearly labelled containers, far away from where food containers are stored. Cleaning products should never be combined, particularly with chlorine bleach, which can cause a hazardous situation if mixed with other cleaning products. Material safety data sheets (MSDSs) are available in many countries for learning about the contents of cleaning products, their effects and how to handle them properly.
Trash compactors
Trash compactors are used for compacting the large amounts of food waste generated in the kitchen into a much smaller volume. These machines should be designed not to operate with the lids open, in order to prevent catching hands or hair in them. The water supply should also be sufficient for the unit to operate safely and efficiently. Care should always be taken to ensure that glass, metal or plastics do not get into the compactor unit, since these materials will cause the machine to jam and lock out.
Pesticides
Pesticides are often used in restaurants to combat insects that are attracted by a food environment. Most pesticides used in restaurants and kitchens are of low hazard to humans. However, some individuals may be sensitive to such products and may develop skin irritation and other allergic reactions.
To prevent misuse of pesticides, training in the use of pesticides should be provided to janitors and other cleaning staff, and serious insect infestations should be treated by a licensed exterminator. Instructions should be printed on all pesticide containers and must be read prior to use, particularly to determine whether the pesticide can be used safely in food areas.
Food Service
Food service personnel include dining room waiters, cocktail waiters, bartenders, hosts, banquet waiters and buspersons. These individuals are responsible for serving meals and beverages, showing guests to their tables and cleaning and maintaining the dining room
Slips and falls
Injuries can result from slips on wet floors or falling over boxes, carts or garbage containers left in the kitchen or dining room area. These injuries could include sprains, broken limbs, injured necks and backs and cuts from falling on sharp objects. To help prevent these accidents, employees should wear sturdy, low-heeled, rubber-soled shoes at all times. All water, grease or food spills should be wiped up immediately, and loose electrical cords and wiring should always be taped down to the floor.
All area rugs in the dining room should be of the non-slip type, with a rubber or other appropriate backing. Carpeting should be checked for frayed or raised edges that can cause food service personnel to trip and fall. Areas where the flooring changes from carpet to tile should always be clearly marked to alert food service personnel of the surface change.
The layout of the dining room is also important in preventing accidents. Tight corners, dim lighting and small exits to the kitchen can result in collisions between food service personnel. Wider corners and clearly marked, well lit exits will lead to safer traffic patterns.
Burns
Food service personnel can suffer skin burns through spilling of hot liquids such as coffee or soup, or from melted wax if tables are candle lit. To prevent spilling of hot liquids, waiters should never overreach when serving hot beverages at a table. When filling soup bowls, food service personnel should be careful to avoid splashes and try not to overfill the bowls.
When carrying hot coffee pots and urns to the dining room, servers should use a small towel to protect hands.
Musculoskeletal injuries
Repetitive strain injuries (RSIs) and other musculoskeletal problems can be experienced by food service personnel who must routinely carry heavy trays, bend and reach to clear, wipe and set tables or carry boxes of restaurant supplies. Well designed workstations and work schedules, such as rotating tasks among food service personnel so that repetitiveness of tasks can be reduced, can diminish the risks.
Training in ergonomics (as well as training in identifying RSI risk factors) can also be helpful to all food service personnel in order to prevent strain injuries.
Many back and neck injuries occur because of improper lifting techniques. For many food service personnel, improper carrying of overloaded trays of dishes and glasses can cause strain on the back and increase the risk of dropping the tray and injuring someone. Training in proper loading and lifting of trays can reduce the risk of injury. For example, distributing the glasses and dishes evenly on the tray and placing one palm under the center of the tray while holding the front edge with the other hand will help create a safer dining room environment.
Stress
The restaurant dining room can be a very high stress environment because of the pressure of performing efficiently while working within tight schedules. Other causes of stress among food service personnel include working shifts, uncertain income because of dependence on gratuities and dealing with irate, difficult customers. Physical stressors such as noise and poor air quality can also be experienced in the restaurant environment. Some symptoms of stress can include headaches, racing heart, ulcers, irritability, insomnia and depression.
Methods to prevent or cope with stress include having workplace meetings that allow employees to share their views about improving work procedures, seminars on stress management techniques, improving air quality and reducing noise. These issues are discussed more fully elsewhere in this Encyclopaedia.
Bars and lounges
Bars or lounges can range in size from a small club or piano lounge to a vast dance/entertainment complex. Most of the hazards presented here are discussed in more detail elsewhere in this Encyclopaedia.
Broken glass is often a hazard in a bar environment because of the large amount of glassware used. Shards from broken glasses can accidentally be ingested by staff and customers. Glass fragments can cause cuts to fingers. There are several methods which can be used to minimize broken glass in the bar areas. Glasses should be inspected regularly for chips and cracks. Any damaged glasses should be discarded immediately. Picking up several glasses in one hand by placing fingers inside the glasses and bringing them together is hazardous since glasses carried in this manner may break.
A glass should never be used to scoop up the ice. A metal ice scoop should always be used when filling glasses with ice. If a glass does break in the ice area, the ice should be melted and all pieces of glass carefully removed. Broken glass should never be handled with bare hands.
Second-hand smoke. Bar personnel are exposed to heavy amounts of second-hand smoke due to the crowded conditions in many bars and lounges. These conditions can pose a risk since second-hand smoke has been linked to lung cancer and other respiratory problems. Every effort possible should be made to improve ventilation in bars and/or to set up non-smoking rooms in the bar areas.
Slips and falls. The rushed environment of a busy bar can contribute to slips and falls. Spilled drinks and leaking beverage containers can result in the area behind the bar being particularly hazardous for bartenders. Buspersons should regularly dry mop behind the bar throughout the evening. Outside the bar area, all spilled drinks should be cleaned up immediately. If the area is carpeted, there should be checks to ensure that there are no ragged edges where people could trip. All bar personnel should wear non-slip rubber-soled shoes.
If the bar has a dance floor, the floor should be made of wood or a material that allows gliding, but the floor should also be clearly distinct in colour from other walking surfaces.
Lifting. Bartenders are often required to lift heavy boxes or kegs of beer. Where possible, dollies should be used to transport kegs and boxes of beer. If proper lifting techniques are not used, back, neck and knee injuries can occur. All heavy lifting should be done using safe lifting techniques.
Bar waiters often carry heavy trays of drinks, which can put considerable stress on the back and neck. Proper tray carrying techniques should be shown to all bar waiters. Physical fitness is important for avoiding back injuries.
Noise. Excessive noise from live entertainment in bars and lounges can result in hearing damage among bar staff. Noise levels of 90 decibels (dB), which is the legal limit in some countries, like the United States, is a level that will lead to hearing loss in some individuals. Annual hearing testing (audiometric testing) is a requirement for all bar personnel exposed to 85 to 90 dB noise levels for 8 hours daily.
To prevent hearing damage among bar personnel, exposure to high noise levels should be limited to short periods of time, and attempts should be made to reduce the sound volume. If these methods are not feasible, then personal protective equipment such as ear plugs should be issued.
Compressed gases. Compressed gases are found in the bar areas where carbonated beverages are served. The canisters of gas must be kept in an upright position at all times or an explosion may occur.
Fire safety
All restaurant employees should be trained in the use of fire extinguishers and should know the location of all the fire alarms. An effective fire prevention programme includes training employees in spotting fire hazards and in proper procedures if a fire does occur. The telephone numbers of emergency-response personnel and instructions on how to summon them should be posted in a prominent area, and all employees should be familiar with an evacuation plan and escape routes. Kitchen personnel in particular should be trained in how to extinguish small fires that may occur in the kitchen.
Good housekeeping is key to fire prevention in restaurants. All areas of the restaurant should be checked for build-up of trash, grease and oil. Combustible materials such as aerosols and greasy rags should be kept in suitable covered containers and garbage cans when not in use. Ducts, filters and fans in the kitchen must be kept free of grease. This will also result in the equipment running more efficiently.
Fire exits from the restaurant must be clearly marked, and passageways to the exits must be free of boxes, trash and other debris. The use of fire detection devices and sprinkler systems should also be part of a good fire prevention programme.
Cashiers
Restaurant cashiers are generally responsible for operating the cash register, handling incoming cash, processing guest receipts and answering the phone. Restaurants can often be targets for hold-ups and robberies, resulting in injuries and even death for cashiers. Management should provide training to cashiers in proper cash-handling procedures and behaviour during a robbery. Other preventive measures are ensuring that the cashiers’ area is well lit and open, and furnishing the cashier area with alarms that can summon security during a robbery. The entire restaurant should be securable after closing, with all exits alarmed and labelled for emergency use only.
Ergonomics
Cashiers in fast food restaurants and cafeterias in particular may develop repetitive motion injuries due to the design of the job and the high workload. Precautions include well-designed work stations with cash registers at comfortable heights. Flexible seats will allow cashiers to sit and relieve lower-back and leg pressures.
Warehousing
Warehousing has long been a global industry; warehouses are integrally linked to commerce and transportation of goods—by rail, sea, air and road. Warehouses may be classified by the type of products stored: food products stored in dry, chilled or frozen sections; clothing or textiles; construction equipment or materials; machinery or machine parts. In the United States in 1995, for exemple, 1,877,000 workers were employed in trucking and warehousing (BLS 1996); this statistic cannot presently be disaggregated into workers by warehouse type or category. Warehouses might sell directly to external (retail) or internal (wholesale) customers, and the quantities retrieved for customers may be either full-pallet or less-than-full-pallet (one or more cases selected from a single pallet). Mechanical means (fork-lifts, conveyors or automatic storage and retrieval systems (AS/RS)) may be used to transport full-pallet or less-than-full-pallet loads; or workers, working without pallet movers and conveyors, may manually handle stored materials. Regardless of the nature of the business, the products stored or the mode of transportation servicing the warehouse, the basic layout is quite uniform, although the operational scale, terminology and technology will likely differ. (For additional information on AS/RS in warehousing, see Martin 1987.)
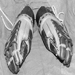
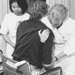
Products are delivered by shippers or suppliers to a receiving dock, where they are then entered into either a manual or computerized inventory system, assigned a storage rack or “slot” location (an address) and then transported to that location, usually by mechanical means (conveyors, AS/RS, fork-lift trucks or tractors). Once a customer order is received, the desired containers or cases must be retrieved from their slot location. Where full pallets are retrieved, mechanical means (a fork-lift or tractor operator) are used (see figure 1). When less than a full pallet load (one or more cases from a rack or slot) is to be retrieved, manual material handling is required, using a worker called a selector, who will choose the desired number of cases and place them either onto a mechanical pallet mover, a push cart or a conveyor. The individual customer order is assembled onto a pallet or similar container for shipment to the customer; a label, tag or other mark containing invoice/billing and/or routing instructions is then applied. This task may be performed by the order selector or fork-lift operator, or, where conveyors are used to deliver single cases for final assembly, by an assembler. When the order is ready for shipment, it is loaded by mechanical means onto the truck, trailer, railroad car or ship. (See figure 2).
Figure 1. A fork-lift truck in a warehouse in the United Kingdom being loaded with apples.
Figure 2. A dockworker in the United Kingdom using lifting machines to move quarters of beef.
Approximately 60% of the work activity in the warehouse is directly related to travel; the remainder relates to manual material handling. Aside from the important work of clerks, dispatchers, cleaners, supervisors and managers, the main work of the warehouse relating to the transporting and handling of goods is performed primarily by two classes of workers: fork-lift operators and selectors.
Intense worldwide competition and the rapid entrance of new firms have created the drive for increased labour and space efficiency, spawning a new discipline called warehouse management systems (WMSs) (Register 1994). These systems are becoming increasingly less expensive and more powerful; they rely on computer networks, bar coding, computer software and radio-frequency communications systems to vastly increase management and control of warehouse inventory and operations, allowing warehouses to improve customer order response times and responsiveness while dramatically increasing inventory accuracy and reducing costs (Firth 1995).
WMSs essentially computerize inventory and order dispatch systems. When incoming product from a supplier or shipper arrives at the receiving dock, bar code scanners record the product code and name, instantly updating the inventory database while assigning the incoming product an address in the warehouse. A fork-lift operator is then alerted to pick up and deliver the stock via a radio-frequency communications system mounted on the vehicle.
Orders from customers are received by another computer program which looks up the product address and availability of each item ordered in the inventory database and then sorts the customer order by the most efficient travel path to minimize travel. Labels with the product name, code and location are printed out for use by the order selectors who must then fill this order. While these features clearly help improve customer service and improve efficiency, they are important preconditions for engineered work standards (EWSs), which may pose additional health and safety hazards for both fork-lift operators and order selectors.
Information about each order—the number of cases, travel distances and so on—which is generated by the order dispatch programme can be further combined with standard or allowed times for each activity to calculate an overall standard time for selecting a particular customer order; it would be extremely time-consuming and difficult to retrieve this information without the use of the computer hardware and databases. Computer monitoring can then be used to record the elapsed time on each order, compare the actual with the allowed time and then compute an efficiency index, which any supervisor or manager can look up by pressing a few computer keys.
Warehouse EWSs have spread from the United States to Australia, Canada, the United Kingdom, Germany, Austria, Finland, Sweden, Italy, South Africa, the Netherlands and Belgium. While WMS systems themselves do not necessarily add safety and health hazards, there is considerable evidence to suggest that the resulting increased workload, lack of control over work pace and the impact of increased frequency of lifting contribute significantly to increased injury risk. In addition, the time pressure imposed by work standards may force workers to take risky short cuts and not utilize proper safe work methods. These risks and hazards are described below.
Hazards
In the most basic warehouse, regardless of the level of technology and computerization, there are a myriad of basic health and safety hazards; modern WMSs can be linked with a different order of health and safety hazards.
Basic health hazards begin with potentially toxic materials which may be stored in warehouses; examples include petroleum products, solvents and dyestuffs. These require proper labelling, employee education and training and an effective hazard communication programme (including MSDSs) for all affected workers, who often know little about the health effects of what they are handling, much less proper handling, spill and clean-up procedures. (See, for example, the ILO Chemicals Convention, 1990 (No. 170), and Recommendation, 1990 (No. 177).) Noise may be present from gasoline or LP-powered fork-lifts, conveyors, ventilation systems and pneumatically-actuated equipment. Additionally, workers who operate such equipment may be subject to whole-body vibration. (See, for example, the ILO Working Environment (Air Pollution, Noise and Vibration) Convention, 1977 (No. 148), and Recommendation, 1977 (No. 156).)
Both fork-lift operators and selectors may be exposed to diesel and gasoline exhaust from trucks at the loading and receiving docks, as well as from fork-lifts. Lighting may not be adequate for fork-lift and other vehicle traffic or for ensuring proper identification of products desired by customers. Workers assigned to work in cold and frozen storage areas may experience cold stress from exposure to cold temperatures and air recirculation systems; temperatures in many freezer storage areas can approach –20ºC, even without wind chill factors being considered. Moreover, since few warehouses are air conditioned during warm months, warehouse workers, particularly those performing manual material handling, may be exposed to heat stress problems.
Safety hazards and risks are also many and varied. Besides the more obvious hazards evident when pedestrians and any motor-driven vehicle are put into the same work area, many of the injuries occurring among warehouse workers include slips, trips and falls from floors not kept free of ice, water or spilled product or that are poorly maintained; a number of injuries involve fork-lift operators who slip or fall while mounting or dismounting their fork-lift trucks.
Workers are often exposed to falling product from overhead racks. Workers may be caught in or between fork-lift masts, forks and cargo, resulting in serious physical injury. Wooden pallets handled by workers often result in exposure to slivers and related puncture wounds. Using knives to cut apart boxes and cases often results in cuts and lacerations. Workers who move boxes or containers on or off conveyors may be exposed to in-running nip points. Selectors, assemblers and other workers engaged in manual material handling are exposed to varying degrees of risk of developing low-back pain and other related injuries. Weight-lifting regulations and recommended methods for materials handling are discussed elsewhere in the Encyclopaedia.
Recordable injuries and lost workday cases in the US warehouse industry, for example, are considerably higher than those for all industry.
Data regarding injuries (and particular back injuries) among grocery order selectors, the group at greatest risk from lifting-related injuries, are not available on a national or international scale. The US NIOSH, however, has studied lifting and other related injuries at two grocery warehouses in the United States (see US NIOSH) and found that “all order selectors have an elevated risk for musculoskeletal disorders, including low-back pain, because of the combination of adverse job factors, all contributing to fatigue, a high metabolic load and the workers’ inability to regulate their work rate because of the work requirements” (NIOSH 1995).
A comprehensive application of ergonomics to the warehouse should not be confined to lifting and to order selectors. A wide focus is required, involving detailed job analysis, careful measurement and assessment (part of the job analysis begins with the job safety analyses below). A more comprehensive look at the design of racks and shelves is required, as is establishment of a closer working relationship with suppliers to design or retrofit fork-lift controls to reduce ergonomic risk factors (extensive reaches, foot flexion and extension, winging, awkward neck and body positions) and to design containers that are less heavy and bulky, with handles or grips to reduce lifting risk.
Corrective Actions
Basic health hazards
Employers, workers and trade unions should cooperate to develop and implement an effective hazard communication programme which emphasizes the three following fundamentals:
- adequate labelling of all toxic substances
- availability of detailed MSDSs that provide more detailed information about health effects, fire, reactivity, PPE, first aid, spill clean-up and other emergency procedures
- regular and relevant worker training in proper handling of these substances.
Lack of an effective hazard communication programme is one of the most frequent standards violations cited in this industry by the US Occupational Safety and Health Administration (OSHA).
Noise and vibration from mechanical equipment, conveyors and other sources require frequent noise and vibration testing and worker training, as well as engineering controls where needed. These controls are most effective when applied at the source of the noise in the form of noise insulation, mufflers and other controls (since most fork-lift operators are seated on top of the engine, vibration and noise dampening at this point are generally most effective). Lighting should be checked frequently and maintained at levels sufficient to reduce vehicle-pedestrian accidents and ensure that product identification and other information can be easily read. Heat (or cold) stress prevention programmes should be implemented for workplaces in warm and humid climates and for selectors or fork-lift operators assigned to cold storage or freezer rooms, to ensure that workers receive adequate breaks, fluids, training and information and that other preventive measures are implemented. Finally, where diesel or petroleum-based fuels are used, exhaust systems should be periodically tested for emissions of carbon monoxide and nitrogen oxides to ensure that they are within safe levels. Proper maintenance of vehicles and restricting their use to adequately ventilated areas will also help reduce the risk of over-exposure to these emissions.
Safety hazards for fork-lift and vehicle operators
Vehicle-pedestrian accidents are a constant risk in any warehouse. Pedestrian lanes should be clearly marked and respected. All vehicle operators should receive training in the safe operation of the vehicle, including traffic rules and speed limits; refresher training should also be considered. Mirrors should be installed at busy intersections or at blind corners to enable vehicle operators to check for traffic or pedestrians before proceeding, and operators should sound their horn before proceeding; back-up beepers or signals may also be considered. Dockplates from loading and receiving docks to the truck, railroad car or barge need to be sufficient to support the load and adequately secured.
Table 2 gives a job safety analysis for fork-lift operators, with recommendations.
Table 2. Job safety analysis: Fork-lift operator.
|
Job elements or tasks |
Hazards present |
Recommended protective actions |
|
Mounting/dismounting fork-lift |
Slipping/tripping on floor (grease, water, cardboard) during mounting/dismounting; back or shoulder strain from repeated incorrect entry/exit and bumping head on protective structure |
Proper maintenance and clean-up of floors, particularly in high-traffic areas; exercising caution when mounting/dismounting; using three-point method to get in and out of fork-lift cab, being careful not to bump your head on overhead protective structure: grasping the support beams for the overhead protective structure with both hands, placing the left foot into the foot-hold (if one is provided) and then pushing off with the right foot and levering oneself into the cab. |
|
Driving with and without loads |
Pedestrian traffic and other vehicles might cross path suddenly; inadequate lighting; noise and vibration hazards; turning and twisting neck into awkward postures; steering may require wrist deviation, winging and/or excessive force; brake and accelerator pedals often require awkward foot and leg posture together with static loading |
Slowing down in high traffic areas; waiting and sounding horn at all crossings with other aisles; exercising caution around other pedestrians; observing speed limits; ensuring proper lighting is provided and maintained through periodic inspections of illumination; installing and maintaining material that dampens noise and vibration on all vehicles and equipment; regular noise testing; operators should twist their upper torso at their waist, not at their neck, particularly when looking behind mirrors installed on the fork-lift and throughout the work facility will also help reduce this risk factor; purchasing, retrofiting and maintaining power steering and steering wheels which can tilt and raise to fit operators and avoiding winging; providing frequent rest breaks for recovery from static loading fatigue; considering redesign of foot pedals to reduce angle of foot (extension) and by hinging accelerator pedals to the floor |
|
Raising or lowering forks with or without loads |
Leaning and twisting of neck in order to see load clearly; reaching for hand controls which may involve excess reach or winging |
Twisting or leaning from the waist, not from the neck; selecting fork-lifts which provide adequate visibility about the mast and which have hand controls within easy reach (located at side of operator, not on control console by steering wheel), but which are not so close or high as to involve winging; possibly retrofiting fork-lifts, with manufacturer’s permission. |
|
Filling gas tanks or changing batteries |
Changing LPG or gasoline tanks or batteries may require excessive and awkward lifting |
Using at least two employees to lift, or using a mechanical hoist; considering redesign of fork-lift to facilitate a more accessible location for fuel tank |
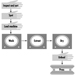
Implementing ergonomic solutions will require closer coordination with fork-lift and vehicle manufacturers; relying solely upon operator training and traffic rules will not eliminate hazards by itself. In addition, safety and health regulatory agencies have prepared mandatory standards for the design and use of fork-lifts—for example, requiring overhead guards to offer protection against falling objects (see figure 3).
Figure 3. An overhead guard fitted to a fork-lift truck.
Safety hazards for order selectors
Table 3 is a job safety analysis listing most of the corrective actions necessary to reduce the safety and lifting hazards for order selectors. However, just as improved fork-lift design to reduce ergonomic risk factors requires closer coordination with vehicle manufacturers, reducing safety and lifting hazards for order selectors requires similar coordination with designers of racking systems, consultants who design and install warehouse control systems and engineered standards systems and the vendors who store their products in the warehouse. The latter can be enlisted to design products that are less bulky, weigh less and have better handles or grips. Rack manufacturers can be very helpful in designing and retrofitting rack systems which allow the selector to stand upright during selection.
Table 3. Job safety analysis: Order selector.
|
Job elements or tasks |
Hazards present |
Recommended protective actions |
|
Mounting/dismounting pallet jack |
Slipping/tripping on floor (grease, water, cardboard) during mounting/dismounting |
Proper maintenance and clean-up of floors, particularly in high-traffic areas; exercising caution when mounting/dismounting |
|
Travel up and down aisles |
Pedestrian traffic and other vehicles might cross path suddenly; lighting; noise |
Slowing down in high-traffic areas; waiting and sounding horn at all crossings with other aisles; exercising caution around other pedestrians; observing speed limits; ensuring that proper lighting is provided and maintained; installing and maintaining material that dampens noise and vibration on all vehicles and equipment; regular noise testing |
|
Select case from rack, walk to pallet, place case on pallet |
Lifting injuries, shoulder, back and neck strain; bumping head on racks; heat stress; cold stress in freezer or cold rooms |
Working in conjunction with vendors to reduce container weight to lowest possible levels and to install handles or better grips on bulky or heavy products; storing heavy products at knuckle height or higher; not storing products to require significant lifting over the shoulder, or provide steps, stairs or platforms; providing “turntable” pallets which can be rotated when selecting products, to avoid stretching; modifying carts or pallet jacks to raise higher, to minimize bending and stooping when placing product on the cart or pallet jack; restricting the “cube” of the pallet so that over-the-shoulder lifting is minimized; providing regular heat and cold stress monitoring; providing adequate fluids, conditioning programmes, clothing and frequent rest breaks |
|
Separate pallets to wrap, mark or drop off at loading docks |
Slipping/tripping on floor (grease, water, cardboard) during mounting/dismounting |
Proper maintenance and clean-up of floors, particularly in high traffic areas; exercising caution when mounting/dismounting |
Consultants who design and install warehouse control systems and engineered standards need to be more aware of the health and safety risks concerning the effect of work intensification on manual material-handling injuries. NIOSH (1993a, 1995) has recommended that more objective forms of determining fatigue allowance, such as oxygen consumption or heart rate, be used. They have also recommended that the height of the pallet being constructed (the “cube”) be limited to no more than 150 cm, and that there be an “order break” after one pallet has been assembled by the order selector, thus increasing the frequency of recovery periods between orders. In addition to more frequent breaks, NIOSH has recommended restricting overtime for workers based on engineered standards, considering worker rotation and installing “light duty” programmes for order selectors who return from injury or leave.
Hospital Waste Management
An adaptation of current guidelines on the disposal of hospital wastes, as well as improvements in internal safety and hygiene, must be part of an overall plan of hospital waste management that establishes the procedures to follow. This should be done through properly coordinating internal and external services, as well as defining responsibilities in each of the management phases. The main goal of this plan is to protect the health of health care personnel, patients, visitors and the general public both in the hospital and beyond.
At the same time, the health of the people who come in contact with the waste once it leaves the medical centre should not be overlooked, and the risks to them should also be minimized.
Such a plan should be campaigned for and applied according to a global strategy that always keeps in mind the realities of the workplace, as well as the knowledge and the training of the personnel involved.
Stages followed in the implementation of a waste management plan are:
- informing the management of the medical centre
- designating those responsible at the executive level
- creating a committee on hospital wastes made up of personnel from the general services, nursing and medical departments that is chaired by the medical centre’s waste manager.
The group should include personnel from the general services department, personnel from the nursing department and personnel from the medical department. The medical centre’s waste manager should coordinate the committee by:
- putting together a report on the present performance of the centre’s waste management
- putting together an internal plan for advanced management
- creating a training programme for the entire staff of the medical centre, with the collaboration of the human resources department
- launching the plan, with follow-up and control by the waste management committee.
Classification of hospital wastes
Until 1992, following the classical waste management system, the practice was to classify most hospital wastes as hazardous. Since then, applying an advanced management technique, only a very small proportion of the large volume of these wastes is considered hazardous.
The tendency has been to adopt an advanced management technique. This technique classifies wastes starting from the baseline assumption that only a very small percentage of the volume of wastes generated is hazardous.
Wastes should always be classified at the point where they are generated. According to the nature of the wastes and their source, they are classified as follows:
- Group I: those wastes that can be assimilated into urban refuse
- Group II: non-specific hospital wastes
- Group III: specific hospital wastes or hazardous wastes
- Group IV: cytostatic wastes (surplus antineoplastic drugs that are not fit for therapeutic use, as well as the single-use materials that have been in contact with them, e.g., needles, syringes, catheters, gloves and IV set-ups).
According to their physical state, wastes can be classified as follows:
- solids: wastes that contain less than 10% liquid
- liquids: wastes that contain more than 10% liquid
Gaseous wastes, such as CFCs from freezers and refrigerators, are not normally captured (see article “Waste anaesthetic gases”).
By definition, the following wastes are not considered sanitary wastes:
- radioactive wastes that, because of their very nature, are already managed in a specific way by the radiological protection service
- human cadavers and large anatomical parts which are cremated or incinerated according to regulations
- waste water.
Group I Wastes
All wastes generated within the medical centre that are not directly related to sanitary activities are considered solid urban wastes (SUW). According to the local ordinances in Cataluna, Spain, as in most communities, the municipalities must remove these wastes selectively, and it is therefore convenient to facilitate this task for them. The following are considered wastes that can be assimilated to urban refuse according to their point of origin:
Kitchen wastes:
- food wastes
- wastes from leftovers or single-use items
- containers.
Wastes generated by people treated in the hospital and non-medical personnel:
- wastes from cleaning products
- wastes left behind in the rooms (e.g., newspapers, magazines and flowers)
- wastes from gardening and renovations.
Wastes from administrative activities:
- paper and cardboard
- plastics.
Other wastes:
- glass containers
- plastic containers
- packing cartons and other packaging materials
- dated single-use items.
So long as they are not included on other selective removal plans, SUW will be placed in white polyethylene bags that will be removed by janitorial personnel.
Group II Wastes
Group II wastes include all those wastes generated as a by-product of medical activities that do not pose a risk to health or the environment. For reasons of safety and industrial hygiene the type of internal management recommended for this group is different from that recommended for Group I wastes. Depending on where they originate, Group II wastes include:
Wastes derived from hospital activities, such as:
- blood-stained materials
- gauze and materials used in treating non-infectious patients
- used medical equipment
- mattresses
- dead animals or parts thereof, from rearing stables or experimental laboratories, so long as they have not been inoculated with infectious agents.
Group II wastes will be deposited in yellow polyethylene bags that will be removed by janitorial personnel.
Group III Wastes
Group III includes hospital wastes which, due to their nature or their point of origin, could pose risks to health or the environment if several special precautions are not observed during handling and removal.
Group III wastes can be classified in the following way:
Sharp and pointed instruments:
- needles
- scalpels.
Infectious wastes. Group III wastes (including single-use items) generated by the diagnosis and treatment of patients who suffer from one of the infectious diseases are listed in table 1.
Table 1. Infectious diseases and Group III wastes
|
Infections |
Wastes contaminated with |
|
Viral haemorrhagic fevers |
All wastes |
|
Brucellosis |
Pus |
|
Diphtheria |
Pharyngeal diphtheria: respiratory secretions |
|
Cholera |
Stools |
|
Creutzfelt-Jakob encephalitis |
Stools |
|
Borm |
Secretions from skin lesions |
|
Tularaemia |
Pulmonary tularaemia: respiratory secretions |
|
Anthrax |
Cutaneous anthrax: pus |
|
Plague |
Bubonic plague: pus |
|
Rabies |
Respiratory secretions |
|
Q Fever |
Respiratory secretions |
|
Active tuberculosis |
Respiratory secretions |
Laboratory wastes:
- material contaminated with biological wastes
- waste from work with animals inoculated with biohazardous substances.
Wastes of the Group III type will be placed in single-use, rigid, colour-coded polyethylene containers and hermetically sealed (in Cataluna, black containers are required). The containers should be clearly labelled as “Hazardous hospital wastes” and kept in the room until collected by janitorial personnel. Group III wastes should never be compacted.
To facilitate their removal and reduce risks to a minimum, containers should not be filled to capacity so that they can be closed easily. Wastes should never be handled once they are placed in these rigid containers. It is forbidden to dispose of biohazardous wastes by dumping them into the drainage system.
Group IV Wastes
Group IV wastes are surplus antineoplastic drugs that are not fit for therapeutic use, as well as all single-use material that has been in contact with the same (needles, syringes, catheters, gloves, IV set-ups and so on).
Given the danger they pose to persons and the environment, Group IV hospital wastes must be collected in rigid, watertight, sealable single-use, colour-coded containers (in Cataluna, they are blue) which should be clearly labelled “Chemically contaminated material: Cytostatic agents”.
Other Wastes
Guided by environmental concerns and the need to enhance waste management for the community, medical centres, with the cooperation of all personnel, staff and visitors, should encourage and facilitate the selective disposal (i.e., in special containers designated for specific materials) of recyclable materials such as:
- paper and cardboard
- glass
- used oils
- batteries and power cells
- toner cartridges for laser printers
- plastic containers.
The protocol established by the local sanitation department for the collection, transport and disposal of each of these types of materials should be followed.
Disposal of large pieces of equipment, furniture and other materials not covered in these guidelines should follow the directions recommended by the appropriate environmental authorities.
Internal transport and storage of wastes
Internal transport of all the wastes generated within the hospital building should be done by the janitorial personnel, according to established schedules. It is important that the following recommendations be observed when transporting wastes within the hospital:
- The containers and the bags will always be closed during transport.
- The carts used for this purpose will have smooth surfaces and be easy to clean.
- The carts will be used exclusively for transporting waste.
- The carts will be washed daily with water, soap and lye.
- The waste bags or containers should never be dragged on the floor.
- Waste should never be transferred from one receptacle to another.
The hospital must have an area specifically for the storage of wastes; it should conform to current guidelines and fulfil, in particular, the following conditions:
- It should be covered.
- It should be clearly marked by signs.
- It should be built with smooth surfaces that are easy to clean.
- It should have running water.
- It should have drains to remove the possible spillage of waste liquids and the water used for cleaning the storage area.
- It should be provided with a system to protect it against animal pests.
- It should be located far away from windows and from the intake ducts of the ventilation system.
- It should be provided with fire extinguishing systems.
- It should have restricted access.
- It should be used exclusively for the storage of wastes.
All the transport and storage operations that involve hospital wastes must be conducted under conditions of maximum safety and hygiene. In particular, one must remember:
- Direct contact with the wastes must be avoided.
- Bags should not be overfilled so that they may be closed easily.
- Bags should not be emptied into other bags.
Liquid Wastes: Biological and Chemical
Liquid wastes can be classified as biological or chemical.
Liquid biological wastes
Liquid biological wastes can usually be poured directly into the hospital’s drainage system since they do not require any treatment before disposal. The exceptions are the liquid wastes of patients with infectious diseases and the liquid cultures of microbiology laboratories. These should be collected in specific containers and treated before being dumped.
It is important that the waste be dumped directly into the drainage system with no splashing or spraying. If this is not possible and wastes are gathered in disposable containers that are difficult to open, the containers should not be forced open. Instead, the entire container should be disposed of, as with Group III solid wastes. When liquid waste is eliminated like Group III solid waste, it should be taken into consideration that the conditions of work differ for the disinfection of solid and liquid wastes. This must be kept in mind in order to ensure the effectiveness of the treatment.
Liquid chemical wastes
Liquid wastes generated in the hospital (generally in the laboratories) can be classified in three groups:
- liquid wastes that should not be dumped into the drains
- liquid wastes that can be dumped into the drains after being treated
- liquid wastes that can be dumped into the drains without being previously treated.
This classification is based on considerations related to the health and quality of life of the entire community. These include:
- protection of the water supply
- protection of the sewer system
- protection of the waste water purification stations.
Liquid wastes that can pose a serious threat to people or to the environment because they are toxic, noxious, flammable, corrosive or carcinogenic should be separated and collected so that they can subsequently be recovered or destroyed. They should be collected as follows:
- Each type of liquid waste should go into a separate container.
- The container should be labelled with the name of the product or the major component of the waste, by volume.
- Each laboratory, except the pathological anatomy laboratory, should provide its own individual receptacles to collect liquid wastes that are correctly labelled with the material or family of materials it contains. Periodically (at the end of each work day would be most desirable), these should be emptied into specifically labelled containers which are held in the room until collected at appropriate intervals by the assigned waste removal subcontractor.
- Once each receptacle is correctly labelled with the product or the family of products it contains, it should be placed in specific containers in the labs.
- The person responsible for the laboratory, or someone directly delegated by that person, will sign and stamp a control ticket. The subcontractor will then be responsible for delivering the control ticket to the department that supervises safety, hygiene and the environment.
Mixtures of chemical and biological liquid wastes
Treatment of chemical wastes is more aggressive than treatment of biological wastes. Mixtures of these two wastes should be treated using the steps indicated for liquid chemical wastes. Labels on containers should note the presence of biological wastes.
Any liquid or solid materials that are carcinogenic, mutagenic or teratogenic should be disposed of in rigid colour-coded containers specifically designed and labelled for this type of waste.
Dead animals that have been inoculated with biohazardous substances will be disposed of in closed rigid containers, which will be sterilized before being reused.
Disposal of Sharp and Pointed Instruments
Sharp and pointed instruments (e.g., needles and lancets), once used, must be placed in specifically designed, rigid “sharps” containers that have been strategically placed throughout the hospital. These wastes will be disposed of as hazardous wastes even if used on uninfected patients. They must never be disposed of except in the rigid sharps container.
All HCWs must be repeatedly reminded of the danger of accidental cuts or punctures with this type of material, and instructed to report them when they occur, so that appropriate preventive measures may be instituted. They should be specifically instructed not to attempt to recap used hypodermic needles before dropping them into the sharps container.
Whenever possible, needles to be placed in the sharps container without recapping may be separated from the syringes which, without the needle, can generally be disposed of as Group II waste. Many sharps containers have a special fitting for separating the syringe without risk of a needlestick to the worker; this saves space in the sharps containers for more needles. The sharps containers, which should never be opened by hospital personnel, should be removed by designated janitorial personnel and forwarded for appropriate disposal of their contents.
If it is not possible to separate the needle in adequately safe conditions, the whole needle-syringe combination must be considered as biohazardous and must be placed in the rigid sharps containers.
These sharps containers will be removed by the janitorial personnel.
Staff Training
There must be an ongoing training programme in waste management for all hospital personnel aimed at indoctrinating the staff on all levels with the imperative of always following the established guidelines for collecting, storing and disposing wastes of all kinds. It is particularly important that the housekeeping and janitorial staffs be trained in the details of the protocols for recognizing and dealing with the various categories of hazardous waste. The janitorial, security and fire-fighting staff must also be drilled in the correct course of action in the event of an emergency.
It is also important for the janitorial personnel to be informed and trained on the correct course of action in case of an accident.
Particularly when the programme is first launched, the janitorial staff should be instructed to report any problems that may hinder their performance of these assigned duties. They may be given special cards or forms on which to record such findings.
Waste Management Committee
To monitor the performance of the waste management programme and resolve any problems that may arise as it is implemented, a permanent waste management committee should be created and meet regularly, quarterly at a minimum. The committee should be accessible to any member of the hospital staff with a waste disposal problem or concern and should have access as needed to top management.
Implementing the Plan
The way the waste management programme is implemented may well determine whether it succeeds or not.
Since the support and cooperation of the various hospital committees and departments is essential, details of the programme should be presented to such groups as the administrative teams of the hospital, the health and safety committee and the infection control committee. It is necessary also to obtain validation of the programme from such community agencies as the departments of health, environmental protection and sanitation. Each of these may have helpful modifications to suggest, particularly with respect to the way the programme impinges on their areas of responsibility.
Once the programme design has been finalized, a pilot test in a selected area or department should permit rough edges to be polished and any unforeseen problems resolved. When this has been completed and its results analysed, the programme may be implemented progressively throughout the entire medical centre. A presentation, with audio-visual supports and distribution of descriptive literature, can be delivered in each unit or department, followed by delivery of bags and/or containers as required. Following the start-up of the programme, the department or unit should be visited so that any needed revisions may be instituted. In this manner, the participation and support of the entire hospital staff, without which the programme would never succeed, can be earned.
Hotels
Departmental operations within a hotel usually consist of: reception, which oversees reservations and guest reception services; housekeeping, which cleans and stocks guest rooms and public areas; maintenance, which does heavy cleaning, setup, painting, repair and remodelling; food and beverage; office and accounting; and other miscellaneous services such as health centres, beauty salons, barber shops and gift shops.
Hazards by Department
Reception
Reception includes the following job classifications: managers, desk clerks, telephone operators, bell and door staff, security personnel, concierges, drivers and parking attendants. Key job safety and health hazards include:
Visual display units (VDUs). Desk clerks, telephone operators and other front desk personnel often use computer terminals. It has been shown that computer use under some conditions can cause various repetitive strain injuries (RSIs), such as carpal tunnel syndrome (in the wrist) as well as shoulder, neck and back problems. Employees are at special risk if workstations are poorly adjusted and require awkward body postures, or if VDU work is continuous without adequate breaks. VDU work can also produce eyestrain and other visual problems. Preventive measures include providing adjustable computer workstations, training staff on how to adjust their equipment properly and maintain correct postures, and ensuring that employees take rest and stretch breaks.
Shift work. Many guest service employees work shifts that can vary according to the level of daily hotel occupancy. Staff members may be required to work both day and evening shifts, or split shifts with random days off. Physiological and psychological health effects of shift work can include disturbed sleep patterns, stomach trouble and stress. Staff may also use drugs or medicines as sleeping aids to adjust to unusual work hours. Workers should receive training on health hazards related to shift work. Whenever possible workers should have adequate time off between rotating shifts to allow for sleep adjustments.
Special consideration should also be paid to other issues associated with swing and graveyard shifts, such as safety concerns, access to healthy meals while on duty and proper ventilation (as air conditioning is often turned off in the evening).
Poor indoor-air quality. Employees can be exposed to second-hand smoke in the lobby, bar, dining rooms and guest rooms. Where ventilation is inadequate, second-hand smoke can pose a risk of cancer and heart disease.
Lifting. Lifting hazards affect staff who load, unload and carry luggage and convention supplies. Back, neck, knee and ankle injuries can result when staff are not trained on proper lifting techniques. Luggage carts should be available. They should be well maintained and equipped with smooth-rolling wheels and safety locks.
Parking and garage hazards. Garage jobs in hotels range from valet parking, to collecting fees, to site maintenance. Employees may work part time, and turnover is often high.
Workers can be struck by vehicles, can inhale exhaust fumes (which contain carbon monoxide among other toxins), or can be exposed to chemicals in automotive products, cleaning products and paints. They can be exposed to asbestos from brake dusts. They can fall from ladders or other maintenance equipment, and can trip or fall due to fluid spills, broken pavement or snow. They can also be assaulted or robbed.
Measures to prevent auto accidents include having clearly marked traffic lanes and walkways, warnings indicating the direction of traffic flow, stop signs for crossing lanes and roped-off areas wherever maintenance work is being done.
Workers exposed to car exhaust, paint fumes and other chemicals should have access to fresh air. Training should be provided about chemical hazards and health effects.
Kerosene heaters sometimes used to warm workers in parking garages can release toxic fumes, and should be prohibited. If heaters are necessary, properly guarded and grounded electric heaters should be used.
Oil spills, water and debris should be cleaned up immediately to prevent falls. Snow should be removed and not allowed to accumulate.
Housekeeping
This group includes housekeepers, laundry workers and supervisors. The department is usually responsible for cleaning and maintaining guest rooms, public areas and meeting and recreational facilities. It may also supply laundry services for guests. Typical safety and health hazards can include:
Repetitive strain injuries (RSIs). Housekeepers are subject to strains from repeated lifting, pushing, bending, reaching and wiping when cleaning bathrooms, changing bed linen, vacuuming rugs, wiping furniture and walls and pushing supply carts from room to room. Laundry workers are also at risk for to RSI injuries due to reaching and to rapid motions from folding, sorting and loading laundry.
Housekeeping carts help transport supplies and equipment, but carts need to be well maintained, with smooth-rolling wheels, and designed to carry heavy loads without tipping over. Carts also need to be relatively light and easy to manoeuvre, with sufficient clearance above the cart so housekeepers can see where they are going.
Training in both ergonomics and proper lifting should be available for housekeepers and laundry workers. Training should include RSI risk factors and methods for reducing them.
Chemical products. Housekeepers and maids use chemical cleaning products for sinks, tubs, toilets, floors and mirrors. Some products can cause dermatitis, respiratory distress and other problems. Some general cleaning agents containing ammonia, detergents and solvents can irritate the skin, eyes, nose and throat. Certain solvent-based products can damage the kidneys and reproductive organs. Disinfectants often contain phenol compounds, which can cause irritation and are suspected to cause cancer.
Preventive measures include supplying protective gloves and substituting with less hazardous products. Proper ventilation should be provided through open windows, mechanical air vents or fans. Chemical storage areas should be well maintained and away from break and eating areas.
Training should be provided about chemical hazards and health effects. It should be conducted in a way staff can understand. To be effective, some training procedures may need translation into workers’ first languages.
Trips and falls. Housekeepers are required to move quickly. Speed can result in slipping on wet floors, falling from tubs and other surfaces when cleaning, and tripping over cords, sheets and bed covers and debris. Laundry staff may slip on wet floors.
Training should be offered emphasizing safety measures to prevent falls and work methods that reduce the need to rush.
Cuts. Cuts from glass, discarded razor blades and debris can be reduced by using liners in wastebaskets and by installing razor blade disposal devices in bathrooms. Workers should be trained in proper waste-handling techniques.
Needlesticks. Used hypodermic needles left by guests in wastebaskets, linens or rooms put hotel staff at risk of getting infectious diseases from accidental punctures. Housekeeping and laundry personnel are the most likely to encounter a discarded needle. Staff should be instructed on how to report and dispose of needles. Staff should have access to approved types of needle receptacle boxes. Management should also have effective medical and counselling procedures to assist staff who have been stuck by a discarded needle.
Heat stress. Hotel laundry workers wash, iron, fold and deliver linen. Heat from machinery, combined with poor ventilation, can result in an oppressive work environment and cause heat stress. Symptoms may include headache, nausea, irritability, fatigue, fainting and accelerated pulse. Eventually these can lead to convulsions and more serious problems if early symptoms are not treated.
Heat stress can be prevented by installing air conditioning, insulating sources of heat, ventilating hot areas with hoods that draw hot air away, taking frequent short breaks in cool areas, drinking plenty of water and wearing loose-fitting clothes. If the work area is only moderately hot (below 35°C), fans may be useful.
Maintenance
Maintenance staff do heavy cleaning, set-up, painting, repair, remodelling and grounds work. Hazards include:
Chemical products. Maintenance staff may use toxic cleaning products to strip and polish floors as well as to clean carpets, walls, furniture, brass fixtures and marble. Certain products can irritate the skin, eyes, nose and throat; can affect the nervous system; and can damage the kidneys, lungs, liver and reproductive system.
Solvents may be present in painting and remodelling materials. Fast-drying paints are used to enable rooms and public areas to be available quickly, but these paints contain high solvent concentrations. Glues used in laying carpet and flooring and in other remodelling jobs may also contain toxic solvents. Solvents can irritate the skin, eyes, nose and throat. Some may damage the nervous system, kidneys, lungs, liver and reproductive organs. Certain solvents are known to cause cancer.
Pesticides and herbicides may be applied in kitchens, dining rooms, public areas, locker rooms and outside the hotel in gardens and driveways. Some of these chemicals can cause respiratory problems; can irritate the skin, eyes, nose and throat; and can damage the nervous system, kidneys, liver and other organs.
Preventive measures include training about chemicals, proper ventilation and proper use of personal protective equipment. If respirators are required, staff should be trained on how to select the proper respirator and cartridge, and how to fit test, use and maintain the equipment. In addition, employees should be given a medical exam to ensure that they are physically fit to work wearing a respirator. Wherever possible, less toxic chemicals should be used.
Asbestos. Asbestos is present in many hotels. Used for years as an insulator and fire retardant, it is found around pipes and in ceiling materials and floor coverings. This highly toxic substance can cause asbestosis, lung cancer or mesothelioma (another form of cancer).
Asbestos is most hazardous when it ages or is damaged. It may begin to break up, creating dust. Hotels should regularly inspect areas where asbestos-containing materials are present to ensure that the asbestos is in good condition.
Extreme caution must be used to protect workers and guests when asbestos dust is present (through ageing or damage or during asbestos abatement jobs). Hotel workers and guests must be kept away from the area, warning signs must be posted and only skilled and licensed personnel should be hired to abate the hazard. The area should be inspected by qualified professionals when work in completed. In new construction or renovation, substitute products should be used in lieu of asbestos.
Trips and falls. Maintenance staff may fall when using ladders and hoists to reach high places such as ceilings, chandeliers, light fixtures, walls and balconies. Training should be provided.
Food and beverage
These staff members include kitchen workers, dishwashers, restaurant servers, room service personnel, hosts and bartenders. Among the hazards are:
Repetitive strain injuries (RSIs). RSIs can occur when room service personnel or restaurant servers deliver food. Trays can be heavy and the server may have to walk long distances. To reduce the risk of injury, room service carts can be used to deliver orders. Carts should be easy to manoeuvre and well maintained. If carts are equipped with heating boxes, the staff should be trained on their proper use.
Trips and falls. Floor surfaces in the kitchen, as well as in all areas to which serving personnel must go, should be kept clean and dry to prevent falls. Spills should be cleaned up immediately. See also the article “Restaurants” in this chapter.
Miscellaneous services
Swimming pools and fitness centres. Many hotels provide swimming facilities or fitness centres for guests. Often showers, saunas, whirlpools, weight rooms and locker rooms are available.
Chemicals used to clean and disinfect showers and locker rooms can cause skin and respiratory irritation. In addition, employees who maintain swimming pools may handle solid or gaseous chlorine. Chlorine leaks can cause burns and severe respiratory problems. If mishandled, it can explode. Employees should be trained on how to handle all these chemicals properly.
Workers who maintain pool and fitness facilities are exposed to injuries from slips and falls. Nonskid, well-maintained and well-drained walking surfaces are important. Water puddles should be wiped up immediately.
Gift shops. Hotels often provide gift and convenience shops for guests. Employees are subject to falls, strains and cuts associated with unpacking and stocking merchandise. They should be trained on proper lifting techniques and should have hand carts to aid in transporting merchandise. Aisles should be kept clear to avoid accidents.
Beauty salons and barber shops. Barbers and cosmetologists risk injuries including skin irritation from hair chemicals, burns from hot towels and curling irons, and cuts and punctures from scissors and razors.
Special hazards include a risk of respiratory problems and possibly even cancer from repeated exposure to certain chemicals such as some hair dye ingredients. There is also a risk of RSIs due to continual use of the hands in awkward postures. Employees should be trained to recognize chemical and ergonomic hazards, and to work in a way that minimizes the risk. They should be supplied with proper gloves and aprons when working with dyes, bleaches, permanent-wave solutions and other chemical products. Shop areas should be properly ventilated to provide fresh air and remove fumes, especially in areas where employees are mixing solutions. Scissors and razors should be properly maintained for ease in cutting, as discussed elsewhere in this Encyclopaedia.
All Occupations
Sexual harassment. Housekeepers and other hotel employees may be exposed to sexual advances from guests or others. Employees should be trained about sexual harassment issues.
Management should have a clear policy on how to report and respond to such incidents.
Fires and other emergencies. Emergencies and disasters can result in loss of life and injuries to both guests and staff. Hotels should have clear emergency response plans, including designated evacuation routes, emergency procedures, an emergency communication system and methods for clearing guests out of the hotel quickly. Certain managers as well as the switchboard operators should have clear instructions on how to coordinate emergency communication with guests and staff.
Staff training and joint labor-management safety meetings are vital components of an effective emergency prevention and response programme. Training sessions and meetings should include translation for staff who need it. Training should be frequent since there is high turnover among hotel workers. Periodic emergency drills should be scheduled, incorporating “walk-throughs” of evacuation routes, staff roles and other emergency procedures.
There should also be a fire prevention programme, including regular inspections. Management and staff members should ensure that exits are not blocked, flammable materials are properly stored, kitchen hoods are regularly cleaned and electrical equipment is well maintained (without frayed wires). Fire retardant materials should be used in interior decorating projects, and there should be screens around fireplaces. Ashtrays should be properly emptied, and candles should be used only in semi-enclosed containers.
Hotel accommodations as well as all facilities attached to the hotel, such as beauty shops, restaurants and gift shops, should be in compliance with all fire codes. Guest rooms and public areas should be equipped with smoke detectors and water sprinklers. Fire extinguishers should be available throughout the hotel. Exits should be well marked and illuminated. Back-up generators should be available to provide emergency lighting and other services.
Evacuation instructions should be posted in each guest room. Many hotels now provide in-room videos with information on fire safety. Guests who are hearing impaired should have rooms equipped with alarms using bright lights to alert them to an emergency. Visually impaired guests should receive emergency procedure information in Braille.
There should be a central alarm system which can display the exact location of a suspected fire. It should also automatically communicate to local emergency services, and broadcast messages over the public address system for guests and staff.
Managing Hazardous Waste Disposal Under ISO 14000
A formal Environmental Management System (EMS), using the International Organization for Standardization (ISO) standard 14001 as the performance specification, has been developed and is being implemented in one of the largest teaching health care complexes in Canada. The Health Sciences Centre (HSC) consists of five hospitals and associated clinical and research laboratories, occupying a 32-acre site in central Winnipeg. Of the 32 segregated solid waste streams at the facility, hazardous wastes account for seven. This summary focuses on the hazardous waste disposal aspect of the hospital’s operations.
ISO 14000
The ISO 14000 standards system is a typical continuous improvement model based on a controlled management system. The ISO 14001 standard addresses the environmental management system structure exclusively. To conform with the standard, an organization must have processes in place for:
- adopting an environmental policy that sets environmental protection as a high priority
- identifying environmental impacts and setting performance goals
- identifying and complying with legal requirements
- assigning environmental accountability and responsibility throughout the organization
- applying controls to achieve performance goals and legal requirements
- monitoring and reporting environmental performance; auditing the EMS system
- conducting management reviews/ identifying opportunities for improvement.
The hierarchy for carrying out these processes in the HSC is presented in table 1.
Table 1. HSC EMS documentation hierarchy
|
EMS level |
Purpose |
|
Governance document |
Includes the Board’s expectations on each core performance category and its requirements for corporate competency in each category. |
|
Level 1 |
Prescribes the outputs that will be delivered in response to customer and stakeholder (C/S) needs (including government regulatory requirements). |
|
Level 2 |
Prescribes the methodologies, systems, processes and resources to be used for achieving C/S requirements; the goals, objectives and performance standards essential for confirming that the C/S requirements have been met (e.g., a schedule of required systems and processes including responsibility centre for each). |
|
Level 3 |
Prescribes the design of each business system or process that will be operated to achieve the C/S requirements (e.g., criteria and boundaries for system operation; each information collection and data reporting point; position responsible for the system and for each component of the process, etc.). |
|
Level 4 |
Prescribes detailed task instructions (specific methods and techniques), for each work activity (e.g., describe the task to be done; identify the position responsible for completing the task; state skills required for the task; prescribe education or training methodology to achieve required skills; identify task completion and conformance data, etc.). |
|
Level 5 |
Organizes and records measurable outcome data on the operation of systems, processes and tasks designed to verify completion according to specification. (e.g., measures for system or process compliance; resource allocation and budget compliance; effectiveness, efficiency, quality, risk, ethics, etc.). |
|
Level 6 |
Analyses records and processes to establish corporate performance in relation to standards set for each output requirement (Level 1) related to C/S needs (e.g., compliance, quality, effectiveness, risk, utilization, etc.); and financial and staff resources. |
ISO standards encourage businesses to integrate all environmental considerations into mainstream business decisions and not restrict attention to concerns that are regulated. Since the ISO standards are not technical documents, the function of specifying numerical standards remains the responsibility of governments or independent expert bodies.
Management System Approach
Applying the generic ISO framework in a health care facility requires the adoption of management systems along the lines of those in table 1, which describes how this has been addressed by the HSC. Each level in the system is supported by appropriate documentation to confirm diligence in the process. While the volume of work is substantial, it is compensated by the resulting performance consistency and by the “expert” information that remains within the corporation when experienced persons leave.
The main objective of the EMS is to establish consistent, controlled and repeatable processes for addressing the environmental aspects of the corporation’s operations. To facilitate management review of the hospital’s performance, an EMS Score Card was conceived based on the ISO 14001 standard. The Score Card closely follows the requirements in the ISO 14001 standard and, with use, will be developed into the hospital’s audit protocol.
Application of the EMS to the Hazardous Waste Process
Facility hazardous waste process
The HSC hazardous waste process currently consists of the following elements:
- procedure statement assigning responsibilities
- process description, in both text and flowchart formats
- Disposal Guide for Hazardous Waste for staff
- education programme for staff
- performance tracking system
- continuous improvement through multidisciplinary team process
- a process for seeking external partners.
The roles and responsibilities of the four main organizational units involved in the hazardous waste process are listed in table 2.
Table 2. Role and responsibilities
|
Organizational unit |
Responsibility |
|
S&DS |
Operates the process and is the process owner/leader, and arranges responsible disposal of waste. |
|
UD–User Departments |
Identifies waste, selects packaging, initiates disposal activities. |
|
DOEM |
Provides specialist technical support in identifying risks and protective measures associated with materials used by HSC and identifies improvement opportunities. |
|
EPE |
Provides specialist support in process performance monitoring and reporting, identifies emerging regulatory trends and compliance requirements, and identifies improvement opportunities. |
|
ALL–All participants |
Shares responsibility for process development activities. |
Process description
The initial step in preparing a process description is to identify the inputs (see table 3 ).
Table 3. Process inputs
|
Organizational unit |
Examples of process inputs and supporting inputs |
|
S&DS (S&DS) |
Maintain stock of Hazardous Waste Disposal Requisition forms and labels |
|
S&DS (UD, DOEM, EPE) (S&DS) |
Maintain supply of packaging containers in warehouse for UDs |
|
DOEM |
Produce SYMBAS Classification Decision Chart. |
|
EPE |
Produce the list of materials for which HSC is registered as a waste generator with regulatory department. |
|
S&DS |
Produce a database of SYMBAS classifications, packaging requirements, TDG classifications, and tracking information for each material disposed by HSC. |
The next process component is the list of specific activities required for proper disposal of waste (see table 4 ).
Table 4. List of activities
|
Unit |
Examples of activities required |
|
UD |
Order Hazardous Waste Disposal Requisition, label and packaging from S&DS as per standard stock ordering procedure. |
|
S&DS |
Deliver Requisition, label and packaging to UD. |
|
UD |
Determine whether a waste material is hazardous (check MSDS, DOEM, and such considerations as dilution, mixture with other chemicals, etc.). |
|
UD |
Assign the Classification to the waste material using SYMBAS Chemical Decision Chart and WHMIS information. Classification can be checked with the S&DS Data Base for materials previously disposed by HSC. Call first S&DS and second DOEM for assistance if required. |
|
UD |
Determine appropriate packaging requirements from WHMIS information using professional judgement or from S&DS Data Base of materials previously disposed by HSC. Call first S&DS and second DOEM for assistance if required. |
Communication
To support the process description, the hospital produced a Disposal Guide for Hazardous Waste to assist staff in the proper disposal of hazardous waste materials. The guide contains information on the specific steps to follow in identifying hazardous waste and preparing it for disposal. Supplemental information is also provided on legislation, the Workplace Hazardous Materials Information System (WHMIS) and key contacts for assistance.
A database was developed to track all relevant information pertaining to each hazardous waste event from originating source to final disposal. In addition to waste data, information is also collected on the performance of the process (e.g., source and frequency of phone calls for assistance to identify areas which may require further training; source, type, quantity and frequency of disposal requests from each user department; consumption of containers and packaging). Any deviations from the process are recorded on the corporate incident reporting form. Results from performance monitoring are reported to the executive and the board of directors. To support effective implementation of the process, a staff education programme was developed to elaborate on the information in the guide. Each of the core participants in the process carries specific responsibilities on staff education.
Continuous Improvement
To explore continuous improvement opportunities, the HSC established a multidisciplinary Waste Process Improvement Team. The Team’s mandate is to address all issues pertaining to waste management. Further to encourage continuous improvement, the hazardous waste process includes specific triggers to initiate process revisions. Typical improvement ideas generated to date include:
- prepare list of high hazard materials to be tracked from time of procurement
- develop material “shelf life” information, where appropriate, for inclusion in the materials classification database
- review shelving for physical integrity
- purchase spill containing trays
- examine potential for spills entering sewer system
- determine whether present storage rooms are adequate for anticipated waste volume
- produce a procedure for disposing of old, incorrectly identified materials.
The ISO standards require regulatory issues to be addressed and state that business processes must be in place for this purpose. Under the ISO standards, the existence of corporate commitments, performance measuring and documentation provide a more visible and more convenient trail for regulators to check for compliance. It is conceivable that the opportunity for consistency provided by the ISO documents could automate reporting of key environmental performance factors to government authorities.
Health Effects and Disease Patterns
Hotels and restaurants constitute a large, diversified, labour-intensive service industry made up predominantly of small enterprises. While there are a number of giant corporations, some of which attempt to standardize procedures and working rules, their hotels and restaurants are usually operated individually, often on a franchise rather than a directly owned basis. Frequently, the eating and drinking establishments in hotels are leased to franchise operators.
There is a high degree of failure among the enterprises in this industry, with many being very close to the edge of financial insolvency for some time before closing their doors. This often dictates economies in staffing, in the purchase and maintenance of equipment and in the provision of necessary supplies. It also often forces neglect of employee training programmes and a reluctance to spend scarce resources on measures to promote and protect employee safety and health.
The majority of the jobs are unskilled and provide low or minimal wages (in some of the jobs, these may be supplemented by gratuities that depend on the largesse of the patrons). Consequently, they attract only workers with minimal education and experience, and because minimal language and literacy skills are required, many of the jobs are filled by immigrants and ethnic minorities. Many are entry-level positions with little or no opportunities for advancement. Shift work is required in hotels because they operate around the clock; in restaurants, the flurries of activity at meal times are often covered by part-time workers. Because their patronage is seasonal, many establishments curtail their operations or shut down entirely during the off-season, and, as a result, there may be little or no job security. The end result of all of this is a high rate of turnover in the workforce.
Job Stress
Because of the periods of intense activity and the necessity of pleasing the patrons on whose gratuities their livelihoods often depend, many of the workers in this industry are subject to high levels of job stress. They must often comply with seemingly unreasonable or even impossible requests and may be subjected to abusive behaviour on the part of supervisors as well as customers. Many of the jobs, particularly those in kitchens and laundries, must be carried out in stressful environments featuring high heat and humidity, poor ventilation, poor lighting and noise (Ulfvarson, Janbell and Rosen 1976).
Violence
Hotels and restaurants rank high on the lists of workplaces with the greatest incidence of occupational violent crime. According to one survey, over 50% of such incidents involving hotel and restaurant workers resulted in death (Hales et al. 1988). These workers are exposed to many of the risk factors for workplace homicide: exchange of money with the public, working alone or in small numbers, working late night or early morning hours and guarding valuable property or possessions (Warshaw and Messite 1996).
Types of Injuries and Diseases
According to the US Bureau of Labor Statistics, food and beverage preparation and housekeeping departments accounted for 76% of all work injuries and accidents in hotels (US Bureau of Labor Statistics 1967), while a Danish survey found that these were predominantly skin and musculoskeletal problems (Direktoratet for Arbejdstilsynet 1993). Most of the skin problems may be traced to exposure to soap and hot water, to the chemicals in detergents and other cleaning/polishing materials and, in some instances, to pesticides. Except for the special problems noted below, the majority of musculoskeletal injuries result from slips and falls and from lifting and handling heavy and/or bulky objects.
Sprains, strains and repetitive motion injuries
Back injuries and other sprains and strains commonly occur among doormen, porters and bellmen lifting and carrying luggage (a particular problem when large tour groups arrive and depart); kitchen workers and others receiving and storing bulk supplies; and housekeeping workers lifting mattresses, making beds and handling bundles of laundry. A unique type of injury is carpal tunnel syndrome among food service workers who use scoops to prepare servings of hard ice cream and other frozen desserts.
Cuts and lacerations
Cuts and lacerations are common among restaurant workers and dishwashers who deal with broken glass and crockery, and who handle or clean sharp knives and slicing machines. They are also common among chambermaids who encounter broken glasses and discarded razor blades in cleaning out waste baskets; they may be protected by lining the baskets with plastic bags which can be removed en masse.
Burns and scalds
Burns and scalds are common among chefs, dishwashers and other kitchen workers and laundry workers. Grease burns occur from splatters during cooking or as food is dropped into deep-fat fryers, when hot grease is added, filtered or removed, and when grills and fryers are cleaned while hot. Many result when workers slip on wet or slippery floors and fall on or against hot grills and open flames. A unique type of burn occurs in restaurants where flaming desserts, entrees and drinks are served (Achauer, Bartlett and Allyn 1982).
Industrial chemicals
Hotel and restaurant establishments share with other small enterprises a propensity for improper storage, handling and disposal of industrial chemicals. All too frequently cleaning supplies, disinfectants, pesticides and other “household” poisons are stored in unlabelled containers, are placed above open food containers or food preparation areas or, when used in spray form, are excessively inhaled.
The fast food industry
The fast food industry, one of the most rapidly growing in the United States and becoming increasingly popular in other countries, is one of the largest employers of young people. Lacerations and burns are common hazards in these establishments. It has also been noted that the home delivery of pizzas and other prepared food is often extremely hazardous because of policies which encourage reckless driving on bicycles as well as in motor vehicles (Landrigan et al. 1992).
Preventive Measures
Standardized work processes, adequate training and proper supervision are key elements in the prevention of work-related injuries and illnesses among workers in the hotel and restaurant industry. It is essential that, because of their generally low educational levels and language difficulties, the educational materials and training exercises be readily understood (they may have to be conducted in several languages). Also, because of the high turnover, training must be repeated at frequent intervals. The training exercises should be supplemented by frequent inspections to assure that the basic principles of good housekeeping and elimination of accident hazards are observed.
Emergency drills
In addition to regular inspections to verify that firefighting equipment (e.g., smoke alarms, sprinkler systems, fire extinguishers and hoses and emergency lighting equipment) is in good working order and that emergency exits are clearly marked and not blocked, frequent drills are necessary to train the workers in how to prevent themselves and the patrons from being trapped and overcome in the event of a fire or an explosion. It is desirable to hold at least some of these drills in concert with the community fire, rescue and police organizations.
Conclusion
Apropriately designed and diligently practised preventive measures will do much to lower the frequency of occupational injuries and illnesses among hotel and restaurant workers. Language barriers and relatively low educational levels often represent formidable challenges to the effectiveness of training and indoctrination programmes, while the high rate of turnover dictates the frequent repetition of these programmes. It is important to remember that the health and safety of the workers in this industry is an essential element in the enjoyment and satisfaction of the patrons, upon whose good will the success - and even the survival - of the enterprise depends.
The Nature of Office and Clerical Work
Work Organization and Stress
Office and sales work are traditionally thought of as clean, easy, safe work. While life-threatening, acute injuries are rare in these fields, occupational hazards exist that diminish the quality of life and in some cases, cause serious injury and death.
Stress can be defined as a physical or psychological stimulus that produces strain or disruption of the individual’s normal physiological equilibrium. Stress reactions include headaches, gastro-intestinal and sleep disturbances, high blood pressure and other cardiovascular disease, anxiety, depression and increased use of alcohol and drugs. Work in offices and retail trades is stressful both because of the structure of the industries and because of the organization of work.
The Structure of Work
Employers are increasingly using part-time and temporary workers (“temps” or contract workers). Often, this arrangement provides the desired flexibility in working hours. But there are costs. Government labour statistics show that the average part-time worker in the United States, for example, earns only 60% as much as a full-time worker on an hourly basis. Not only are they paid less, but their benefits, like health insurance, pensions, paid sick leave and vacation, are substantially less than those received by full-time workers. Fewer than 25% of part-time workers have employer-paid health insurance, compared to nearly 80% of full-time workers. Sixty per cent of full-time workers have pensions, while only 25% of part-time workers have this coverage. In 1990 in the US, there were nearly 5 million part-time workers who would have preferred to be employed full time. Other countries are also undergoing similar transformations of work. For example, in the European Union, 15% of the workforce and roughly 20% of clerical and sales worked had part-time jobs in 1991, and 8.4% of clerical workers were temps (De Grip, Hovenberg and Willems 1997).
In addition to lower pay and few benefits, there are other negative aspects of this restructuring of work. Temps often live with the stress of not knowing when they will be working. They also tend to work more overtime because they are often hired for “crunch” periods. Neither part-time workers nor temps receive equal protection under many government laws, including occupational safety and health regulations, unemployment insurance and pension regulations. Few are represented by labour unions. A case study commissioned by the US Occupational Safety and Health Administration of contract labour in the petrochemical industry shows that contract workers get less health and safety training and have higher injury rates than non-contract workers (Murphy and Hurrell 1995). The health consequences of an increasingly non-unionized, temporary workforce should not be underestimated.
Work organization
When the well-known long-term study of heart disease, the US Framingham Heart Study, examined the relationship between employment status and the incidence of coronary heart disease, it found that 21% of women clerical workers develop coronary heart disease, a rate almost twice that of non-clerical workers or housewives. According to Karasek’s demand control model of job stress, work that is characterized by high demands and low control, or decision-making latitude, is the most stressful, because of the imbalance between responsibility and ability to respond (Karasek 1979, 1990). Occupations such as clerical work, electronics manufacturing, garment work and poultry processing are characterized by tedium, ergonomic hazards and low job control. Clerical work ranked among the most stressful in this regard.
Recognizing the social, economic and physical determinants of health effects related to occupational stressors instead of focusing solely on personal pathology is a first step in the complete and long-term management of stress-related problems. While many people may benefit from programmes that provide individual coping and relaxation exercises, workplace stress management programmes should also acknowledge the broader social and economic constraints that provide the context for the daily lives of working people.
Air Quality
Many buildings have serious indoor air pollution problems. In offices, the combination of poor ventilation design, sealed buildings and the build-up of chemicals from building materials, office machines and cigarette smoke has resulted in an office smog in many buildings. Micro-organisms (e.g., moulds, bacteria) can flourish in the air-conditioning and humidifying systems, evaporative condensers and cooling towers in many office buildings. The result may be “tight building syndrome”, which can involve a wide range of symptoms depending on the situation, including allergies and respiratory infections, such as legionnaires’ disease, that sometimes can reach epidemic proportions. Perhaps the most common office air pollutant is cigarette smoke, which can increase the level of respirable particles in the air to 5 times that of a non-smoking office. Since research has linked the cigarette smoking of a spouse with the increased lung cancer risk of a non-smoking spouse, non-smoking office workers may also be at risk.
Ergonomic Hazards
Ergonomic hazards in the retail trade have risen in recent years as new technologies and organizational structures have been introduced. The trend in retail has been towards self-service operations and towards larger retail outlets. The introduction of the electronic scanner has created shorter cycle times and increased repetitiveness. In addition, the work space is often not adapted to the new technology, and many work practices can lead to musculoskeletal stress.
Many studies and investigations have found a higher rate of cumulative trauma disorders in cashiers than in non-cashiers, and a dose-response relationship between the work and these disorders. These jobs usually require high levels of upper extremity activity, and, as a result, carpal tunnel syndrome, tendinitis and tenosynovitis are experienced by a large proportion of cashiers. General merchandise clerks have been shown to have moderate levels of wrist activity and high levels of ankle activity. The check stand design can greatly influence the cashier’s posture and movement patterns, causing awkward positions, long reaches and frequent lifts. As a result other common areas of discomfort are the neck, shoulder, elbow and back. Prolonged standing for cashiers and clerks can also lead to back pain from the compressive forces associated with the activity. Additionally, prolonged standing may cause discomfort in the legs, knees and feet, and varicose veins. Further risk to the back comes from moving stacks which can be too heavy and/or too large.
There are many other sectors within the retail trades that experience these disorders as well as many more. For example, retail floristry and hairdressing are frequently associated with skin problems such as rashes and chronic dermatitis. The most common injuries in eating and drinking establishments are lacerations and burns. Take these factors into account along with the high turnover rate of employees and the inadequate training that can occur as a consequence, and the result is a setting that is conducive to chronic pain, discomfort and eventual cumulative trauma disorders.
Office Trades
The image of white-collar work being safe and clean is often deceptive. The dramatic change in workforce characteristics where job specialization, the repetitiveness of tasks and physical demands have all increased and available work space has decreased has led to many ergonomic injuries and illnesses. The most obvious injuries are associated with safety, such as falls on slippery floors, trips over electrical cords, collisions with open file cabinet drawers and moving heavy objects such as boxes of paper and furniture. However, with the ubiquitous use of computers in offices today, a new pattern of health problems exists. The areas of the body most frequently affected by cumulative trauma disorders are the upper limbs and neck. However, prolonged visual disply unit (VDU) use can lead to inflammation in the muscles, joints and tendons of the back and legs as well. Serious wrist disorders such as carpal tunnel syndrome, tendinitis and tenosynovitis are often associated with VDU use. These conditions can result from continuous wrist extension during keyboard use or from direct mechanical pressure on the wrist from such things as the sharp edge of the desk. Disorders of the fingers may result from the numerous, rapid fine finger movements that occur during typing. Shoulders being held in a static elevated position, resulting from too high a work surface, can possibly lead to tendinitis. As is often the case, prolonged sitting, which is characteristic of VDU use, can reduce the blood circulation and increase blood pooling in the legs and feet as the soft tissue in the legs is compressed. Lower-back pain is often a disorder associated with prolonged sitting, as the compressive forces in the spine can be elevated, especially if the chair is poorly designed. Other common health effects of VDU use are eye strain and headaches from improper lighting or VDU flicker. The computer is rarely the only piece of equipment in large offices. The noise level generated by the combination of copiers, typewriters, printers, phones and the ventilation system is often higher than the 45 to 55 dBA recommended for easy office and phone conservation and can interfere with concentration and elevate annoyance and stress levels, which have been associated with heart disease.
Environmental Hazards
The leading environmental hazards related to office and retail trades are primarily concerned with the consumer society: mall development and groundwater problems related to “green fields” development. In many suburban communities in advanced industrial nations, retail trade and office development in malls threatens the viability of both downtown urban areas and open space in the suburbs. In Asia and Africa the problems are different: along with the vast, unplanned growth of urban areas has come even sharper geographic division of social classes. But in the North and in the South, some cities have become dumping grounds for the poor and disenfranchised, as shopping centres and office complexes—and the more privileged classes—have abandoned urban areas. Neither the work of the future nor the consumption possibilities associated with it are available, and the urban environment has deteriorated accordingly. The new efforts of environmental justice organizations have sharpened the discussion of urban development, living, shopping and work.
The development of offices also presents the problem of wasteful uses of paper. Paper presents a problem of resource depletion (the cutting of forests for paper pulp) and the problem of solid waste. An international campaign against chlorine has also pointed out the chemical hazards associated with paper production. The recycling of paper, however, has captured the imagination of the environmentally conscious, and the paper and pulp industry has been induced to increase production of recycled paper products, as well as to find alternatives to the use of chlorine compounds. Electronic communication and record keeping may very well pose a long-term solution to this problem.
The enormous problem of excess packaging materials is a critical environmental concern. For example, Fresh Kills landfill, New York City’s dump for residential garbage, the largest landfill in the United States, covers about 3,000 acres and receives approximately 14,000 tons of trash a day. At present, in some places, the landfill reaches 150 feet (about 50 m) deep, but is projected to go to 450 feet (about 140 m) in 10 years. This does not include commercial or industrial non-toxic waste. Much of this waste is paper and plastic, which could be recycled. In Germany, producers of goods are required to take back packaging materials. Thus, companies are strongly encouraged to reduce their own wasteful retail marketing practices.
Professionals and Managers
The workplace, especially in industrialized countries, has become increasingly a world of white-collar workers. For example, in the United States in 1994, white-collar work was done by 57.9% of the workforce, and service occupations accounted for 13.7% of the workforce. The professional occupations have moved from the fourth to the third largest occupational group (AFL-CIO 1995). Table 1 lists standard professional jobs according to the International Standard Classification of Occupations (ISCO-88). White-collar membership in national unions and organizations has grown from 24% in 1973 to 45% in 1993 (AFL-CIO 1995). Professional, managerial and technical occupational employment is expected to grow faster than average.
Table 1. Standard professional jobs
Professionals
Physicists, chemists and related professionals
Physicists and astronomers
Meteorologists
Chemists
Geologists and geophysicists
Mathematicians, statisticians and related professionals
Mathematicians and related professionals
Statisticians
Computing professionals
Computer systems designers and analysts
Computer programmers
Other computing professionals
Architects, engineers and related professionals
Architects, town and traffic planners
Civil engineers
Electrical engineers
Electronics and telecommunications engineers
Mechanical engineers
Chemical engineers
Mining engineers, metallurgists and related professionals
Cartographers and surveyors
Other architects and engineers
Life science and health professionals
Biologists, zoologists and related professionals
Pharmacologists, pathologists and related professionals
Agronomists and related professionals
Health professionals (except nursing)
Medical doctors
Dentists
Veterinarians
Pharmacists
Other health professionals
Nursing and midwifery professionals
College, university and higher education teaching professionals
Secondary education teaching professionals
Primary and pre-primary education teaching professionals
Special education teaching professionals
Other teaching professionals
Education methods specialists
School inspectors
Business professionals
Accountants
Personnel and career professionals
Other business professionals
Legal professionals
Lawyers
Judges
Other legal professionals
Archivists, librarians and related information professionals
Archivists and curators
Librarians and related professionals
Social science and related professionals
Economists
Sociologists, anthropologists and related professionals
Philosophers, historians and political scientists
Philologists, translators and interpreters
Psychologists
Social work professionals
Writers and creative or performing artists
Authors, journalists and other writers
Sculptors, painters and related artists
Composers, musicians and singers
Choreographers and dancers
Film, stage and related actors and directors
Religious professionals
Source: ILO 1990a.
One characteristic of professional office staff and managers is that their work function may require decision-making and responsibility for the work of others. Some managers or professional staff (for example, engineers, nurse administrators or social workers) may be located in industry and experience industrial hazards shared with the line staff. Others with managerial and executive functions work in buildings and offices remote from the industry itself. Both groups of administrative workers have risk from the hazards of office work: occupational stress, poor indoor air quality, chemical and biological agents, repetitive strain injuries (RSIs), fire safety concerns, sexual harassment and violence or assault in the workplace. See also the article “Offices: A hazard summary” in this chapter.
Demographic Changes
In a study of executive “hardiness” in the 1970s, not enough women could be found in executive positions to be included in the study (Maddi and Kobasa 1984). In the 1990s, women and minorities have had increasing representation in positions of authority, professional jobs and non-traditional jobs. However, a “glass ceiling” clusters most women in the lower levels of the organizational hierarchy: only 2% of senior management positions are held by women in the United States, for example.
As women enter traditionally male occupations, the question arises as to whether their experience in the workplace will result in an increase in coronary heart disease similar to that of men. In the past, women have been less reactive than men in stress hormone secretions when faced with the pressure to achieve. However, in studies of women in non-traditional roles (female engineering students, bus drivers and lawyers) a laboratory experiment showed that women had almost as sharp an increase in epinephrine secretion as men exposed to a difficult task, considerably higher than female clerical workers in traditional roles. A study of male and female managers in 1989 showed that both sexes had a heavy workload, time pressure, deadlines and responsibility for others. Women managers reported lack of communication at work and conflict between work and family as sources of stress, whereas male managers did not. Male managers reported the highest work satisfaction. The female managers were not found to have the support of a strong work network. Studies of professional women and their spouses showed child care responsibilities to be more heavily borne by women, with men shouldering chores with less time-specific demands, such as lawn care (Frankenhaeuser, Lundberg and Chesney 1991).
Although studies do not indicate that working leads to smoking, workplace stress is associated with increased smoking rates and difficulties in smoking cessation. In 1988, a higher rate of smoking was observed among female professionals as compared to male professional workers (Biener 1988). Smoking is a behavioural style of coping with stress. For example, nurses who smoked cigarettes reported higher levels of job stress than non-smoking nurses. In the Women and Health study, salaried workers were more likely to report job strain (45%) than hourly wage workers (31%), and more difficulty unwinding after work (57%) than hourly workers (35%) (Tagliacozzo and Vaughn 1982).
International changes have caused political and social restructuring that lead to large numbers of people emigrating from their country of birth. Workplace adaptation to minority groups results in more diverse workers represented in managerial positions. Implications of these changes include human factor analyses, personnel policies and diversity education. Ergonomic changes may be needed to accommodate diverse body types and sizes. Cultures may clash; for example, values regarding high productivity or time management may vary among nations. Sensitivity to such cultural differences is taught more often today as a global economy is envisioned (Marsella 1994).
New Structures of Work Organization
An increase in the use of participative techniques for input and governance of organizations, such as joint labour-management committees and quality improvement programmes, have changed the typical hierarchical structures of some organizations. As a result, role ambiguity and new skill requirements are frequently mentioned as stressors for those in managerial positions.
If the condition of managerial and supervisory work remains challenging, then the high stress/low illness individual can be described as a “hardy executive”. Such executives have been characterized as being committed to various parts of their lives (e.g., family, work, interpersonal relationships), as feeling a greater sense of control over what occurs in their lives and as regarding challenge in a positive mode. If stressful life events (e.g., staff reductions) can debilitate a worker, the model of hardiness provides a buffering or protective effect. For example, during periods of organizational change, efforts to maintain a feeling of control among workers could include increased clarity in work activities and job descriptions, and perceptions of the change as having possibilities, rather than as a loss (Maddi and Kobasa 1984).
Change in Workplace Technology
Work has altered so that in addition to the mental skills required of the professional, technological expertise is expected. The use of the computer, fax, telephone and video-conferencing, electronic mail, audio-visual presentations and other new technology has both changed the function of many managers and created ergonomic and other hazards associated with the machines which assist these functions. The term techno-stress has been coined to describe the impact of the introduction of new information technologies. In 1991 for the first time in history, US companies spent more on computing and communications hardware than on industrial, mining, farm and construction machines.
Computers affect how professional work and work processes are organized today. Such effects can include eye strain, headaches, and other VDU effects. The World Health Organization (WHO) in 1989 reported that psychological and sociological factors are at least as important as physical ergonomics in working with computers. Unintended consequences of computer use include the isolation of the computer operator, and the increase in working with computers in remote locations using high-speed modems. (See also the article “Telework” in this chapter.)
Occupational Stress
A well-known hazard is that of occupational stress, now linked to physiological outcomes, especially cardiovascular diseases. Stress is discussed extensively in several chapters in this Encyclopaedia.
A Swedish study of professional telecommunication engineers suggests that most studies of stress, which have usually been based on low- and medium-skill jobs, are not applicable to skilled professionals. In this study, three stress-reduction interventions were applied to the professional workforce with the following beneficial results: a feeling of being in control of one’s own work (thought to protect against high mental strain work); a lessening of mental strain; a lasting effect on social interactions and support; an improvement in elevated prolactin levels; a lessening of circulating thrombocytes (which may be a factor in stroke); and an improvement in cardiovascular risk indicators (Arnetz 1996).
As the human and financial costs of occupational stress have become known, many organizations have introduced initiatives that reduce stress and improve employee health in the workplace. Such interventions can focus on the individual (relaxation techniques and employee assistance programmes); on the individual-organizational interface (person-environment fit, participation and autonomy); or on the organization (organizational structures, training, selection and placement).
Violence
Managerial and professional workers are at risk for violence and assault because of their visibility and the possibility of adverse reactions to their decisions. Most commonly, violence and assault occur where money changes hands in retail settings or where troubled clients are seen. Workplaces at greatest risk for homicide (in descending order) are taxicab establishments, liquor stores, gas stations, detective services, justice and public order establishments, grocery stores, jewellery stores, hotels/motels, and eating/drinking places. Homicide in the workplace was the leading cause of occupational death for women, and the third leading cause of death for all workers in the United States from the mid-1980s to the mid-1990s (NIOSH 1993; Stout, Jenkins and Pizatella 1989).
Travel Hazards
Approximately 30 million people travelled from industrialized countries to developing countries in 1991, many of these business travellers. One-half of the travellers were US and Canadian residents, most commonly travelling to Mexico. European travellers were 40% of the total, with the majority visiting Africa and Asia. Health risks to international travellers occur when travelling to developing countries with high endemic rates of disease for which the traveller may have low levels of protective antibodies. An example is the hepatitis A virus (HAV), which is transmitted to 3 in 1,000 for the average traveller to developing countries and which increases to 20 in 1,000 people for those who travel to rural areas and were not careful with food and hygiene. Hepatitis A is a food- and water-borne disease. A vaccine is available that was introduced in Switzerland in 1992 and is recommended by the Advisory Committee on Immunization Practices for individuals travelling to areas with a high incidence of HAV (Perry 1996). Background and references for such hazards are provided elsewhere in this Encyclopaedia.
Other travel hazards include motor vehicle accidents (the highest rated cause of workplace fatality in the United States), jet lag due to diurnal disturbances, extended family absences, gastrointestinal disturbances, public transport accidents, crime, terrorism or violence. Traveller advisories for specific hazards are available from disease control agencies and embassies.
Health and Safety Interventions
Measure for the improvement of professional and managerial workers’ working conditions include the following:
- All managerial, supervisory and professional workers should be included in health and safety training on the worksite.
- Worksite smoking cessation programmes are appropriate as they are convenient, allow practice of cessation behaviours during working hours (when they are often most needed to cope with stressful events) and provide incentive to quit smoking.
- Stress- and time-management programmes lead to improved worker satisfaction and productivity.
- Diversity in the workplace will be commonplace in the coming century. Diversity training improves cross-cultural understanding.
- Female professional and managerial staff need workplace support for their demanding roles at home and in the workplace: family leave, support groups and increased opportunities for advancement and control over their work.
- Employee assistance programmes that are non-judgemental and confidential should be provided to all workers.
- Computer work hazards require organizational, environmental, equipment and training emphasis, as well as engineering improvements in workstation, monitor and remote worksite designs.
- Travellers need time to reorient to other time zones and countries, updated health information to protect them, time off to provide for family needs and security protections.
- All workers need engineering, work practice and protective equipment controls to protect against violent acts and assaults by others. Training in personal and office protection should deal with prevention, personal protection, and post-assault help and counselling.
Offices: A Hazard Summary
Office workers may perform a wide variety of tasks, including: answering the telephone; interacting with the public; handling money; receiving and delivering mail; opening mail; typing and transcribing; operating office machinery (e.g., computers, adding machines, duplicating machines and so on); filing; lifting supplies, parcels and so on; and professional work such as writing, editing, accounting, research, interviewing and the like. Table 1 lists standard clerical jobs.
Table 1. Standard clerical jobs
Clerks
Secretaries and keyboard-operating clerks
Stenographers and typists
Word-processor and related operators
Data entry operators
Calculating-machine operators
Secretaries
Numerical clerks
Accounting and bookkeeping clerks
Statistical and finance clerks
Material-recording and transport clerks
Stock clerks
Production clerks
Transport clerks
Library, mail and related clerks
Library and filing clerks
Mail carriers and sorting clerks
Coding, proof-reading and related clerks
Scribes and related clerks
Other office clerks
Cashiers, tellers and related clerks
Cashiers and ticket clerks
Tellers and other counter clerks
Bookmakers and croupiers
Pawnbrokers and money-lenders
Debt-collectors and related workers
Client information clerks
Travel agency and related clerks
Receptionists and information clerks
Telephone and switchboard operators
Source: ILO 1990a.
Office workers are often thought to have pleasant, safe environments to work in. Even though office work is not as hazardous as many other workplaces, there are a variety of safety and health problems that may be present in an office. Some of these can pose significant risks to office workers.
Some Hazards and Health Problems
Slips, trips and falls are a common cause of office injuries. Poor weather conditions such as rain, snow and ice create slip hazards outside of buildings, and inside when wet floors are not cleaned up promptly. Electrical and telephone cords placed in aisles and walkways are a common cause of trips. Carpeted offices can create trip hazards when old, frayed and buckling carpet is not repaired and shoe heels catch on it. Electrical floor outlet boxes can cause trips when they are located in aisles and walkways.
Cuts and bruises are seen in office settings from a variety of causes. Paper cuts are common from file folders, envelopes and paper edges. Workers can be injured from walking into tables, doors or drawers that have been left open and are unseen. Office supplies and materials that are improperly stored can cause injury if they fall onto a worker or are placed where a worker would inadvertently walk into them. Cuts can also be caused by office equipment such as paper cutters and sharp edges of drawers, cabinets and tables.
Electrical hazards occur when electrical cords are placed across aisles and walkways, subjecting the cords to damage. Improper use of extension cords is often seen in offices, for example, when these cords are used in place of fixed (permanently installed) outlets, have too many items plugged into them (so that there could be an electrical overload) or are the wrong size (thin extension cords used to energize heavy-duty cords). Adapter or “cheater” plugs are used in many offices. Most often they are used to connect equipment that must be grounded (three-pronged plug) into two-pronged outlets without connecting the plug to ground. This creates an unsafe electrical connection. Ground pins are sometimes broken off a plug to allow for the same two-prong connection.
Stress is a significant psychosocial health problem for many offices. Stress is caused by many factors, including noise from overcrowding and equipment, poor relationships with supervisors and/or co-workers, increase in workload and lack of control of work.
Musculoskeletal problems and soft tissue injuries such as tendinitis result from office furniture and equipment which is not fitted to a worker’s individual physical needs. Tendinitis can occur from repeated movement of certain body parts, such as finger problems from constant writing, or filing and retrieving files from cabinets that are too full. Many office workers suffer from a variety of RSIs such as carpal tunnel syndrome, thoracic outlet syndrome and ulcer nerve damage because of the ill-fitting equipment and the lack of rest breaks from continuous keying (on a computer) or other repetitive activities. Poorly designed furniture and equipment also contribute to poor posture and nerve compression of lower extremities, since many office workers sit for long periods of time; all of these factors contribute to low-back and lower-extremity problems, as does constant standing.
Continual use of computers and poor overall lighting create eye strain for office workers. Because of this, many workers experience a worsening of vision, headaches, burning eyes and eye fatigue. Adjustments in lighting and computer screen contrast, as well as frequent breaks in eye focus, are necessary to help eliminate eye problems. Lighting must be appropriate for the task.
Fire and emergency procedures are essential in an office. Many offices lack adequate procedures for workers to exit a building in case of fire or other emergency. These procedures, or emergency plans, should be in writing and should be practised (through fire drills) so that office occupants are familiar with where to go and what to do. This insures that all workers will promptly and safely evacuate in the event of a real fire or other emergency. Fire safety is often compromised in offices by blocking of exits, lack of exit signage, storage of incompatible chemicals or combustible materials, inoperative alarm or firefighting systems or total lack of adequate means of notification of workers in emergencies.
Violence
Violence in the workplace is now being recognized as a significant workplace hazard. As discussed in the chapter Violence, in the United States, for example, homicide is the leading cause of death for women workers and the third-leading cause of death for all workers. Non-fatal assaults occur much more frequently than most people realize. Office workers who interact with the public—for example, cashiers—can be at greater risk of violence. Violence can also be internal (worker against worker). The vast majority of office workplace violence, however, comes from people coming to the office from the outside. Government office workers are much more at risk for workplace violence incidents because these workers administer laws and regulations to which many citizens have hostile reactions, be they verbal or physical. In the United States, 18% of the workforce are government workers, but they constitute 30% of the victims of workplace violence.
Offices can be made safer by restricting access to work areas, changing or creating policies and procedures which help eliminate sources of hostility and provide for emergency procedures and installing security equipment which is appropriate for the particular office being improved. Measures for improving safety are illustrated in the article describing German requirements for bank teller safety.
Indoor Air Quality
Poor indoor air quality (IAQ) is probably the most frequent safety and health complaint from office workers. The effect of poor IAQ on productivity, absenteeism and morale is substantial. The US Environmental Protection Agency (EPA) has listed poor IAQ in their top 5 public health problems of the 1990s. Many reasons exist for poor air quality. Among them are closed or sealed buildings with inadequate amounts of outside air, overcrowding of offices, inadequate maintenance of ventilation systems, presence of chemicals such as pesticides and cleaning compounds, water damage and mould growth, installation of cubicles and walls which block off air flow to work areas, too much or too little humidity and dirty work environments (or poor housekeeping).
Table 2 lists common indoor air pollutants found in many offices. Office machines are also a source of many indoor air pollutants. Unfortunately, most offices have not designed their ventilation systems to take into account emissions from office equipment.
Table 2. Indoor air pollutants that may be found in office buildings
|
Pollutant |
Sources |
Health effects |
|
Ammonia |
Blueprint machines, cleaning solutions |
Respiratory system, eye and skin irritation |
|
Asbestos |
Insulation products, spackling compounds, fire retardants, ceiling and floor tiles |
Pulmonary (lung) fibrosis, cancer |
|
Carbon dioxide |
Humans’ exhaled air, combustion |
Headache, nausea, dizziness |
|
Carbon monoxide |
Automobile exhaust, tobacco smoke, combustion |
Headache, weakness, dizziness, nausea; long-term exposure related to heart disease |
|
Formaldehyde |
Urea-formaldehyde foam insulation and urea-formaldehyde resin used to bind laminated wood products such as particleboard and plywood; tobacco smoke |
Respiratory system, eye and skin irritation, nausea, headache, fatigue, possibility of cancer |
|
Freons |
Leaking air conditioning systems |
Respiratory system irritation; heart arrhythmia at high concentrations |
|
Methyl alcohol |
Spirit duplicating machines |
Respiratory system and skin irritation |
|
Micro-organisms (viruses, bacteria, fungi) |
Humidifying and air conditioning systems, evaporative condensers, cooling towers, mildewed papers, old books, damp newsprint |
Respiratory infections, allergic responses |
|
Motor vehicle exhaust (carbon monoxide, nitrogen oxides, lead particulates, sulphur oxides) |
Parking garages, outside traffic |
Respiratory system and eye irritation, headache (see carbon monoxide), genetic damage |
|
Nitrogen oxides |
Gas heaters and stoves, combustion, motor vehicle exhaust, tobacco smoke |
Respiratory system and eye irritation |
|
Ozone |
Photocopying and other electrical machines |
Respiratory system and eye irritation, headache, genetic damage |
|
Paint vapours and dusts (organics, lead, mercury) |
Freshly painted surfaces, old, cracking paint |
Respiratory system and eye irritation; neurological, kidney and bone-marrow damage at high levels of exposure |
|
PCBs (polychlorinated biphenyls), dioxin, dibenzofuran |
Electrical transformers, old fluorescent light ballasts |
Sperm and foetal defects, skin rashes, liver and kidney damage, cancer |
|
Pesticides |
Spraying of plants and premises |
Depending on chemical components: liver damage, cancer, neurological damage, skin, respiratory system and eye irritation |
|
Radon and decay products |
Building construction materials such as concrete and stone; basements |
Genetic damage, cancer, foetal and sperm damage, etc., due to ionizing radiation |
|
Solvents (methylene chloride, 1,1,1-trichloro-ethane, perchloroethylene, hexane, heptane, ethyl alcohol, glycol ethers, xylene, etc.) |
Typewriter cleaners and correction fluids, spray adhesives, rubber cement, stamp pad inks, felt-tip markers, printing press inks and cleaners |
Depending upon solvent: skin, eye and respiratory system irritation; headaches, dizziness, nausea; liver and kidney damage |
|
Sterilant gases (such as ethylene oxide) |
Systems to sterilize humidifying and air-conditioning systems |
Depending on chemical components: respiratory system and eye irritation, genetic damage, cancer |
|
Tobacco smoke (passive exposure to particulates, carbon monoxide, formaldehyde, coal tars and nicotine) |
Cigarettes, pipes, cigars |
Respiratory system and eye irritation; may lead to diseases associated with smokers |
|
Volatile organic compounds (VOCs) |
Photocopiers and other office machines, carpets, new plastics |
Respiratory system and eye irritation, allergic reactions |
Source: Stellman and Henifin 1983.
The prevalence of poor IAQ has contributed to a rise in occupational asthma and other respiratory disorders, chemical sensitivity and allergies. Dry or irritated skin and eyes are also common health complaints that can be linked to poor IAQ. Action must be taken to investigate and correct problems that are causing poor IAQ according to air quality standards and recommendations.
Dermatitis (both allergic and irritant) can be caused by many of the air pollutants listed in table 2—for example, solvents, pesticide residues, inks, coated papers, typewriter ribbons, cleaners and so forth can cause skin problems. The best solutions for office workers are identification of the cause and substitution.
More...
Bank Teller Safety: The Situation in Germany
Working in the Bank: Now Safer for the Personnel
What long-term measures can be taken to reduce the attraction of robbing a bank? The new provisions in Germany’s Accident Prevention Regulation (APR) for “Teller’s window” (VBG 120) significantly minimizes the risk to employees of being injured or killed in bank robberies.
A precise knowledge of the conduct of bank robbers is crucial. To this end, the Administration Trade Organization has been studying bank robberies since 1966. These studies have shown that, for example, bank robbers prefer small bank branches with few employees. Approximately one-third of bank robberies occur shortly after opening or just before closing. The goal is to leave the robbed bank as quickly as possible (after 2 or 3 minutes) and with the largest possible haul. Many bank robbers work under the wide-spread misconception that DM 100,000 and more can be taken from a teller’s window. The results of these and other studies are contained in the sections “Building and equipping” and “Operations” in the “Teller’s window” APR. Measures that drastically reduce the bank robbers’ expectations are proposed here to protect the employee. The success of these measures depends upon the employees strictly adhering to them in daily practice.
What basic requirements are set in the “Teller’s window” APR? In paragraph 7 of the “Teller’s window” APR, the central requirement is laid out: “Protecting the insured requires securing the banknotes so as to considerably reduce the incentive for robbery”.
What does that mean in daily practice? Easily accessible money should be kept and worked with in publicly accessible areas only within rooms separated from the public by bullet-proof or break-proof sections.
The maximum amount of accessible money allowed is given in paragraph 32: a combined maximum of DM 50,000 is allowed if there are bullet-proof tellers’ windows, other break-proof safeguards and at least 6 employees present. DM 10,000 may not be exceeded when using break-proof safeguards (but not bullet-proof tellers’ windows) in connection with containers equipped with time-staggered releases. There must be at least 2 employees present at all times, who must be in eye-contact.
To keep the incentive for bank robbery as low as possible, amounts of accessible money should be kept well below the maximums set in the “Teller’s window” APR. In addition, paragraph 25 calls for company instructions to set the maximum allowable accessible amounts for each branch. Larger amounts necessary for business and other needs should be secured in time-lock containers to make access by bank robbers more difficult.
Tellers’ windows that are not equipped with bullet-proof or break-proof safety guards and have no central money supply facility or employee-operated automatic teller machine should not have any accessible banknotes on hand.
Securing Windows and Doors
Personnel entrance and exit doors to teller areas containing cash must be secured against viewing or entering from outside, so that bank robbers cannot easily intercept employees entering and leaving bank rooms. The employee must be able to ensure, with built-in peepholes, that no danger exists.
To prevent unnoticed entrance by bank robbers into bank rooms, door closers must ensure that doors are always kept closed.
Since a considerable incentive for theft arises from viewing banknotes, windows behind which banknotes are handled must be secured against viewing or penetrating. Statistics show that holding strictly to this requirement results in very few bank robberies through windows or personnel entrances.
In contrast to personnel entrance and exit doors, doors for public traffic must have a clear view. Bank robbers can thereby be recognized early and an alarm sounded to bring assistance. Therefore it is important that the view not be obstructed by placards or the like.
Optimal Room Surveillance
In order to be able to identify the bank robber as quickly as possible, and to have effective evidence for court, optimal room surveillance equipment is prescribed in the “Teller’s window” APR. This is also important for determining whether the robber extorted money or threatened employees, since particularly brutal actions increase the penalty. Good pictures reduce the incentive to rob a bank.
The instruction “Installation directions for optimal room surveillance equipment (ORSE) SP 9.7/5” of July 1993 permitted only individual cameras as standard ORSE. Photographs are superior to video shots for identification because of greater detail recognition, resulting in better evidence. The disadvantage lies in the fact that photos are available only after the camera is triggered. Because of technical advances, the Administration technical committee now also permits the use of video cameras as possible ORSE. The corresponding instruction is now being prepared; it provides that the limited resolution of video pictures should be compensated for by using 2 views. For this, at least 2 cameras must be installed for recognizing the robber and for videotaping essential events.
Appropriate installation of the video technology can continuously record, and a “wanted” photo can thus be available without special triggering. The further advantages of the system include colour shots, quicker availability of “wanted” photos, transmission of the pictures to the police even during the robbery and the ability to constantly check the functioning of the camera.
Teller’s Window Security
The “Teller’s window” APR authorizes:
- bullet-proof and break-proof glass enclosures and tellers’ booths
- power-driven separations
- break-proof separations in connection with bullet-proof screens
- central money supply equipment
- employee-operated teller machines.
Furthermore, customer-operated teller machines support the requirements of paragraph 7, since their use can reduce the amount of money in the booth or separated room.
In order to comply with the “Teller’s window” APR, the number of employees needed at the counter and the amounts to be taken in and paid out (quantity and number) must be known before a tellers’ counter is built or remodeled. Optimal security can be achieved only when counter security corresponds to the actual flow of business.
Constant Presence with Eye contact
Certain teller security measures require a minimum of 2 to 6 employees having eye contact with each other. This requirement flows from the recognition that bank robbers prefer smaller branches with higher yields, where the tellers, when threatened with a gun, cannot withdraw behind bullet-proof shielding.
Break-proof teller shielding can be used only when 6 employees with eye contact are always present in the counter area. This does not mean a 6-person location, where not everyone is always at their workplace due to vacation, sickness, customer visits and so on. Experience shows that this condition can be fulfilled only when 8 to 10 employees work at the location. Alternatively, a floater service can possibly be used to ensure the necessary minimum number of employees.
To guarantee the constant presence of 2 employees with eye contact, the location must have 3 to 4 positions.
It is important that the facility not be opened before the required minimum number of employees are present. When consultations are taking place in adjoining rooms, the minimum number of employees at the windows must still be maintained.
Security through Separation
Small branches
“Small branches” are those where the presence of at least 2 employees with eye contact in the counter area is not ensured. For these branches, bullet-proof shielding in connection with break-proof separations offers good protection, since the employee does not have to leave the secured area in the event of a robbery. Consultations are carried on in an area protected by break-proof shielding. Good communication is possible here. The bullet-proof shield, behind which the accessible cash must be kept, should be placed so that employees cannot be threatened with a weapon from the customer area. Money transactions take place by way of a prescribed hatch or sliding drawer. Since the employee must go into the bullet-proof-secured area in the event of an attack, the necessary personal security is provided. This area must not be left under any circumstances, including while handing money over to the robber.
Bullet-proof full separation presents an alternative for 1- to 3-person teller operations. It offers mechanical protection against the typical bank robbery, since all employees are separated from the robber by bullet-proof shielding. The disadvantage here is that communication with customers is reduced in the interest of security. So full bullet-proof separation is appropriate only for small branches.
Larger branches
The teller’s booth is a form of security in which only the teller’s work station is separated from the customer area. This possibility makes sense only for teller jobs in which the teller is fully occupied by his or her work in the booth and does not have to leave it.
Before installing a booth, it is necessary to determine whether the teller is fully occupied handling money. In smaller branches with only 2 to 4 employees, this is often not the case. If the teller has other tasks outside the booth, the security requirements of the APR are not met, since the teller is supposed to always be separated from the customers for protection against bodily attack. In practice what repeatedly happens is that while the teller is performing tasks outside the booth, the door is held open with a wedge or the key is left in the lock. Thus the security of the teller’s booth is compromised, which is of great interest to potential robbers.
The bullet-proof teller’s booth does hinder communication between the teller and customers. But since longer discussions take place in unsecured workplaces anyway, this does not present a big problem. More serious problems include ensuring draft-free ventilation and air-conditioning in small teller’s booths.
For power-driven separations, a movable steel wall, built into the counter, is raised in emergencies by way of several arranged triggers in second intervals. This creates a bullet-proof separation, with the employees behind it in a secure area. To prevent a robber from entering unnoticed, it must be activated whenever there are no employees in the vault area, or when work is being done that requires personnel to turn away from the counters. In order to avoid constant activation of the steel wall, this type of security should be used only in 2- to 4-person teller areas.
Furthermore, the tellers’ workstations can be isolated with bullet-proof separations. For this, full separations for all employees as well as tellers’ booths can be installed. This form of security, however, requires the constant presence of at least 6 employees with constant eye contact in the main hall.
Bullet-proof full separation and tellers’ booths can also be used when a minimum of 2 employees are present with eye contact and the accessible cash does not exceed DM 10,000. A time-release money container is required in this case so that the teller does not constantly have to leave the secured area to restock. Bank robbers avoid teller positions where they can expect only a small amount of cash or have to wait a long time for it. In this case, notice of the time-release container at the entrance and in the tellers’ area is important for the employees’ protection. This makes immediately clear to the potential robber that the employee has no control over the container and that only a small haul can be expected.
Security without Accessible Banknotes in the Main Hall
Security is possible even without building a separation between the employees and the customer area. But for this to reduce the incentive, no accessible quantities of money can be in the tellers’ area. Money taken in must be immediately secured. The money is kept in a cash box in an area not open to the public, so it cannot be threatened by the robber. The employees receive the necessary amounts of money through a tube delivery system in the main hall. Money taken in is sent to the cash box by this means. No minimum number of employees in the main hall is prescribed in this case. This type of security, however, results in longer waiting times for customers. The advantage is that bank robbers have virtually no chance of getting anything in a robbery.
Employee-operated automatic teller machines (ATMs) are a second way to make payments with cash that is not accessible in the main hall. These, referred to by the bank as AKT-designated machines, contain 4 to 6 magazines for holding banknotes in a time-released secured container. For payments, the required amount is called up using a keyboard, with which an alarm can also be sounded in emergencies. The money is delivered to the employee after a time delay. The length of the delay depends upon the amount of money and is set in paragraph 32 of the “Teller’s window” APR. These are set so that good service is possible, but the robber is scared off by the longer waiting times for larger amounts. Cash receipts should be secured by use of time- or double-closing containers.
At least 2 employees with eye contact must be constantly present when using an employee-operated ATM. For this reason, this form of security is appropriate only for locations in which 3 to 4 employees work. Discussions can take place in a conference room only when 2 or more employees are present in the customer area during the discussion.
In the case of a technical problem in an employee-operated ATM, appropriate instructions and measures should be prepared. These should include an emergency cash box and corresponding organizational procedures to ensure that work proceeds in accordance with the “Teller’s window” APR.
Company Directives and Instructions
The employer must prepare company directives for every teller’s window and regularly check on compliance. These directives should outline the possible events during a robbery and describe what to do during and after the robbery. Furthermore, daily instructions should be given, and use of the installed security equipment should be mandated. This is especially true when larger amounts of accessible banknotes are present. Instructions should also prescribe the manner of safekeeping for other valuable objects. Employees at the windows should be instructed in these company policies at least twice a year.
The purpose of these instructions is clear—to ensure that the employees follow the requirements of the “Teller’s window” APR for their own protection, and to significantly reduce the incentive for robbing a teller’s window.
Telework
Telework—or working out of one’s home—is a growing trend in businesses internationally. This article discusses the occupational health and safety hazards of telework (from the Greek tele, meaning “far off”). The employer’s responsibility to provide safe and healthy working conditions to such employees will vary depending on the contract or understanding that exists between each teleworker and employer and on the applicable labour laws.
While telework is most widespread in the United States, where it involves over 8 million workers and accounts for 6.5% of the workforce, other countries also have significant numbers of teleworkers. There are more than 560,000 in the United Kingdom, 150,000 in Germany and 100,000 in Spain. There are over 32,000 in Ireland, which amount to 3.8% of the workforce (ILO 1997).
The growing trend toward telework arrangements can be explained by the following factors:
- business efforts to reduce the time, expense and environmental impact of commuting
- legislative efforts to reduce traffic-induced air pollution trends
- changes in technology, computerization and electronic communication that enable businesses to employ workers in disparate geographic locations
- costs of maintaining large office spaces needed to accommodate large numbers of employees
- accommodation of workers who prefer telework due to physical disability, parenting needs or other family responsibilities or other reasons
- a strategy to reduce absenteeism
- recognition that workers have varying internal cycles of productivity and creativity.
Increased productivity is another factor, as a number of studies have demonstrated that telework can result in large productivity gains (ILO 1990b).
Telework may be contracted in several ways:
- The employee works full time (or part time) at home for their employer and is entitled to all of the same benefits provided by that employer to all onsite workers.
- The employee works full time for the employer but only works out of the home during a specified number of days per week or month.
- The worker is defined as an independent contractor and does not receive benefits or equipment provided by the employer.
Health and Safety Hazards of Telework
The health and safety hazards of telework can include all of the same hazards found in conventional office environments, with several additional concerns.
Indoor air quality
Most homes are not equipped with mechanical ventilation systems. Instead, air exchanges in the home rely on natural ventilation. The effectiveness of this can depend on such factors as the type of insulation of the building and so on. Provision of a fresh supply of outside air cannot be guaranteed. If the natural ventilation is inadequate to remove sources of indoor air pollutants in the home work environment, then additional ventilation may be necessary.
Indoor air pollutants in the home environment may include the following:
- natural gas or carbon monoxide exposure from inefficient heating systems or leaky stoves
- vapours and gases from photocopiers, printers or other office machines
- ongoing passive exposure to chemicals, gases or dusts resulting from renovation or construction in the worker’s home
- exposure to the effluents of other activities if housed in a multi-use building (such as an apartment building with a nail salon, dry cleaner or fast food restaurant on the ground floor).
- exposure to radon hazards if office is located in the basement in parts of the world where radon arises from construction materials or the earth.
Fire hazards
Home electrical wiring is rarely designed to accommodate the needs of the electrical equipment typically used in telework, such as printers, copiers and other office machines. Installing such equipment without assessing the wiring limits of the dwelling could create a fire hazard. Local building codes may prohibit the adjustments necessary to accommodate increased equipment needs.
Teleworkers who rent their apartments may live in multi-unit dwellings with inadequate fire evacuation plans, blocked means of egress to fire exits or locked exit doors.
Ergonomics hazards
Home work environments often rely on the employee’s personal furnishings such as chairs, tables, shelves and other items to perform required tasks. Computer workstations in the home environment may not allow for the adjustments necessary for computer-intensive work. A shortage of adequate surface area, shelf space or storage areas may result in excessive bending, awkward postures, excessive reaching and other risk factors for cumulative trauma disorders (CTDs). Working in cold or unevenly heated environments can also contribute to musculoskeletal injuries.
Lighting
Inadequate lighting may result in awkward body postures, eye strain and visual disturbances. Task lighting may be necessary for work surfaces or document holders. Wall and furniture surfaces should be neutral with a non-glare finish. While this glare-reducing strategy is increasingly utilized in office environments, it is not yet a standard of home decoration and design.
Occupational stress
Full-time employment in the home environment deprives the worker of the interpersonal and professional benefits of continuous interaction with co-workers, colleagues and mentors. The isolation created by telework can prevent the worker from engaging in professional development activities, taking advantage of promotional opportunities and contributing ideas to the organization. Gregarious workers in particular may depend on human contact and suffer personally and professionally without it. The lack of administrative support services for employees who require clerical assistance presents an additional burden to teleworkers. The employer should make an effort to incorporate the teleworker into staff meetings and other group activities, either in person or electronically (tele-conferencing) as per physical and geographical limitations.
Employees with children, disabled family members or ageing parents may perceive distinct advantages of working at home. But attending to the needs of dependent family members can affect the concentration needed to focus on job responsibilities. The ensuing stress can negatively impact on the worker who is unable to perform to capacity in the home and fails to meet employer expectations. Telework should not be considered as a substitute for child or elder care. Since workers vary tremendously in their capacity to balance work and other responsibilities in the home environment, the need for support services must be evaluated on a case-by-case basis to prevent excessive occupational stress and subsequent loss in productivity. No worker should be required to adopt a telework arrangement against his or her will.
Injury and Illness Compensation
Occupational illnesses often occur over long periods of time from cumulative exposures. Prevention of these illnesses depends on rapid identification of risk factors, fixing the problem using a variety of methods and medical management of the affected worker when the first signs or symptoms of illness appear.
To date, employer responsibility for accidents and injuries in the home environment have been debated on a case-by-case basis. Most national occupational health and safety standards do not include formal policies addressing the safety of teleworkers. The serious impact of this trend must be carefully evaluated and addressed via international standard-setting.
When telework arrangements shift the employee’s status to that of an independent contractor, the burden of many responsibilities shift to the employee as well. Once the work is performed in the home by an independent contractor, the employer no longer feels obligated to provide a healthy and safe workplace, access to preventive and curative medical care for the worker and his or her family, social security, disability insurance and compensation for injured workers who need to recuperate. This trend eliminates worker benefits and protections that were won after decades of struggle and negotiation.
Protection for the Teleworker
The contract between the teleworker and the employer must address the overall work environment, safety and health standards, training and equipment. Employers should inspect the home workspace (at agreed-upon times) to ensure worker safety and to identify and correct risk factors that could contribute to illness or injury. The inspection should evaluate indoor air, ergonomics, trip hazards, lighting, chemical exposure and other concerns. Clear policy must be established regarding the provision of office supplies required for job tasks. Liability issues must be clearly defined regarding employer (and worker) assets that are lost or damaged due to fire, natural disaster or theft. Employees must be exempt from financial liability unless found to be negligent.
In addition, telework arrangements should be evaluated on a regular basis in order to identify workers who discover that working at home does not work for them.
Summary
The advantages of telework are extensive, and beneficial telework arrangements should be encouraged for job tasks and mature workers who will have much to gain by working at home. Telework has enabled disabled workers to achieve greater independence and seek professional opportunities not previously offered or available. In return, employers are able to retain valuable workers. However, the telework arrangement must ensure continuation of employee benefits and occupational health and safety protections.
The Retail Industry
The retail trade is the selling of goods to consumers. Enterprises sell everything from automobiles to clothing, from food to television sets. In many countries what once was an industry comprised mainly of small shops and stores, now largely consists of multinational conglomerates which own huge megastores competing for the global market. Competition and technological changes have changed job descriptions, the hazards associated with those jobs and the nature of the workforce itself.
In the developed nations, small retailers struggle to compete with large corporate retailers. In the United States, Canada and throughout the European Community and the Pacific Rim, the retail trade has moved from the city centre to suburban shopping malls. Instead of the neighbourhood “mom and pop” stores, multinational chain stores sell the same products and the same brand names, effectively limiting consumer choice of product and forcing competition out of the market by their buying power, advertising capabilities and lower prices. Many times a large store will take a loss on certain products in order to bring customers into a store; this technique frequently generates other sales.
In developing countries with predominantly agrarian economies, bartering systems and open marketplaces are still common. However, in many developing countries, the large multinational retailers are beginning to enter the retail market.
Each type of establishment has its own hazards. Retail work in developing countries and countries in transition is often very different from retail work in developed countries; conglomerates with large chain stores are not yet dominant and retail work is mainly conducted in an open-air market, in all types of weather.
There is a trend among multinational conglomerates to try and change employment conditions: trade unionism is discouraged, staff is reduced to a bare minimum, wages go down, stores predominantly hire part-time workers, the average age of the workforce is lowered and benefit packages diminish.
Throughout the world store opening hours have changed so that some establishments even remain open 24 hours a day, 7 days per week. In the past, a worker who worked late at night or on a holiday received extra compensation; now, premium pay for working those hours has been taken away as such long hours become the norm. In the US, for example, traditional holidays are now negotiable when the store stays open on a 24-hour, 7-day basis.
The changes in the nature of how business is conducted has forced several fundamental changes in the workforce. Since many jobs have been marginalized to part-time work, the jobs themselves require little skill and workers receive no training. Workers who once saw a career in retail work, now find themselves changing jobs frequently or even leaving the field of retail work, which has become short term and part time.
The size of the workforce in the retail industry is difficult to estimate. The informal sector plays a significant role in developing countries (see “Case Study: Outdoor Markets”). Many times, health and safety problems go unnoticed, are not recorded by government and are considered to be part of the job.
In many of the countries that do keep statistics, retail, wholesale and restaurant and hotel workers are grouped into one category. Statistics from around the world show that the percentage of people who work in the wholesale, retail, restaurant and hotel trades ranges from over 20% in some countries in Asia to less than 3% in Burkina Faso (see table 1 ). Although men outnumber women in the labour force, the percentage of women in the retail industry is higher in at least half of the countries for which statistics are available.
Table 1. Labour statistics in the retail industry (selected countries)
|
Country |
Men in the labour force (%) |
Men in |
Women in the labour force (%) |
Women in |
Total population in |
Total number |
Injured people |
|
Burkina Faso |
51.3 |
1.0 |
48.7 |
1.5 |
2.6 |
1,858 |
8.71 |
|
Costa Rica |
69.9 |
11.0 |
30.1 |
7.4 |
18.4 |
156,782 |
7.02 |
|
Egypt |
75.9 |
7.3 |
24.1 |
1.2 |
8.4 |
60,859 |
2.52 |
|
Germany |
52.3 |
4.5 |
47.7 |
7.0 |
11.5 |
29,847 |
20.13 |
|
Greece |
63.0 |
10.9 |
37.0 |
7.0 |
17.0 |
23,959 |
10.54 |
|
Italy |
63.1 |
11.7 |
36.9 |
6.9 |
8.6 |
767,070 |
8.15 |
|
Japan |
59.5 |
11.0 |
40.5 |
10.9 |
21.9 |
2,245 |
9.7 |
|
Mexico |
69.1 |
10.8 |
30.9 |
9.6 |
20.5 |
456,843 |
16.96 |
|
Netherlands |
58.9 |
9.1 |
41.1 |
8.0 |
17.1 |
64,657 |
16.5 |
|
Norway |
54.5 |
7.9 |
45.5 |
8.9 |
16.7 |
26,473 |
5.0 |
|
Singapore |
59.8 |
13.2 |
40.2 |
9.0 |
22.0 |
4,019 |
0.27 |
|
Sweden |
52.0 |
6.8 |
48.0 |
6.5 |
13.3 |
43,459 |
6.6 |
|
Thailand |
55.5 |
5.8 |
49.5 |
6.8 |
12.6 |
103,296 |
3.18 |
|
United Kingdom |
56.2 |
8.3 |
43.8 |
9.5 |
17.8 |
157,947 |
11.09 |
|
United States |
54 |
11.1 |
46.0 |
10.0 |
21 |
295,340 |
23.610 |
1 Including commuting accidents; including occupational diseases.
2 Including commuting accidents; establishments employing 100 or more workers.
3 The series related to the territory of the Federal Republic of Germany before 1990;
including commuting accidents.
4 Including occupational diseases;.including non-fatal cases without lost workdays.
5 Including commuting accidents; persons losing more than three workdays
per period of disability.
6 Including non-fatal cases without lost workdays.
7 Including commuting accidents; including occupational diseases;
including non-fatal cases without lost workdays.
8 Including commuting accidents.
9 Employees only; excluding traffic accidents; year beginning April, 1993.
10 Including occupational diseases.
Sources: Country reports: Costa Rica 1994; Greece 1992, 1994; Mexico 1992, 1996; Singapore 1994, 1995; Thailand 1994, 1995; Euro-FIET Commerce Trade Section 1996; ILO 1994, 1995; Price Waterhouse 1991.
Operations, Hazards and Prevention
Cashiers
Many cashiers work at mechanized registers that require them to punch a keypad thousands of times per day to ring up the price of the article. The key punching is usually done with the right hand while products are moved from in front of the cashier to the rear of the cashier for packaging with the left hand. These work activities frequently involve poorly designed workstations, causing cashiers to lift heavy products, reach extensively for products and frequently twist the body in order to move products from one area to another. This job function places different burdens on each side of the body, causing lower-back pain, upper-extremity illnesses and repetitive-motion illnesses including tendinitis, carpal tunnel syndrome, tenosynovitis, thoracic outlet syndrome and hip, leg and foot problems.
Well-designed workstations, with automatic scanners, flexible work height conveyors, lowered bagging stations, extra personnel to bag the products and flexible seats (so that cashiers can sit to relieve lower-back and leg pressures) help eliminate upper- extremity pressures, strains and twisting motions.
Lasers
Bar-code readers and hand-held scanners in supermarkets are generally Class 2 lasers, which produce infrared radiation in the wavelength range of 760 to 1,400 nm; they are considered nonhazardous unless there is prolonged viewing of the laser beam. A laser produces a high-intensity light which can damage the retina of the eye. The eyes are vulnerable to heat, have no heat sensors and do not dissipate heat efficiently. Recommended safe practices should include, at a minimum, training workers about the hazards of looking into the beam of light and the damage to the eye that can result. Baseline eye examinations should be included in a worker protection programme to ensure that no damage has occurred.
Clerks
Retail clerks move large quantities of product from trucks to the loading dock and then to the shelves in the sales area of the store. Products come packaged in cartons of various weights. Manually unloading trucks and moving the product cartons to the front of the store may cause musculoskeletal problems. Pricing the items and placing them on the shelves puts tremendous pressure on the back, legs and neck. Using a pricing gun can cause carpal tunnel syndrome and other RSIs by putting excessive and repeated strain on the wrist, fingers and palm of the hand. Opening cartons with a knife or blade can lead to cuts on the hands, arms and other parts of the body. Cutting through cardboard with a dull knife requires extra pressure, which puts extra strain on the palms of the hands.
Mechanical lifting aids, such as fork-lift trucks, manual high-low trucks, dollies and carts help move items from one part of the store to another. Tables, scissor jacks and movable carts can help bring the items to a good height and help clerks place product on the shelves without back strain from lifting and twisting. Automated pricing guns or packaged goods already labelled will prevent wrist and upper extremity strains from repeated motions. Sharp knives will prevent forceful motions when opening cartons.
Meat cutters and delicatessen workers
Meat cutters and delicatessen workers work with saws, grinders, slicers and knives (see figure 1). When machine blades are not guarded, get jammed or become loose, fingers can be severed, cut, crushed or bruised. Machines must be securely anchored to the floor to prevent tipping and moving. Blades must be kept free of debris. If a machine is jammed, wooden devices should be used to unjam the machine with the power off. No machines should be unjammed with the power still on. Knives should be kept sharp to avoid problems in the wrists, hands and arms. The handles of knives, cleavers and clubs should be kept clean and unslippery.
Figure 1. Small-scale manual cutting of dried meet for local sale, Japan, 1989
L. Manderson
When meat is mechanically weighed and packaged on a styrofoam tray in a plastic film sealed with a heating element, vapours and gases from the heated plastic may cause “meat wrapper’s asthma” and eye, nose and throat irritation, difficulty in breathing, chest pains, chills and fever. Local exhaust ventilation (LEV) should be placed near the heating element so that these vapours are not breathed in by workers, but are vented outside the workplace.
Meat cutters enter and leave freezers many times during the day. Work clothing should include heavy clothing for freezer work.
Floors and walkways can become slippery from meat, grease and water. Slips, trips and falls are common causes of injury. All waste material must be carefully discarded and kept off walking surfaces. Walking and standing mats must be cleaned daily or whenever they become soiled.
Chemical exposures
Retail workers are increasingly exposed to hazardous chemicals in cleaning products, pesticides, rodenticides, fungicides and preservatives. Hardware store workers, automotive distributive workers and others are potentially exposed to hazardous chemicals because of the stock of paints, solvents, acids, caustics and compressed gases. The hazardous or toxic chemicals vary depending on the nature of the products that are stocked in each establishment. These can include materials not necessarily considered hazardous. Department store workers, for example, can develop sensitivities and allergies to perfumes that are sprayed as demonstrations.
Cleaning products that are used to clean surfaces in supermarkets and other retail establishments may contain chlorine, ammonia, alcohols, caustics and organic solvents. These products may be used by cleaning crews during the night shift, in stores without natural ventilation and when the mechanical ventilation system is not working at full capacity. These chemical products affect the body when used in the workplace in industrial strengths and amounts. Chemical safety information must be readily available in the workplace for workers to read. Chemical containers must be labelled with the name of the chemical and how the product affects the body, as well as which protective equipment must be used to prevent illness. Workers need to be trained about the health hazards associated with the use of chemicals, how the chemicals enter the body and how to avoid exposure.
Retail workers who set up shop on the street are exposed to exhaust from motor vehicle traffic, as are the back-of-the-store workers who inhale exhaust from idling delivery trucks in the truck bays. The incomplete combustion products in motor vehicle exhaust include, among other things, carbon monoxide and polycyclic aromatic hydrocarbons. Exhaust gases and particulates affect the body is several ways. Carbon monoxide causes dizziness and nausea and acts as an asphyxiant, limiting the blood’s ability to use oxygen. Delivery trucks should turn off their engines while unloading. Mechanical general exhaust ventilation may be needed to vent the contaminated air away from workers. Routine scheduled maintenance and cleaning is needed to maintain the ventilation system.
Formaldehyde is frequently used on clothing and other textiles to prevent mildew. It can affect those who breathe it in. In stores with larger stocks of clothing and textiles without adequate natural or mechanical ventilation systems, formaldehyde gas can build up and irritate the eyes, nose and throat. Formaldehyde can cause skin and respiratory irritation and allergies and is considered a probable carcinogen.
Pesticides, rodenticides and fungicides are frequently used to keep vermin out of establishments. They can affect the nervous, respiratory and circulatory systems of human beings as well as insects, rodents and plants. It is important not to spray chemicals indiscriminately when people are present and to keep people away from sprayed areas until it is safe to enter them again. The pesticide applicator must be trained in safe work methods before pesticides are applied.
“Tight” buildings—those without windows that can open and without natural ventilation—are dependent on mechanical ventilation systems. These systems must provide an adequate exchange of air within the space and must include adequate fresh outdoor air. The air must be heated or cooled depending on the ambient temperature outside.
Sanitation
Personal hygiene is important in the retail industry, especially when employees handle food, money and hazardous chemicals. Toilets and washing and drinking facilities must be sanitary and available in areas where employees can use them while on duty. Facilities must have clean running water, soap and towels. Employees must be encouraged to wash their hands thoroughly after using the toilet and before returning to work. Clean, cool drinking water should be available throughout the work area. Good housekeeping is necessary to prevent vermin and accumulation of garbage. Trash should be picked up on a regular basis.
Sanitation facilities are difficult to maintain in open-air markets, but an attempt must be made to provide toilets and washing facilities.
Weather
In open-air markets, retail workers are exposed to the elements and subject to the problems relating to heat and cold. In supermarkets, cashiers often work at the front of the store close to the doors that the public uses to enter and exit, exposing cashiers to hot and cold air drafts. Air shields in front of the doors that go to the outside will help block drafts and keep the air temperature at the cash register consistent with the rest of the store.
Fire prevention
There are many fire hazards in retail stores, including locked or blocked exits, limited entry and exits, combustible and flammable materials and faulty or temporary electrical wiring and heating systems. If workers are required to fight a fire, they must be trained in how to call for help, use fire extinguishers and evacuate the space. Fire extinguishers must be of the appropriate type for the type of fire and must be inspected regularly and maintained. Fire drills are necessary so that workers know how to get out of the facility during an emergency.
Stress
A new trend in retail work, when the establishment is owned by a large conglomerate, is to change full-time work to part-time work. Many large retail stores are now staying open 24 hours per day, and many stay open every day of the year, forcing workers to work “unsocial” hours. Disruption of the internal biological clock which controls natural physical phenomena such as sleep, causes symptoms such as sleepiness, gastro-intestinal disturbances, headaches and depression. Changing shifts, working on holidays and part-time work cause emotional and physical stress on the job and at home. “Normal” family life is severely compromised and meaningful social life is restricted.
Late night hours are more and more prevalent, increasing the feeling of insecurity about personal safety and the fear of robberies and other types of violence on the job. In the United States, for example, homicide is a major cause of death on the job for women, with many of these deaths occurring during robberies. Handling money or working alone or during late night hours should be avoided. A regular review of security measures should be part of a violence prevention and security programme.
Part-time pay, with few or no benefits, increases job stress and forces many workers to find additional jobs in order to support their families and maintain health benefits.
Case Study: Outdoor Markets
The informal sector accounts for between 20 and 70% of the urban workforce in developing countries (with the average being 40%); and the traders and hawkers of outdoor markets comprise a significant portion of this sector. Such work is by its very nature precarious. It involves long hours and low pay. Average earnings may not total 40% of levels found in the formal sector. Not only do many workers in outdoor markets lack permanent locations to conduct their business, they also may be compelled to do without supporting infrastructural facilities. They do not enjoy the same legal protection or social insurance as workers in the formal sector and are subject to harassment. Occupationally related morbidity and mortality rates generally go unrecorded (Bequele 1985).
Figure 1. Outdoor food market in Malatia, Solomon Islands, 1995
C. Geefhuyson
Workers in outdoor markets in both developing and developed countries, such as those shown in figure 1 and figure 2 , are exposed to numerous health and safety hazards. They are exposed to exhaust from motor vehicles, which contains such things as carbon monoxide and polycyclic aromatic hydrocarbons. Workers are also exposed to the weather. In tropical and desert locations they are subject to heat stress and dehydration. In cooler climates they are exposed to freezing temperatures, which can cause problems such as numbness, shivering and frostbite. Workers in outdoor markets may not have access to adequate hygiene facilities.
Figure 2. Heavy baskets of sea urchins being distributed by a small operator-owner, Japan, 1989
L. Manderson
The informal sector generally and outdoor markets specifically involve child labour. Roughly 250 million children are engaged in full- and part-time work around the world (ILO 1996); street traders are the most visible child workers. Children who work, including street traders, typically are denied education and often are forced to perform tasks, such as lifting heavy loads, which can result in permanent disabilities.
" DISCLAIMER: The ILO does not take responsibility for content presented on this web portal that is presented in any language other than English, which is the language used for the initial production and peer-review of original content. Certain statistics have not been updated since the production of the 4th edition of the Encyclopaedia (1998)."